Claim scrubbing is the pre-submission review process that audits every insurance claim for coding mistakes, missing information, and payer rule violations before it ever reaches the insurer. The process moves through five structured stages: pre-submission validation, coding accuracy review, regulatory compliance checks, payer-specific requirements verification, and a final data integrity review. Done correctly, it reduces denial rates by up to 90%, accelerates reimbursements, and strengthens overall revenue cycle efficiency.
Without it, the consequences are specific. Incorrect diagnosis codes, mismatched procedure-to-diagnosis pairs, and missing or expired prior authorizations are among the most common errors that send claims back from payers weeks after submission.
This guide covers everything, including the definition, the full process, the key benefits, the errors to watch for, and how to prevent them.

Table of Contents
ToggleWhat is Claim Scrubbing?
Claim Scrubbing in medical billing is a pre-submission review process. It audits insurance claims for errors, inconsistencies, and missing data before those claims are sent to an insurance payer. The goal is to achieve a high “clean claim” rate, meaning the payer accepts and pays the claim on the first attempt without rejections or denials.
Medical practices lose thousands of dollars every year to denied claims, not because the services were not rendered, but because the billing contained preventable errors. Reworking a single denied claim costs an average of $118, and up to 30% of claims are initially denied for completely avoidable reasons.
Think of it as proofreading for medical bills. But not the casual kind. This is a structured, rule-based inspection that checks every data point on a claim against coding standards, payer requirements, and federal regulations.
The output of this process is either a clean claim ready for transmission or a flagged claim that gets returned to the billing team for correction. Nothing gets sent to the payer if it does not pass inspection.
A claim in medical billing is a formal request for reimbursement submitted by a provider to an insurance payer. It documents which services were performed, by whom, to whom, and which codes justify the charges. Claim scrubbing is the verification layer that confirms all of that information is accurate, complete, and compliant before it leaves the practice.
Claim Scrubber vs Clearinghouse
For your clarity, here is what you need to know when comparing Clearinghouse edits vs Scrubbing.
| Aspect | Claim Scrubber | Clearinghouse |
|---|---|---|
| Primary Role | Detects and fixes errors before submission | Transmits claims between provider and payer |
| Position in Workflow | Pre-submission stage | Post-scrubbing / submission stage |
| Main Function | Validates codes, data, and compliance | Routes claims to correct the payer |
| Error Handling | Flags and helps correct errors internally | Rejects or returns claims with errors |
| Focus Area | Accuracy & compliance | Connectivity & transmission |
| Coding Checks | Yes (CPT, ICD-10, modifiers) | Limited or basic checks |
| Payer-Specific Rules | Advanced validation based on payer rules | May apply basic payer edits |
| Denial Prevention | High (prevents errors early) | Low (does not prevent, only detects) |
| Integration | Works with EHR/RCM systems | Connects providers with multiple payers |
| Output | Clean, validated claim | Accepted or rejected claim response |
| Impact on Revenue Cycle | Improves first-pass acceptance & reduces denials | Speeds up claim submission & communication |
| Example Scenario | Flags are missing a modifier before submission | Rejects claim due to missing modifier |
What is Claim Scrubber Software?
A claim scrubber, in most modern practices, is a specialized software tool integrated into the billing or Electronic Health Record (EHR) system. It acts as an automated claims scrubbing tool to implement a quality filter between the provider and the payer.
How it works:
The software sits between the EHR and the insurance company. Once a biller completes a claim, the scrubber automatically runs it through a large database of coding rules, federal regulations, including HIPAA, and payer-specific requirements.
If the claim passes all checks, it moves forward for submission. If it fails, the software flags the specific errors and sends the claim back to the biller for correction before anything leaves the system.
How it detects errors:
The scrubber uses a logic engine to cross-reference data points across multiple rule sets:
- Pattern matching: Checking if the ICD-10 diagnosis code logically supports the CPT procedure code.
- Database comparison: Verifying the provider’s NPI number, patient ID, and practice address against official registries.
- Rule validation: Applying National Correct Coding Initiative (NCCI) edits to prevent unbundling of codes that should be billed together.
- Payer logic: Knowing that one payer requires a specific modifier that another does not, and flagging the claim if it is missing.
Why it matters:
- It ensures more claims are paid on the first submission, preventing the denial-and-resubmit cycle
- It speeds up reimbursement by catching errors before the payer ever sees them
- Fixing a typo in-house is far cheaper than paying staff to research and appeal a denied claim
- It helps prevent billing fraud by confirming that all billed services are supported by documented medical necessity
Best Claims Scrubbing Software for Small Practices
| Vendor | Core Strength | Best Fit Providers | Current Value Delivered |
|---|---|---|---|
| Optum | Enterprise-scale rule library, predictive analytics, massive payer edit database | Large hospital systems, enterprise RCM teams | Enables data-driven payer negotiation and deep denial trend visibility at scale |
| Waystar | Clearinghouse-integrated scrubbing, AI-driven denial prevention, and real-time updates | Mid-to-large practices, multi-specialty groups | Learns from denial patterns quickly and improves first-pass acceptance rates (often 98%+) |
| Experian Health | Eligibility verification + demographic intelligence, front-end error prevention | Eligibility-heavy orgs, high patient-volume clinics | Prevents errors before claim creation, reducing denials tied to patient data issues |
| Athenahealth | Fully embedded scrubbing within EHR workflows, cloud-based updates | Small-to-mid practices using the Athena ecosystem | Delivers seamless workflows with consistently high clean-claim rates (~98%) |
| OmniMD | AI-driven, specialty-focused scrubbing with integrated EHR + RCM | Small and mid-sized practices, specialty clinics | Provides predictive denial prevention and affordable, scalable automation for smaller providers |

What is the Process of Claim Scrubbing?
The process of claim scrubbing is a systematic series of checks that occur after a medical encounter is coded but before the claim is submitted to an insurance payer. Each step builds on the last, and together they form a complete pre-submission validation cycle.
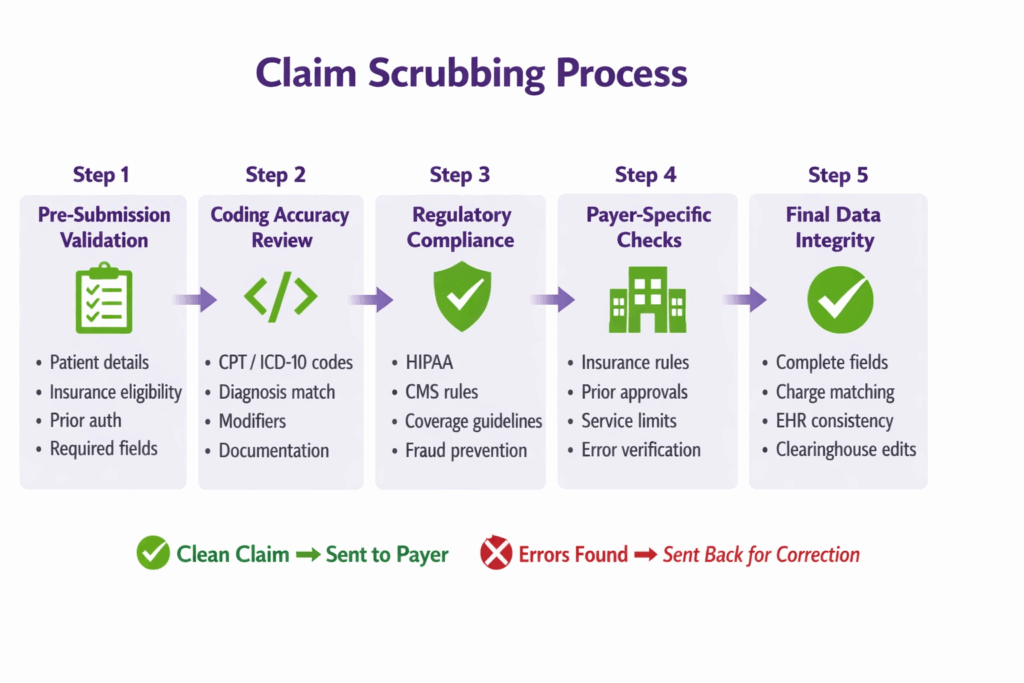
1. Pre-Submission Validation
This is the first line of defense. Before anything else gets checked, the system confirms that the basic building blocks of the claim are present and correct.
Patient demographics get verified first. Name, date of birth, gender, and insurance ID must all match what the payer has on file. A misspelled name or a single digit off in a policy number will stop a claim cold.
Then comes eligibility. Advanced scrubbers perform real-time checks to confirm the patient’s insurance is active on the date of service. This step alone prevents a significant share of rejections, because submitting a claim for a patient whose coverage lapsed is a guaranteed denial.
Other checks at this stage include:
- Confirming that prior authorizations are in place for services that require them
- Verifying that all mandatory fields on the claim form are populated
- Checking that policy and subscriber numbers are correctly formatted for proper routing
The goal here is simple. If the claim has missing or incorrect basic information, nothing else matters. This step catches those problems before they ever reach the coding validation phase.
2. Coding Accuracy Review
This is where the clinical layer gets scrutinized. Every CPT procedure code and ICD-10 diagnosis code on the claim goes through a rigorous check.
First, the scrubber confirms that codes are current and active. Medical codes change annually. ICD-10 codes update every October. CPT codes update every January. Using an expired or invalid code triggers an automatic rejection.
Next, it checks medical necessity. Each procedure code needs to be supported by a diagnosis code that justifies why the service was performed. A claim for a complex diagnostic test supported only by a vague or unrelated diagnosis code will not survive payer review.
The system also looks for:
- Upcoding or downcoding: Billing for a higher or lower complexity service than what the documentation supports
- Missing modifiers: Modifiers clarify circumstances around a service. Billing for a bilateral procedure without the correct modifier, for example, will get flagged.
- Documentation support: The scrubber checks whether the coded services align with what clinical notes actually describe
This step is where a lot of preventable denials originate. A code that is technically valid but not supported by the clinical record will pass some checks and fail others.
3. Regulatory Compliance Checks
Medical billing exists within a thick layer of regulations. HIPAA governs how patient data is handled and transmitted. CMS sets rules for Medicare and Medicaid billing. The False Claims Act makes fraudulent billing a federal offense.
The scrubber checks that the claim complies with all of these frameworks. Specifically:
- Patient information handling and transmission must meet HIPAA privacy and security standards
- Codes and billing practices must align with CMS rules
- Billed services must be consistent with both National Coverage Determinations (NCDs) and Local Coverage Determinations (LCDs), where applicable.
- All billing practices must stay compliant with anti-fraud regulations
Non-compliance is not just a billing problem. It exposes the practice to audits, fines, and potential legal liability.
4. Payer-Specific Requirements Verification
This step is where many billing teams get caught off guard. Every insurance company has its own rules. What Medicare accepts differs from what Aetna requires. What works for a commercial payer may fail for Medicaid. The scrubber applies these unique requirements to each claim individually.
Checks at this stage include:
- Confirming that services requiring prior authorization have documented approval before billing
- Verifying that all required supporting documents, such as clinical notes, lab results, or referrals, are attached
- Identifying any plan-specific exclusions or service limits that would prevent payment
- Distinguishing between clearinghouse edit failures and payer-specific edit failures, since each requires a different corrective action
A scrubber that only checks general coding rules without applying payer-specific logic is leaving significant exposure on the table.
5. Final Data Integrity Review
The last stage before submission is a comprehensive data integrity check. This is where the scrubber confirms everything is consistent across systems.
- All required fields are populated and complete.
- Total billed charges match the individual service line items and the patient ledger.
- Patient demographics, service dates, and codes are consistent between the EHR and the claim form.
- The claim passes all clearinghouse edits and meets the electronic submission standard.
Once a claim clears this final review, it goes to the clearinghouse or directly to the payer. If it fails at any point, it gets routed back to the billing team with a specific error report identifying exactly what needs to be fixed.
What are the Benefits of Claim Scrubbing?
Now you may be wondering why claims scrubbing is important. The benefits of claim scrubbing extend beyond cleaner data. They connect directly to how fast a practice gets paid, how well it manages compliance, and how efficiently the billing team operates. Each benefit below addresses a specific operational pain point.
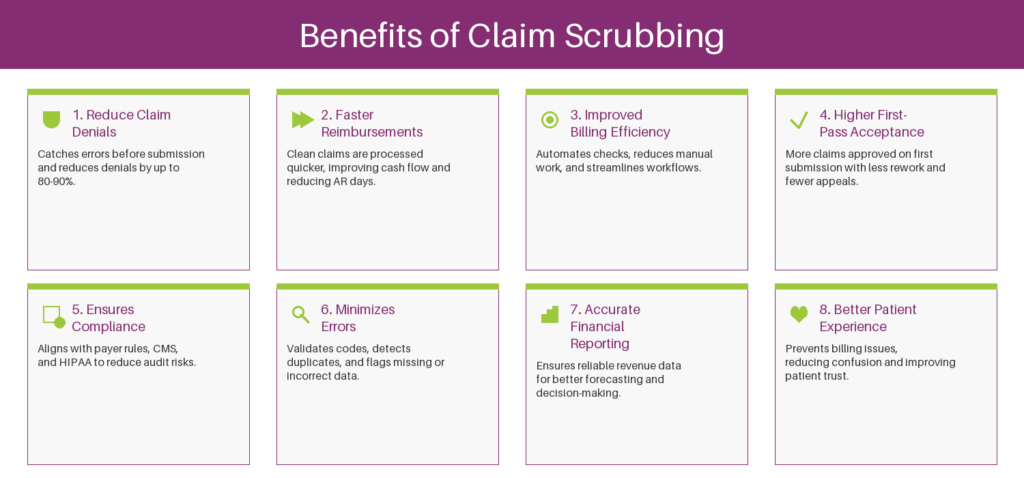
1. Reduce Claim Denials
Claim scrubbing catches preventable errors before they become denials. Incorrect codes, missing patient details, mismatched data, incomplete fields, and formatting issues. These all get flagged internally rather than returned by the payer weeks later.
The numbers are significant. Up to 30% of claims are initially denied for minor administrative errors. Effective scrubbing can reduce denial rates by 80% to 90%. That is not a small efficiency gain. That is a structural change in how a practice collects revenue.
Payer-specific rules make this even more valuable. A scrubber that knows one payer requires a specific modifier that another does not will catch that mismatch before it costs the practice a payment cycle.
2. Accelerates Reimbursements
A clean claim moves faster. Payers adjudicate accurate, complete claims quickly. There are no correction requests, no back-and-forth communications, and no appeals process.
The practical impact is a shorter accounts receivable (AR) cycle. Practices that submit scrubbed claims consistently see faster reimbursements because payers do not need to reject and reprocess. Each day reduction in AR days represents real cash flow for the practice.
3. Improves Revenue Cycle Efficiency
Scrubbing changes how billing staff spends their time. Instead of chasing denials and reworking rejected claims, they focus on higher-value work: denial management for complex cases, AR follow-up, and patient account reconciliation.
Automated scrubbing tools integrate with EHR and Revenue Cycle Management (RCM) platforms to improve data flow between clinical documentation and billing. When a provider documents a service, the scrubber immediately begins checking whether the resulting claim will hold up.
This integration reduces manual touchpoints and the errors that come with them.
4. Increases First-Pass Acceptance Rate
The first-pass acceptance rate is the percentage of claims paid on initial submission without rejection or denial. It is one of the clearest indicators of billing department health.
A high first-pass rate means:
- Less staff time spent on rework
- Faster cash collection
- Lower per-claim processing costs
- Fewer appeals and resubmissions
Claim scrubbing drives this rate up by ensuring that claims are complete, accurately coded, and payer-compliant before they ever leave the practice.
5. Ensures Compliance with Payer Guidelines
Every payer has a rulebook. The scrubber reads it for you.
Beyond preventing denials, compliance checks protect the practice from audit risk. A claim that gets paid but is later identified as non-compliant during an audit creates a recovery liability. Scrubbing ensures that claims not only clear the payer but also hold up under scrutiny.
HIPAA compliance, CMS alignment, supporting documentation requirements, and prior authorization verification. These get checked at submission, not after the fact.
6. Minimizes Billing Errors
Patient information errors, date of service mismatches, incorrect charge entry, and wrong modifiers. These are all fixable before submission if someone catches them.
The scrubber catches them. It checks CPT, ICD, and HCPCS codes for accuracy and current validity. It flags missing or incorrect modifiers. It detects duplicate charges before they create compliance flags.
7. Strengthens Financial Reporting Accuracy
Accurate billing creates accurate financial records. When every service is coded correctly, and every reimbursement is collected cleanly, the revenue data that feeds into financial reporting reflects actual performance.
This matters for forecasting, budgeting, and planning. A practice that relies on financial data distorted by unpaid or incorrectly paid claims is making decisions on faulty numbers. Clean claims create clean books.
8. Enhances Patient Satisfaction
This one gets overlooked. But billing errors affect patients directly.
When a claim is processed incorrectly, patients receive unexpected charges or confusing statements. When a claim is denied and the practice attempts to collect from the patient instead, that creates disputes and erodes trust. Accurate scrubbing prevents these downstream problems from reaching the patient at all.
What are the Possible Errors of Claim Scrubbing?
Claim scrubbing is designed to catch errors before they cause denials. But for scrubbing to work, billing teams need to understand what kinds of errors actually exist. These fall into several distinct categories.
1. Incorrect Diagnosis Codes
ICD-10 codes must be selected with precision. A code that overstates severity constitutes upcoding. A code that understates it may not support the procedure billed. A code that has been retired or replaced will trigger an automatic rejection.
Insufficiently specific codes are a common problem. ICD-10 requires specificity. Selecting a code at too high a level of generality when a more specific code exists will result in denial for many payers.
2. Invalid Procedure Codes
CPT codes that are inactive, not covered under a specific plan, or incorrectly applied will not survive scrubbing. Related procedures must be billed correctly according to bundling rules. Billing two codes separately when they should be billed as one combined code is called unbundling, and it is both a denial trigger and a compliance risk.

3. Improper Modifier Usage
Modifiers tell payers something specific about the circumstances of a service. A bilateral procedure, a service performed by an assistant, or a reduced service. When modifiers are missing, wrong, or excessive, claims get flagged.
Overusing modifiers to inflate reimbursement is a compliance risk. Using the wrong modifier for a payer that has specific requirements triggers a denial. The scrubber checks for all of these.
4. Diagnosis-to-Procedure Mismatch
Every procedure billed must be linked to a diagnosis that justifies it. If the diagnosis code does not logically support the procedure code, the claim fails medical necessity review.
Local Coverage Determinations (LCDs) and National Coverage Determinations (NCDs) define which diagnoses support which procedures for Medicare and Medicaid. Submitting a claim that violates these determinations will result in denial regardless of how the rest of the claim looks.
5. Missing or Incomplete Patient Information
Demographic errors are among the most common causes of claim rejection. Missing date of birth, misspelled patient name, incorrect subscriber ID. These stop a claim before it even reaches clinical review at the payer.
Authorization information must also be complete. A claim for a service that required prior authorization, submitted without the authorization number, will be denied. Every time.
6. Duplicate Claims
Submitting the same claim more than once, whether due to a system error or staff oversight, creates problems. Payers flag duplicate submissions and deny them. In some cases, duplicate billing can raise compliance flags suggesting intentional fraud.
Tracking submission status for every claim prevents this. A claim tracking system that confirms receipt and adjudication prevents resubmission errors.
7. Authorization or Referral Errors
Authorization numbers have validity windows. Submitting a claim after an authorization expires results in denial. The approved service type must match exactly what was billed. The date of service must fall within the authorization period.
Referral requirements work similarly. If a payer requires a referral for specialist services, the referral must be on file, current, and matched to the correct provider and service.
8. Payer-Specific Rule Violations
Each payer has formatting requirements, code-specific rules, and documentation expectations. Submitting an electronic 837 claim formatted incorrectly for a specific payer. Using a modifier that one payer accepts but another rejects. Missing an attachment that one plan requires.
These violations do not always reflect coding errors. They reflect a failure to apply payer-specific knowledge to each claim.
9. Software Configuration Errors
The scrubber itself can be misconfigured. If the software’s code library has not been updated for the current year, it will not catch retired codes. If payer rules have not been updated following a contract change, it will pass claims that should be flagged.
Software maintenance is not optional. It is a direct operational requirement.
10. Data Entry Mistakes
Manual data entry introduces errors that automated tools can catch but not prevent. A transposed digit in a policy number. A wrong date of service. A charge amount that does not match the fee schedule.
The scrubber flags these mismatches. But the root cause is upstream, in how data is entered into the system in the first place.
How to Prevent Claim Scrubbing Errors?
To prevent claim scrubbing errors, practices need structured, proactive processes, not reactive corrections.

- Ensure accurate coding: Keep code libraries updated every October for ICD-10 and every January for CPT. Train coding staff on new bundling rules and modifier requirements when changes occur.
- Validate patient information at the point of registration: Use insurance card scanners to auto-populate demographics. Build mandatory fields for date of birth, gender, and policy ID so nothing moves forward without complete data.
- Verify authorizations and referrals before the date of service: Confirm that authorization numbers are current, matched to the correct service type and CPT code, and valid through the scheduled date. Do not wait until billing to discover a lapsed authorization.
- Follow payer-specific rules with dedicated rule sets: Map each payer’s requirements into the scrubber. Different payers need different modifier rules, different attachment requirements, and different claim formatting. A generic rule set is not sufficient.
- Implement quality checks at the source: Build hard stops into the EHR that prevent chart sign-off when required fields are incomplete or when a procedure code is selected that does not match the patient’s demographic data.
- Train staff regularly: Review scrubber reports monthly. When the same biller or provider consistently triggers the same error type, that is a training gap, not a system failure. Address it directly.
- Monitor and audit claims systematically: Track denial patterns by payer, provider, service type, and error code. Use that data to make targeted improvements to both workflow and software configuration.
How Does Claims Scrubbing Reduce Denial Rates?
Claims scrubbing reduces denial rates by catching the specific errors that cause payers to reject claims before those claims ever leave the practice.
- Detecting coding errors before submission: ICD-10 and CPT mismatches, retired codes, and missing modifiers all get caught during the scrubbing cycle, not after payer review.
- Verifying patient and insurance information: Demographic errors, expired coverage, and incorrect subscriber IDs are among the top reasons for claim rejection. Real-time eligibility checks confirm coverage at the point of scrubbing.
- Ensuring compliance with payer-specific rules: Each payer operates under its own rulebook. Scrubbing applies those rules individually to each claim.
- Confirming medical necessity: The scrubber checks that the diagnosis code logically supports the procedure billed and that the combination meets payer coverage criteria.
- Reducing rework and resubmissions: Catching errors pre-submission eliminates the 14 to 30-day delay that comes with a denial-and-resubmit cycle.
- Improving first-pass claim acceptance rate: A claim that passes all scrubbing checks is far more likely to be paid on the first submission.
- Strengthening revenue cycle performance: Fewer denials mean faster AR resolution, better cash flow, and less time spent on exception handling.
Can a Medical Billing Claim be Submitted without Scrubbing?
Yes, technically, a claim can be submitted without scrubbing. But doing so significantly increases the likelihood of rejection, denial, and delayed payment. Without a pre-submission review, billing errors that could have been caught internally get returned by the payer weeks later, adding 14 to 30 days to the payment cycle per resubmission.
For practices without scrubbing software, manual audits are an alternative, but they are slower, more prone to human error, and far less scalable. Another reliable option is to get help from professional medical billing service providers, as they manage everything on their own, including claim scrubbing and denial management.
What is the Difference Between Claim Scrubbing and Claim Denial?
The main difference between claim scrubbing and claim denial is when each occurs and who is involved.
Claim scrubbing happens before the claim reaches the payer. It is performed internally, by the provider or clearinghouse, and results in a flagged claim that gets corrected before submission. Claim denial happens after the claim has been submitted. It is a formal refusal from the insurance company stating they will not pay for the service as billed.
The timing difference has major workflow implications. A scrubbing flag can be resolved the same day with no external delay. A claim denial triggers a formal appeals process, requires documentation, and may take weeks to resolve.
What is the Difference Between Manual and Automated Claim Scrubbers?
The main difference between manual and automated claim scrubbers comes down to speed, consistency, and cost.
Manual scrubbing requires a billing specialist to individually review each claim. It is slower, subject to human oversight, and not scalable for high-volume practices. It does allow for nuanced judgment on complex or unusual cases.
Automated scrubbing uses rule-based software to check thousands of claims in seconds. It can process entire billing batches simultaneously, applies rules consistently across every claim, and is estimated to be nearly 20 times faster than manual review. The tradeoff is that it requires proper configuration and regular updates to remain effective.
For practices of any meaningful scale, automated scrubbing is not a luxury. The cost of scrubbing software for small practices typically runs between $200 and $500 per month. That is frequently less than the staff time required to rework denied claims manually in the same period.
Is Claims Scrubbing Software Necessary for Small Practices?
Yes, even for small practices with low claim volumes, automated scrubbing software pays for itself within approximately three months by reducing rework costs and improving first-pass acceptance rates. The administrative cost of manually reviewing denials, preparing appeals, and resubmitting claims almost always exceeds the monthly software cost.
Small practices have fewer staff resources to absorb that rework. Every denied claim that requires a second submission is time the billing team cannot spend on other work.









