Claim denial occurs when a payer refuses reimbursement after claim adjudication. It happens when the claim fails to meet coverage, coding, medical necessity, or documentation requirements. Unlike claim rejections, denials occur after review and require correction, resubmission, or a formal appeal to receive payment.
The most common denial reasons include incorrect or incomplete CPT, ICD-10, or HCPCS coding, eligibility or coverage issues, and missing prior authorization. Errors in modifiers, inactive insurance, non-covered services, or failure to obtain pre-approval frequently result in non-payment from commercial or government payers.
To avoid claim denials, you should verify patient eligibility and benefits before service. Ensure accurate coding supported by clear clinical documentation. Use claim scrubbing tools to catch data errors. Monitor denial trends and payer-specific codes regularly to correct root causes and reduce recurring revenue cycle losses.
Table of Contents
ToggleWhat is Claim Denial?
Claim denial is a payer’s refusal to reimburse a submitted medical claim after it has been reviewed. The denial occurs when the claim does not meet insurance requirements related to coverage, coding accuracy, medical necessity, authorization, or documentation. It requires a correction or an appeal for payment.
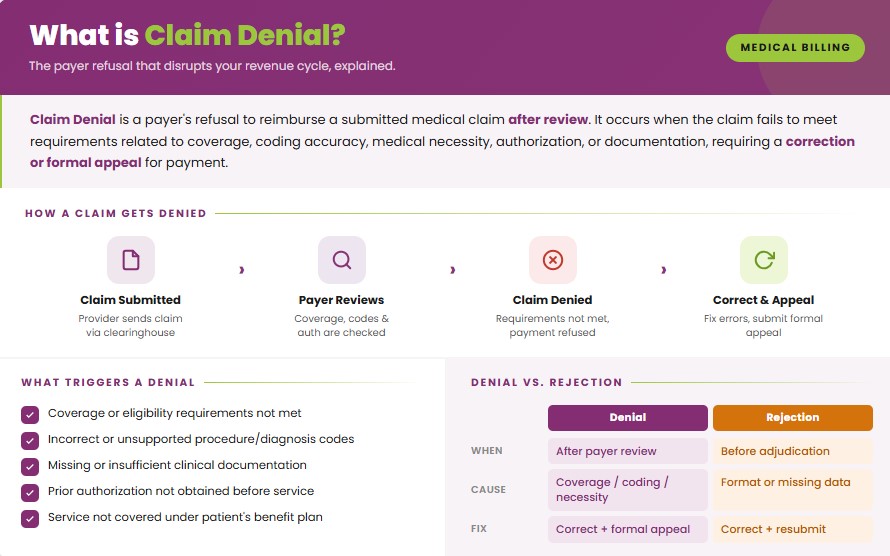
What are the Reasons for Claim Denials?
Claim denials occur due to errors in patient information, eligibility, medical necessity, coding, duplicate submissions, missing authorizations, late filing, non-covered services, coordination of benefits, provider credentials, or insufficient documentation. Each factor can block timely reimbursement of the claim.
Identifying these reasons helps practices address errors before they happen. Understanding the common causes of denial is crucial for reducing payment delays. The following sections explain the most common reasons for claim denials and how each issue can affect claim processing and reimbursement.

Missing or Incorrect Patient Information
Missing or incorrect patient information causes claim denials when payer records do not match submitted insurance details. Patient name, date of birth, address, gender, member ID, and policy number must exactly match the insurance record.
Patient demographics should be verified against a government ID and the insurance card during registration. Staff should confirm the member ID, policy number, group number, and payer name to prevent eligibility mismatches during claim processing.
All information entered into the practice management system must be double-checked for data entry errors. Staff should also review patient intake forms, consent forms, and authorization documents to ensure they are complete and up to date.
Eligibility and benefits verification should be performed before the visit or at check-in. This step confirms active coverage, plan limitations, and payer requirements, which helps prevent claim denials later in the billing process.
Eligibility and Coverage Issues
Eligibility and coverage issues cause claim denials when services are billed for inactive insurance, non-covered benefits, or incorrect payer information. Insurance coverage must be verified before services are provided to ensure the patient’s policy is active on the date of service.
Staff should review benefit details to confirm that the planned procedure is included in the patient’s policy. This includes checking service limitations, covered procedures, and plan requirements that may affect reimbursement.
Provider network status should also be verified. If the provider is out-of-network, the patient must be informed about possible higher out-of-pocket costs before services are provided.
Coverage caps, waiting periods, and excluded services should be identified during eligibility verification. Billing teams should also confirm primary and secondary insurance using coordination of benefits (COB) rules to prevent claim processing errors and payment delays.
Lack of Medical Necessity
Lack of medical necessity is a situation in which documentation does not justify why a service or procedure was required. Payers deny claims when clinical records fail to indicate that the service was appropriate for the patient’s condition.
Clinical documentation must include complete physician notes, test results, and a clear treatment plan supporting the service provided. These records must explain the patient’s diagnosis, symptoms, and clinical findings.
Diagnosis codes should also directly support the billed procedures. The selected ICD-10 code should indicate why the service was medically required according to payer guidelines.
Billing teams should review payer-specific medical policies before submission. Documentation and coding must align with payer coverage rules and reimbursement criteria to prevent medical necessity denials.
Coding Errors
Coding errors occur when procedure or diagnosis codes are incorrect, outdated, or inconsistent with the documented service. Accurate selection of CPT, ICD-10-CM, and HCPCS codes must follow official coding guidelines and reflect the services performed.
Codes should represent the correct level of service based on clinical documentation. Incorrect code selection or overcoding can lead to denials, compliance issues, or payer audits.
Billing teams must follow bundling rules and avoid billing services separately when they are included in a comprehensive procedure code. Incorrect unbundling often triggers claim denials. Modifiers should be applied only when required to clarify services. Using the latest coding manuals and payer policy updates helps maintain compliance and accurate reimbursement.
Duplicate Claims
Duplicate claims occur when the same service is submitted more than once to the payer. This often happens when a claim is resubmitted without confirming its processing status, which leads to automatic denials or rejections.
Billing teams should verify claim status through payer portals or clearinghouse reports before resubmitting. Monitoring transmission logs and claim reports helps identify whether a claim has already been sent or processed.
Clear communication between billing staff and defined claim tracking workflows helps prevent redundant submissions. Quality control checks should also be applied to both manual and electronic claim processes to detect duplicate entries before submission.
Authorization or Referral Issues
Authorization or referral issues occur when required payer approvals are not obtained before services are provided. Many procedures require pre-authorization, and failure to secure it before the date of service can lead to claim denial.
Billing teams must request authorization in advance and track approval timelines based on payer deadlines. Authorization numbers, approved services, and service dates should be recorded accurately.
Referral forms must be verified to confirm referring provider details, service scope, and payer requirements. Staff should also monitor referral validity dates and renew them when necessary. The services performed must match the services approved by the payer. Any difference between authorized and billed procedures can result in claim denial.
Timely Filing Limit Exceeded
Timely filing denials occur when a claim is submitted after the payer’s allowed submission deadline. Each insurance payer sets a specific filing limit, and claims submitted after this period are automatically denied. Billing teams should maintain an updated payer list that tracks timely filing limits for each insurance plan. This helps to ensure claims are submitted within the required timeframe.
Efficient charge entry, coding, and claim submission workflows are necessary to prevent delays. Late claim submission can also limit or eliminate appeal rights under payer policies. Payment delays in primary payers can affect timely filing for secondary or tertiary payers. Billing teams must monitor claim timelines to prevent downstream denials.
Non-Covered or Excluded Services
Non-covered or excluded service denials occur when a billed procedure is not included in the patient’s insurance benefits. Coverage verification must be performed before services are provided to confirm that the treatment is eligible for reimbursement.
Billing teams should review payer medical policies to determine whether a procedure is classified as experimental, investigational, or excluded. These classifications often result in automatic denial.
Insurance plans may also include exclusions, coverage caps, and service limitations. Staff must review these details and track service utilization to ensure treatments do not exceed payer frequency restrictions.
Certain services, such as cosmetic or elective procedures, may be excluded under the patient’s plan. Confirming these exclusions in advance helps prevent non-covered claim denials.
Coordination of Benefits (COB) Issues
COB issues occur when the order of benefits between multiple insurance plans is incorrect or not properly documented. Identifying primary and secondary payers is essential before claim submission to prevent denials or delayed payments.
All active insurance policies should be collected and verified during patient registration. COB data must be maintained across claims and payer records to avoid conflicts.
Primary payer adjudication should be monitored, and secondary claims should be submitted promptly with the required Explanation of Benefits (EOB). Regular confirmation of coverage updates ensures billing reflects active and accurate policies.
Provider Credentialing Problems
Provider credentialing problems occur when a provider is not properly enrolled, ineligible, or incorrectly listed with a payer. Claims submitted without active enrollment or valid credentials are often denied.
Active provider enrollment must be verified with each payer before claim submission. Licensure, certifications, and revalidation deadlines should be monitored to maintain billing eligibility.
Provider identification, role, and taxonomy codes must match payer records and accurately reflect the provider’s specialty. Confirming in-network status helps prevent reduced reimbursement or out-of-network denials.
Insufficient Documentation
Insufficient documentation denials occur when claims lack the necessary medical records to support billed services. Payers require complete and accurate documentation to validate medical necessity and coding accuracy.
All physician and provider notes should be complete, legible, and available to support claims. Patient progress notes, treatment plans, and test results must substantiate the services billed.
Each billed procedure must be backed by documentation that aligns with diagnosis and procedure codes. Cross-checking clinical notes against coding ensures accuracy and helps prevent denials due to missing or incomplete records.

What Are The Tips To Avoid Claim Denial?
Tips to avoid claim denials are practical steps that ensure claims are accurate, complete, and compliant before submission. Following these tips reduces errors, prevents delays, and improves reimbursement for practices.

Key tips include:
- Verify Patient Eligibility in Advance
- Obtain Prior Authorization
- Ensure Accurate Patient Information
- Improve Coding Accuracy
- Submit Claims on Time
- Maintain Complete Documentation
- Monitor Claim Status Regularly
- Prevent Duplicate Claims
- Stay Updated on Payer Policies
- Conduct Internal Audits and Staff Training
Verify Patient Eligibility in Advance
Verifying patient eligibility in advance prevents claim denials related to inactive or incorrect insurance coverage. Eligibility should be checked before services are provided to confirm that the patient’s plan is active and covers the procedures.
Staff should find out how much the patient needs to pay, including copays, deductibles, and coverage limits, to avoid unexpected denials or billing disputes. Provider network status must also be confirmed to ensure the service is in-network, reducing patient out-of-pocket costs and payer rejections.
Standardized workflows for eligibility verification should be implemented at registration or pre-service scheduling. This includes confirming policy details, coverage dates, and required authorizations to ensure claims are submitted with accurate insurance information.
Obtain Prior Authorization
Prior authorization ensures that procedures or treatments requiring payer approval are approved before services are rendered. Determine which services need prior approval by reviewing payer-specific medical policies and coverage guidelines.
Collect and submit necessary forms, clinical notes, and supporting documentation to the payer. Authorization requests should be tracked, and follow-ups conducted to confirm approval before the scheduled service.
Services should not be performed without confirmed prior authorization, as this often leads to claim denials. Appointment scheduling should be coordinated only after the payer has approved the service to ensure timely reimbursement.
Ensure Accurate Patient Information
Accurate patient information prevents claim denials caused by mismatched or incomplete data. Correctly capturing patient name, date of birth, address, and contact details during registration is essential.
Policy numbers, group IDs, and payer information must be verified before services are rendered. Keeping patient demographics and insurance data up to date reduces errors that could delay reimbursement.
Entries should be checked at registration, and patient and insurance information should be confirmed against payer databases or portals. These steps ensure that claims are submitted with accurate, verifiable information.
Improve Coding Accuracy
Accurate coding prevents denials caused by incorrect or inconsistent procedure and diagnosis codes. Codes must be selected according to official CPT, ICD-10-CM, and HCPCS guidelines.
Modifiers should be applied correctly to clarify service specifics without triggering rejections or audits. Code selection must reflect the level and complexity of the services provided.
Yearly updates to CPT, ICD, and HCPCS codes should be reviewed to maintain compliance. Codes must be cross-checked against clinical notes, test results, and procedures to ensure alignment and prevent claim denials.
Submit Claims on Time
Submitting claims on time prevents automatic denials due to missed payer deadlines. Each insurance plan has specific timely filing limits that must be observed.
Outstanding claims should be regularly reviewed, and submission timelines tracked to ensure prompt filing. Streamlined workflows for charge entry, coding, and claim submission help avoid delays.
Effective communication between clinical and billing staff ensures that documentation is complete and ready for timely claim preparation. Proactive measures, such as scheduling submissions within payer deadlines, prevent denials that cannot be appealed.
Maintain Complete Documentation
Maintaining complete documentation prevents denials caused by missing or insufficient records. Every service billed should be supported with clinical notes, test results, and treatment plans.
Clinical notes must be cross-checked against procedure and diagnosis codes to ensure accuracy and alignment with the services provided. Missing or inadequate documentation can lead to claim rejection or delayed reimbursement.
Documentation should follow standards specific to each medical specialty. Adhering to these requirements ensures claims meet payer expectations and reduces the risk of denials.
Monitor Claim Status Regularly
Regularly monitoring claim status helps identify processing issues and prevent denials. Claims should be tracked in real time to stay updated on submission, review, and adjudication progress.
Rejected claims must be quickly identified, corrected, and resubmitted to avoid delays in reimbursement. Timely appeals should be initiated when necessary to recover payments.
Collaboration between billing, clinical, and coding staff ensures that documentation or coding discrepancies are resolved promptly. This coordinated approach reduces errors and accelerates claim resolution.
Prevent Duplicate Claims
Preventing duplicate claims avoids denials caused by resubmitting the same service multiple times. The current status of each claim should be verified before any resubmission.
Billing teams should identify duplicates generated by software or clearinghouse systems. Workflow strategies must prevent multiple staff members from submitting the same claim unintentionally.
All submitted claims should be tracked in detail, including submission dates, reference numbers, and payer responses. This ensures accuracy, prevents redundant submissions, and reduces delays in reimbursement.
Stay Updated on Payer Policies
Staying updated on payer policies prevents claim denials due to outdated rules or coding practices. Regularly review payer updates, CPT/ICD code revisions, and prior authorization requirements.
Each payer’s rules, exceptions, and unique claim requirements should be evaluated to ensure compliance. Internal processes must be modified to align with new regulations and coverage guidelines.
All relevant staff should be informed of changes through training sessions, team meetings, or official memos. Keeping the team updated ensures consistent, accurate claim submissions and reduces denials.
Conduct Internal Audits and Staff Training
Regular internal audits help identify errors and gaps in submitted claims and supporting documentation. Claims should be reviewed for accuracy, completeness, and compliance with payer requirements.
Analyzing denial trends allows practices to pinpoint recurring errors in coding, documentation, or billing workflows. This insight guides corrective actions to prevent future denials.
Staff training should focus on proper coding, documentation, eligibility verification, and claim submission procedures. Feedback loops and corrective measures improve overall revenue cycle performance and increase claim acceptance rates.

What Is The Process Of Claim Denial Appeal?
The process of claim denial appeal is a structured approach to challenge a payer’s rejection and receive reimbursement for a valid claim. The steps of the claim denial appeal include:
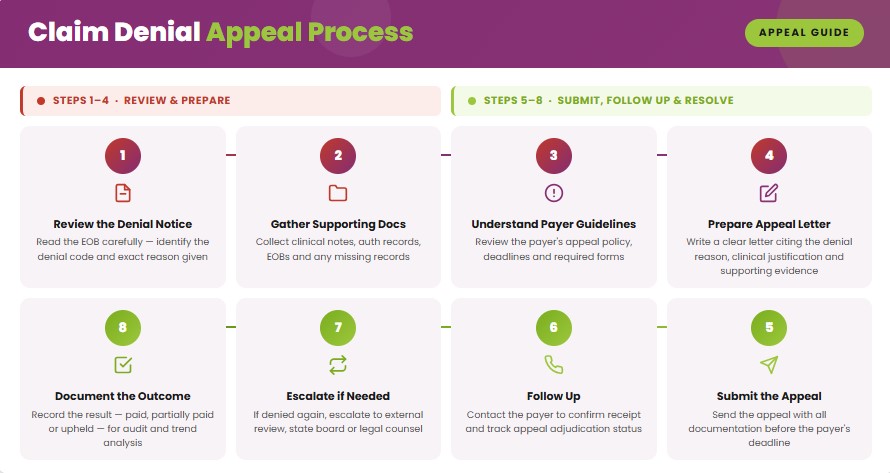
- Review the Denial Notice
Review the payer’s denial notice to identify the exact reason for the rejection. Check denial codes, EOB details, and payer notes to identify the cause of the issue. - Gather Supporting Documentation
Collect all relevant documents needed to justify the claim. These include medical records, physician notes, prior authorization confirmations, or referral documentation. - Understand Payer Guidelines
Review the payer’s appeal policies, deadlines, and submission requirements. Each payer has specific timelines, forms, or documentation that must be followed. - Prepare the Appeal Letter
Draft a clear appeal letter explaining why the claim should be reconsidered. The letter should reference the denial reason with supporting clinical or coding justification. - Submit the Appeal
Send the appeal through the payer’s designated channel, which may include an electronic portal or certified mail. Ensure all required forms and documents are included. - Follow Up
Monitor the appeal status regularly to confirm it has been received and is under review. Timely follow-ups with the payer help to prevent the appeal from being delayed. - Escalate if Needed
If the initial appeal is denied, consider escalating the case through a second-level appeal, peer-to-peer review, or an external review, depending on the payer’s policies. - Document the Outcome
Record the appeal result in the practice’s billing or revenue cycle management system. Tracking helps identify denial patterns and improves claim submission accuracy.
How Claim Denials Impact the Medical Billing Process?
Claim denials affect the medical billing claim process by disrupting reimbursement timelines and increasing operational workload for billing teams. Claim denials result in:
- Delays in Payment
- Increased Administrative Work
- Revenue Loss
- Impact on Accuracy and Compliance
- Slower Revenue Cycle
- Strain on Provider-Patient Relations
What Is The Difference Between Claim Denial And Claim Rejection?
The main difference between a claim denial and a claim rejection is the stage at which the claim is refused. A claim rejection occurs before claim adjudication due to formatting errors, missing data, or invalid information, and it can be corrected and resubmitted immediately. A claim denial occurs after the payer reviews the claim and determines it does not meet coverage, coding, or medical necessity requirements, often requiring correction or a formal appeal.
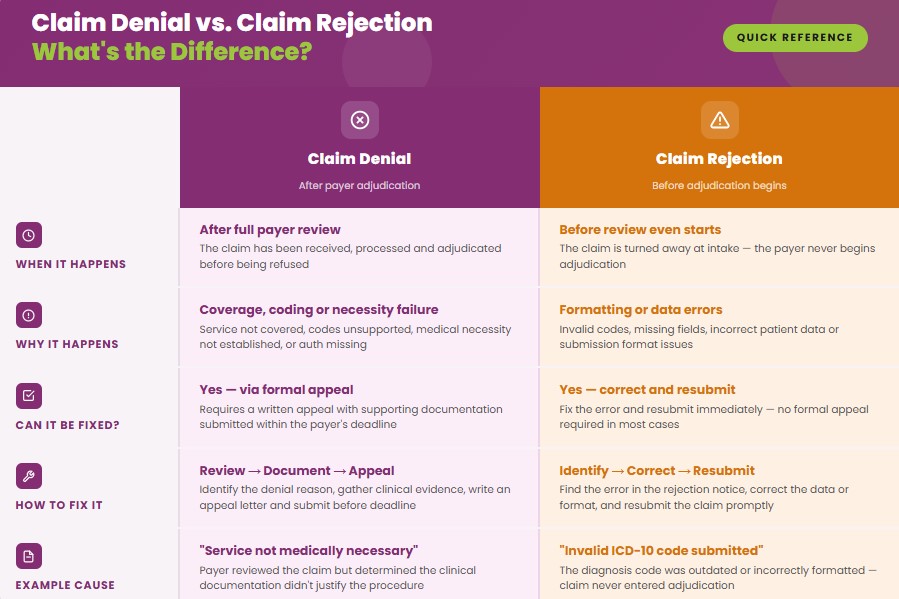
What Is The Rate Of Claim Denial?
The claim denial rate is typically estimated between 5% and 10% of all submitted medical claims, depending on the healthcare specialty, payer mix, and billing processes. It represents the percentage of insurance claims rejected by payers after submission and adjudication. The rate is calculated by dividing the number of denied claims by the total number of claims submitted within a specific period.
Monitoring denial rates is essential for maintaining strong revenue cycle performance, stable cash flow, and efficient billing operations. High denial rates indicate workflow issues, coding errors, or documentation gaps.
The impact of denials is both operational and regulatory. Operationally, denials increase administrative workload and delay reimbursement. From a regulatory perspective, accurate billing, documentation, and compliance with payer policies are required to meet payer rules and reporting standards.
Are Certain Medical Specialties More Prone To Claim Denials?
Yes, certain medical specialties experience higher claim denial rates due to complex procedures, strict medical necessity requirements, and frequent prior authorization rules. Specialties such as cardiology, radiology, oncology, orthopedics, and durable medical equipment (DME) billing experience higher denial rates because they involve high-cost services, complex coding, and strict documentation requirements.








