Payment posting is the process of recording payments received from insurance companies and patients into a medical billing system to update claim balances. The process begins with receiving and reviewing remittance advice, followed by verifying payment details, and then posting insurance and patient payments to the correct claims and accounts.
Medical billing teams use different methods depending on the practice workflow. Common methods include manual payment posting, electronic payment posting (ERA posting), automated payment posting, and insurance payment posting for payer reimbursements.
Payment posting also requires a lot of attention because billing teams often have to deal with manual entry errors, complex insurance adjustments, and ERA–EOB discrepancies. Practices must also identify underpayments and overpayments to ensure claims are reimbursed according to payer contracts and patient balances remain accurate.

Table of Contents
ToggleWhat Is Payment Posting In Medical Billing?
Payment posting in medical billing is the process of recording payments received from insurance companies and patients into a practice management or billing system. It updates the claim status, applies payments to the correct charges, and adjusts the remaining patient balance.
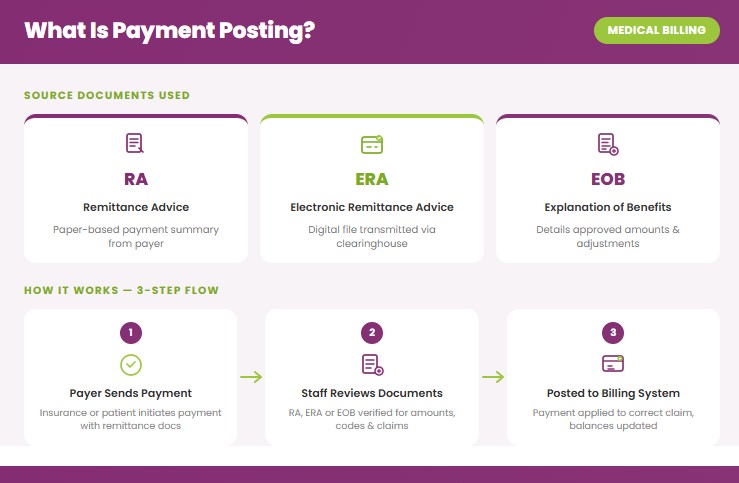
Billing staff post payments using information from remittance advice (RA), electronic remittance advice (ERA), or explanation of benefits (EOB) documents. This step confirms the amount the payer reimbursed, the adjustments applied, and the remaining balance.
What Are The Steps Of Payment Posting?
Payment posting follows a definitive workflow to record payments, apply adjustments, and reconcile claim balances in the billing system. The steps of payment posting include:
- Receive and Review Remittance Advice: Billing staff reviews the remittance advice (RA), electronic remittance advice (ERA), or explanation of benefits (EOB) to understand how claims were processed and paid.
- Verify Payment Details: Payment amounts, claim numbers, patient information, and payer details are checked for accuracy before posting.
- Post Insurance Payments: Payments received from insurance payers are applied to the corresponding claims and service charges.
- Post Patient Payments: Payments made by patients, such as copays or outstanding balances, are recorded in the patient account.
- Apply Adjustments: Contractual adjustments, write-offs, and payer-specific deductions are entered according to the remittance details.
- Identify and Address Denials: Denied or partially paid claims are flagged for correction, appeal, or resubmission.
- Reconcile Payments: Posted payments are matched with deposits and bank records to ensure totals are accurate.
- Generate Reports and Audit: Billing teams generate payment posting reports and perform audits to confirm accuracy and detect discrepancies.

After completing the main payment posting steps, each stage requires detailed attention to ensure proper revenue management. The first critical step is receiving and reviewing the remittance advice.
1. Receive and Review Remittance Advice
The first step in payment posting is collecting the Electronic Remittance Advice (ERA) or Explanation of Benefits (EOB) from insurance payers. These documents show how each claim was processed, including approved amounts, adjustments, and denials.
Billing staff interprets different payer formats, codes, and explanations to understand payment details and apply them correctly. They verify that the payment information matches the submitted claim data, ensuring patient and claim identifiers are accurate.
During this review, staff check for underpayments, overpayments, or coding errors before posting. Careful examination at this stage prevents mistakes and ensures accurate revenue tracking further along the process.
2. Verify Payment Details
Verifying payment details ensures that procedure codes, patient information, and payer-allowed amounts match the original claim. Billing staff checks that the payment aligns with the negotiated payer-provider contracts.
They review the remittance advice to identify discrepancies between expected and received payments and take corrective action if needed. This step also confirms that the payer’s adjudication process correctly applied benefits, adjustments, and patient responsibility before posting.
Additionally, staff cross-checks service dates, modifiers, and diagnosis codes to ensure all billed services are correctly reimbursed. Any inconsistencies are documented for follow-up with the payer, reducing the risk of denied or delayed claims.
3. Post Insurance Payments
Posting insurance payments involves entering received payments into the practice management or billing software. Each payment is applied to the correct patient account and claim to maintain accurate balances.
Billing staff updates the remaining patient responsibility after insurance payments and adjustments. Verifying data entry at this stage prevents errors in accounts receivable and financial reporting.
This step also includes reconciling the payment against the remittance advice totals and noting any partial payments, denials, or adjustments. Proper documentation ensures transparency and supports future audits or appeals if discrepancies arise.
4. Post Patient Payments
Posting patient payments involves accurately entering co-pays, deductibles, and coinsurance amounts into the billing system. Each payment is applied to the correct patient account, keeping the ledger up to date with all payments, adjustments, and balances.
Staff calculates the remaining patient responsibility after accounting for insurance contributions to confirm what the patient owes. Maintaining accurate records ensures billing data is ready for internal audits or patient inquiries.
Additionally, consistent posting helps track payment trends, follow up on outstanding balances, and supports efficient collection processes, reducing errors in revenue cycle management.
5. Apply Adjustments
Applying adjustments involves entering payer-specific contractual rates or discounts to modify billed amounts according to agreements. Non-reimbursable charges or services excluded by the payer are written off to reflect accurate account balances.
Staff also handle secondary or tertiary claims, submitting them after primary insurance payments and reconciling the results. Any discrepancies in patient or insurance balances are corrected to maintain accurate accounts receivable.
This process ensures that all payments and adjustments are properly reflected in the billing system, preventing overbilling and maintaining compliance with payer contracts and regulations.
6. Identify and Address Denials
Identifying and addressing denials involves reviewing payer responses and remittance advice to identify denied claims. Denials are classified by type, such as eligibility, coding, or authorization issues, to determine the appropriate corrective action.
Staff correct errors, gather supporting documentation, and submit appeals to recover denied payments. Prioritizing denials based on potential reimbursement ensures practices maximize revenue and reduce financial losses.
Tracking denial patterns also helps identify recurring issues, allowing billing teams to implement preventive measures and improve overall claim acceptance rates.
7. Reconcile Payments
Reconciliation involves matching recorded insurance and patient payments with actual bank deposit records. Billing staff verifies that total posted payments align with daily collections and system reports.
Any variances between the billing system totals and bank statements are identified and corrected. Implementing daily and monthly reconciliation processes ensures financial accuracy.
Regular reconciliation also helps detect posting errors, missing payments, and duplicate entries, supporting accurate reporting and minimizing discrepancies in accounts receivable.
8. Generate Reports and Audit
Generating reports involves creating regular summaries of collections, adjustments, denials, and accounts receivable. These reports help practices to analyze reimbursement patterns, payer performance, and cash flow trends over time.
Periodic audits are conducted to ensure billing accuracy and regulatory compliance. Staff performance, error rates, denial management efficiency, and overall revenue cycle performance are also assessed.
This process enables practices to identify opportunities for improvement, optimize revenue collection, and maintain transparency in financial operations.

What are the Types of Payment Posting?
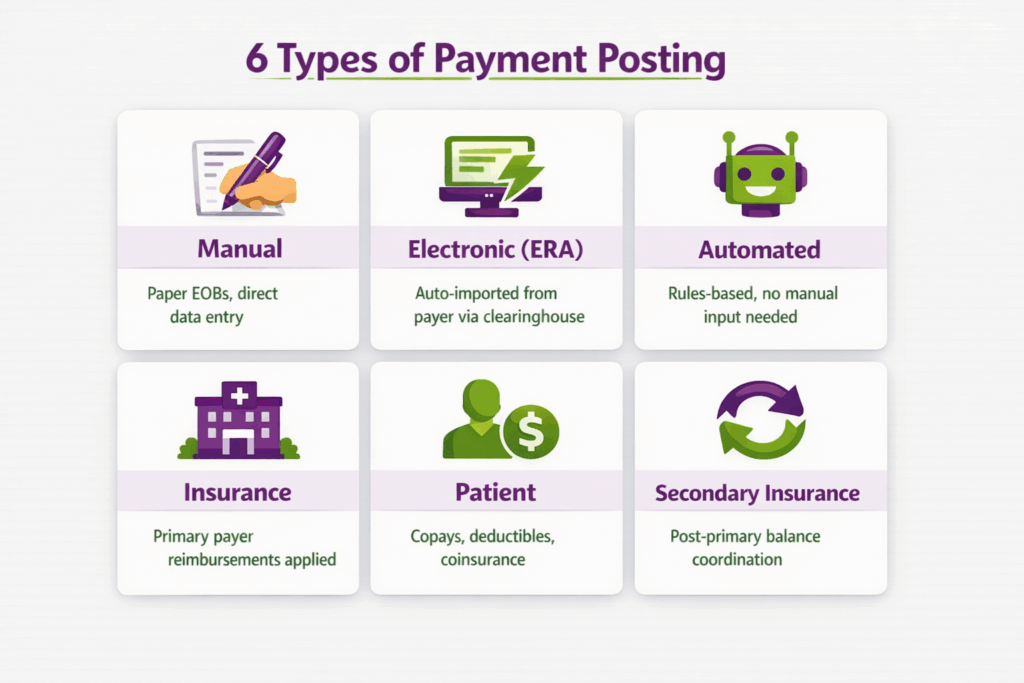
Payment posting in medical billing can be performed through several methods, depending on how payments are received and processed. The types of payment posting are listed below:
- Manual Payment Posting: Payments are entered manually into the billing system using information from remittance advice or explanation of benefits documents.
- Electronic Payment Posting (ERA Posting): Payments are posted using electronic remittance advice files received directly from insurance payers.
- Automated Payment Posting: Billing systems automatically post payments and adjustments using ERA data and predefined automation rules.
- Insurance Payment Posting: Payments received from primary insurance payers are applied to claims based on payer adjudication details.
- Patient Payment Posting: Payments made by patients, such as co-pays, deductibles, and coinsurance, are recorded and applied to their account balances.
- Secondary Insurance Posting: Remaining balances are submitted to secondary insurers, and payments are posted after the secondary payer processes the claim.
Manual Payment Posting
Manual payment posting is the process of entering payment information manually into the billing system based on payer remittance documents. It is typically performed using paper Explanation of Benefits (EOBs) or printed remittance details.
Billing staff enter payment amounts, adjustments, and denial codes directly into the practice management or billing software. Before posting, they review the EOB to interpret payer codes, allowed amounts, and adjustment explanations.
Staff also cross-check claim numbers, procedure codes, billed amounts, and patient responsibility to ensure the payment matches the processed claim. This verification step helps prevent incorrect balances or misapplied payments.
Manual posting has a higher risk of data entry errors and generally takes longer than electronic or automated methods. However, it may still be practical for smaller practices with low claim volume that process fewer remittances.
Electronic Payment Posting (ERA Posting)
Electronic payment posting is the process of recording insurance payments using Electronic Remittance Advice (ERA) files received from payers. The ERA provides structured payment and adjustment data that can be imported into the billing system.
Billing systems receive ERA files through a clearinghouse, which transmits remittance information from payers to providers. The ERA file is then imported into the practice management or billing software, allowing payments and adjustments to be applied automatically to the corresponding claims.
The remittance data includes payment amounts, adjustment codes, denial codes, and patient responsibility, which are mapped to the correct charges during posting. Staff review the imported transactions to confirm that the system correctly applied the remittance information.
Electronic posting reduces processing time compared to manual entry and improves workflow efficiency. Automation also minimizes human data entry, which lowers the risk of posting errors and improves payment accuracy.
Automated Payment Posting
Automated payment posting is the process of using billing software to automatically record payments and adjustments based on predefined system rules. The system processes remittance data and applies payments to claims without manual data entry.
Configured software rules interpret ERA payment data, adjustment codes, and denial information to post transactions according to predefined logic. Intelligent matching tools compare remittance details with claim records to ensure payments are allocated to the correct patient accounts and service charges.
Automation allows the system to process large volumes of ERA files simultaneously, significantly improving operational efficiency. This capability helps billing teams handle high claim volumes without increasing manual workload.
Transactions that cannot be matched automatically are flagged and routed to billing staff for manual review and correction. By reducing manual entry, automated posting minimizes data entry errors and improves payment posting accuracy.
Insurance Payment Posting
Insurance payment posting is the process of recording payments received from insurance payers and applying them to the corresponding medical claims. It ensures payer reimbursements are accurately reflected in the billing system.
Billing staff enter primary insurance payments into the practice management or billing software based on remittance advice or ERA data. They apply payer-specific contractual write-offs according to negotiated reimbursement agreements.
During posting, staff compare the payer’s allowed amount with the original billed charges to confirm that adjustments and reductions follow the payer contract. Any differences are reviewed to identify underpayments or incorrect adjustments.
After applying the insurance payment, billing teams monitor the remaining claim balance to determine whether it should be billed to a secondary insurer or assigned as patient responsibility.
Patient Payment Posting
Patient payment posting is the process of recording payments made directly by patients in the billing system. These payments typically include co-pays, deductibles, coinsurance, and outstanding balances.
Billing staff enter patient payments received through point-of-service collections, online payments, checks, or credit card transactions. Each payment is applied to the correct patient account and service charges to ensure accurate account balances.
The billing system is updated in real time after payments and adjustments are posted, maintaining an accurate record of patient financial responsibility. Staff also reconcile front-desk collections with back-office billing records to confirm that all payments are properly documented.
Maintaining clear, itemized patient account records supports internal audits and allows staff to respond accurately to patient billing inquiries.
Secondary Insurance Posting
Secondary insurance posting is the process of recording payments received from a secondary insurance payer after the primary insurer has processed the claim. It ensures that remaining eligible balances are billed and reconciled correctly.
Billing staff submits the remaining balance to the secondary insurance carrier after the primary payer adjudicates the claim. This process follows Coordination of Benefits (COB) rules to ensure the correct payment sequence between primary and secondary payers.
The remaining amount from the primary payer’s remittance is transferred to the secondary payer, along with the necessary claim and payment details. After the secondary insurer processes the claim, the received payment is posted to the billing system.
Additional contractual adjustments or write-offs are applied based on the secondary payer’s remittance details. Any remaining balance after secondary payment is assigned as the patient’s responsibility if applicable.

What Are The Challenges In Payment Posting?
Payment posting involves several challenges that can affect revenue cycle performance. Some of the key challenges in payment posting include:

Manual Entry Errors
Manual entry errors occur when payment details, adjustments, or claim information are entered incorrectly into the billing system. These errors can affect account balances and revenue accuracy.
Verifying procedure codes, payment amounts, and adjustment entries before finalizing postings is critical. Staff also confirm patient identifiers and claim numbers to ensure payments are applied to the correct accounts.
Incorrect postings increase rework time, delay revenue collection, and disrupt cash flow. Persistent errors can trigger compliance reviews, payer audits, and financial discrepancies, making verification essential in payment posting.
Complex Insurance Adjustments
Complex insurance adjustments are modifications to billed charges based on payer-specific contractual rules, discounts, or allowances. They ensure payments reflect the agreed-upon reimbursement terms.
Billing staff must reference each payer’s contract and fee schedule to apply adjustments accurately. They reconcile billed charges with payer-allowed amounts to prevent posting errors and ensure the correct balance is reflected in patient accounts.
Misinterpreting contract terms can result in incorrect write-offs, underpayments, and potential revenue loss, making careful review essential during payment posting.
ERA and EOB Discrepancies
ERA and EOB discrepancies occur when payment details differ between electronic remittance advice (ERA) files and paper Explanation of Benefits (EOB) documents. These differences can affect the accuracy of payment posting if not reconciled.
Staff must verify that all payment amounts, adjustments, and patient responsibility information are complete before posting. They also standardize data interpretation across various payer formats to ensure consistency in payment applications.
Discrepancies or missing information can slow the payment posting and reconciliation process. Implementing cross-checks and exception workflows helps mitigate errors and maintain timely revenue collection.
Underpayments and Overpayments
Underpayments and overpayments occur when the amount received from a payer or patient does not match the expected payment based on the billed charges or contractual agreements. These variances must be identified to maintain accurate accounts.
Staff compare received payments against payer contracts and fee schedules to find discrepancies. Underpayments are flagged, and follow-up actions are taken with the payer to recover lost revenue. Overpayments are managed by issuing refunds and documenting actions according to payer rules.
Unresolved payment variances can affect financial reporting, delay reconciliation, and disrupt overall cash flow, making timely detection and correction critical in payment posting.
High Claim Volume
High claim volume refers to a large number of claims that need to be posted and reconciled within a given period. It can strain staff capacity and slow down payment posting, especially during peak periods.
To manage backlog, billing teams prioritize claims, implement scheduling strategies, and maintain consistent posting timelines. Measures such as workload balancing, cross-training, and temporary support help reduce fatigue-related errors.
Adjusting staffing levels, leveraging automation tools, and optimizing workflows ensure that increased claim volume is handled efficiently without compromising accuracy or revenue collection.
Denial Code Misinterpretation
Denial code misinterpretation occurs when the reason for a claim denial is misunderstood or incorrectly recorded. Accurate interpretation is essential to determine why a claim was rejected and what corrective actions are needed.
Billing staff classifies denials correctly to enable timely corrections, resubmissions, or appeals. Mismanaged denials can prolong accounts receivable cycles, delay payments, and reduce cash flow.
Errors in denial handling also negatively affect overall revenue cycle performance and staff productivity, making precise coding and documentation critical in payment posting.
Payment Reconciliation Issues
Payment reconciliation issues occur when posted payments do not accurately match actual amounts received from payers or patients. Resolving these discrepancies is essential to maintaining accurate financial records.
Staff reconcile bank deposits, electronic remittance advice (ERA), and patient payments to ensure all transactions are correctly recorded. Reconciliation issues can delay reporting cycles and compromise the accuracy of financial statements.
Manual reconciliation workflows typically have higher error rates and slower processing, while automated systems improve efficiency, accuracy, and timely detection of discrepancies.
Lack of Staff Training
Lack of staff training occurs when billing personnel are not adequately educated on payment posting workflows, adjustment rules, and software use. Insufficient training increases the risk of errors and inefficiencies in the payment posting process.
Without proper knowledge, staff may make data entry mistakes, delay postings, and create additional rework. These errors can negatively impact accounts receivable aging, cash flow, and compliance with payer regulations.
Implementing standardized SOPs and structured training programs helps reduce variability, improve accuracy, and ensure consistent payment posting practices across the billing team.
Technology Integration Problems
Technology integration problems occur when clinical, billing, and financial systems are not fully connected, leading to gaps in data flow. Seamless integration is essential to ensure accurate, real-time information across all systems.
Staff must detect and correct discrepancies caused by integration gaps or software misalignment to maintain accurate payment posting. Manual intervention to resolve these issues can create workflow bottlenecks and slow overall processes.
Integration challenges also reduce automation efficiency, increase error rates, and affect the accuracy of financial reporting, making robust system connectivity critical for effective payment posting.

What Is The Role Of A Payment Posting Specialist?
A payment posting specialist ensures that all insurance and patient payments are accurately applied to claims, bridging the gap between received remittance data and the billing system. They handle EOB/ERA data entry, denial posting, contractual adjustments, write-offs, and secondary insurance processing, which are critical to maintaining accurate accounts and preventing revenue loss.
Using EHR/EMR systems, clearinghouses, and billing platforms, specialists streamline payment posting, reconcile discrepancies, and generate financial reports. Their role connects the workflow steps, posting types, and common challenges, ensuring efficient, accurate, and timely revenue cycle management.
Why Is Payment Posting Important In The Revenue Cycle?
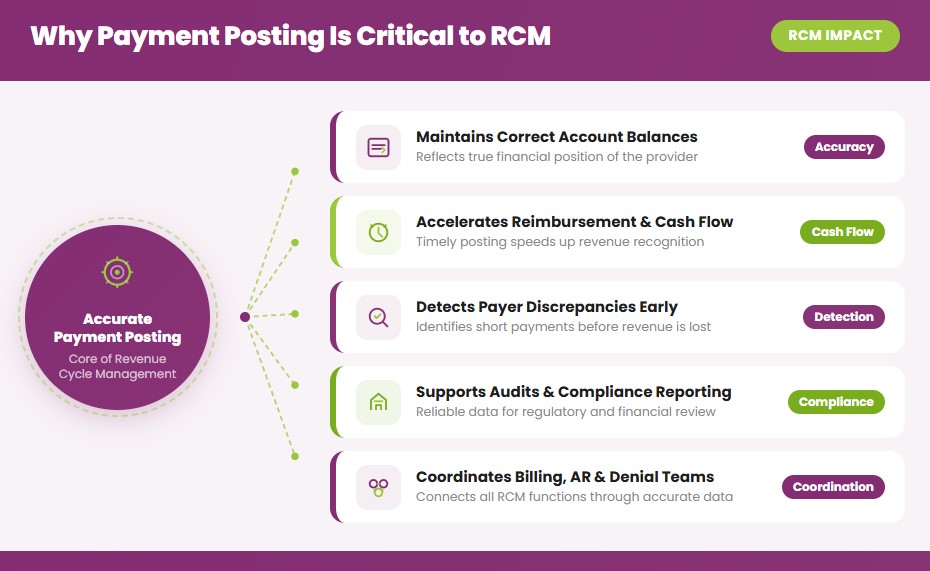
Payment posting is critical because it ensures that all insurance and patient payments are accurately recorded throughout the Revenue Cycle Management (RCM) process. Accurate posting maintains correct account balances and reflects the true financial position of a healthcare provider.
Timely and precise payment posting accelerates reimbursement, improves cash flow, and supports overall financial stability. It allows staff to track accounts receivable (AR) balances, identify outstanding claims, and follow up on unpaid or partially paid accounts.
Accurate posting also detects payer discrepancies, short payments, and contractual variances, enabling corrective action before revenue is lost. Reliable posting data supports revenue forecasting, audits, compliance reporting, and coordination among billing, AR follow-up, and denial management teams, ensuring an efficient and transparent revenue cycle.
How Does Payment Posting Impact Medical Billing Cash Flow?
Payment posting impacts medical billing cash flow by ensuring payments are accurately recorded and applied to patient and insurance accounts. Payment posting directly affects revenue collection and financial stability. Some of the key impacts include:
- Timely Recognition of Revenue: Payments are posted promptly, enabling providers to recognize revenue as soon as they are received.
- Accurate Account Balances: Proper posting ensures patient and payer balances are correct, preventing errors that can delay collections.
- Identification of Denials and Shortfalls: Early detection of denied or underpaid claims allows for faster resolution and follow-up.
- Efficient Accounts Receivable Management: Accurate posting supports tracking outstanding balances and prioritizing collections.
- Reduced Revenue Leakage: Correct application of payments minimizes lost revenue due to posting errors or missed adjustments.
- Supports Financial Planning: Reliable payment data provides the basis for cash flow forecasting, budgeting, and financial reporting.
What Is The Difference Between Payment Posting And Charge Entry?
The main difference between payment posting and charge entry lies in their stage within the revenue cycle and their purpose.
- Revenue Cycle Stage: Charge entry occurs early in the cycle when services are documented and billed, while payment posting happens later when payments from payers and patients are applied.
- Purpose & Objective: Charge entry ensures services are correctly billed for reimbursement, whereas payment posting ensures received funds are accurately recorded.
- Workflow Integration: Charge entry involves capturing service details from clinical documentation, unlike payment posting, which integrates remittance data from EOBs, ERA files, and patient payments.
- Error Impact: Errors in charge entry can lead to claim denials or underbilling, but errors in payment posting affect account balances, cash flow, and financial reporting.
- Tools & Documentation: Charge entry uses encounter forms, clinical notes, and billing software. Payment posting relies on ERA/EOBs, clearinghouses, and billing platforms.
- Financial Outcome: Accurate charge entry drives correct reimbursement, but accurate payment posting ensures timely revenue recognition and prevents revenue leakage.
How are Overpayments Handled during Payment Posting?
Overpayments are handled during payment posting by identifying, recording, and resolving payments that exceed the amount owed by the patient or allowed by the payer. Proper management ensures accurate account balances and compliance with payer rules.
- Identifying Overpayments: Detect payments that exceed the billed charges, contractual allowances, or patient responsibility.
- Recording Overpayments: Enter the overpayment amount in the billing system to clearly track excess funds.
- Resolving Overpayments: Take appropriate action, such as issuing refunds, applying the excess to future patient balances, or coordinating with secondary payers.
- Adjustments and Documentation: Apply necessary adjustments and maintain detailed records to comply with payer regulations and support audits.

What is the Significance of Payment Posting in a Healthcare Facility?
Understanding what is medical billing, including all of its processes, requires seeing how payments update the patient ledger and claim status. This process prevents overbilling and ensures that both insurance and patient contributions are accurately recorded for financial audits.









