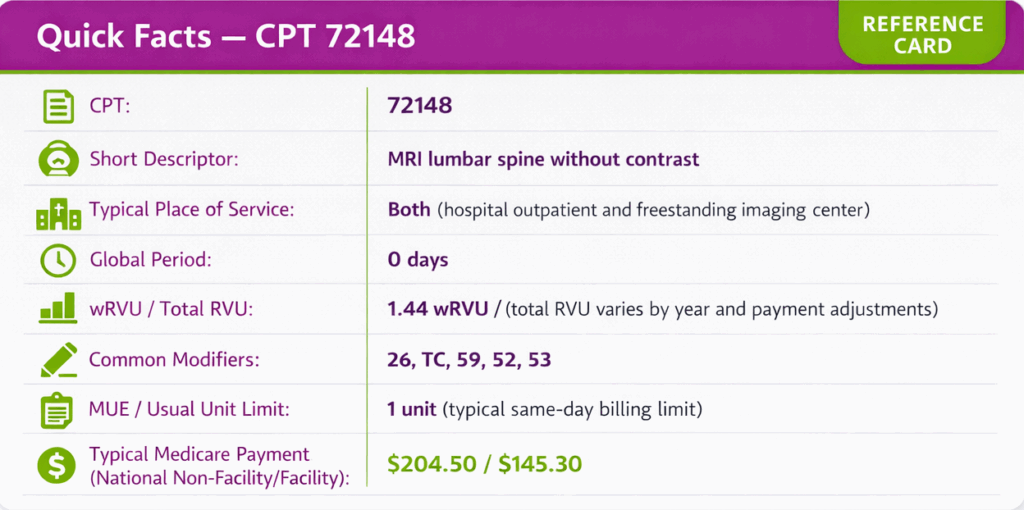
CPT 72148 represents magnetic resonance imaging of the lumbar spinal canal and contents without contrast material. This diagnostic radiology CPT code is reported by imaging centers, hospital radiology departments, and outpatient diagnostic facilities to bill for non-contrast lumbar spine MRI studies. CPT code 72148 generates approximately 2.8 million claims annually across Medicare Part B, making it one of the highest-volume imaging codes in the United States.
Table of Contents
ToggleWhat Is the Description of CPT Code 72148?
AMA defines CPT Code 72148 as “Magnetic resonance (e.g., MRI), spinal canal and contents, lumbar; without contrast material.” If contrast is used for the procedure, report CPT 72149. This diagnostic imaging procedure is used to evaluate conditions such as disc herniation, spinal stenosis, early detection of osteomyelitis, and other abnormalities of the lumbar spine.
How Much Time Is Required for CPT CODE 72148?
The typical time for CPT 72148 ranges from 30 to 60 minutes, depending on the complexity of the study and patient factors. This includes patient preparation, image acquisition, and any immediate post-processing done on the day of the procedure. Time documentation may be required when billing based on total service time or when medical necessity is questioned. Radiologists should document the total face-to-face time with the patient and, when applicable, preparation and interpretation time.
What Are the Modifiers for CPT 72148?
CPT code 72148 (or code 72148) can be reported with specific modifiers based on clinical and billing circumstances. Common modifiers include 26, TC, 59, 52, and 53.
Modifier 26 – Professional Component Only
Modifier 26 is used when the radiologist bills only for the interpretation of the MRI while the technical component (equipment, technologist, facility) is billed separately. This is commonly applied when imaging is performed at a different location than where the radiologist interprets the images.
Documentation Requirement: Radiologist’s signed report clearly documenting interpretation; separate billing arrangement noted.
Modifier TC – Technical Component Only
Modifier TC is used when billing only for the technical portion of the MRI, including use of MRI equipment, technologist services, and facility overhead, while the professional component is billed separately.
Documentation Requirement: Place of service documented (hospital outpatient or imaging center), clear delineation of technical services from professional interpretation.
Modifier 59 – Distinct Procedural Service
Modifier 59 is applied when CPT 72148 is performed on the same date as another related procedure, but the service is distinct and separate.
Documentation Requirement: Clinical notes demonstrating medical necessity and separate documentation justifying the distinct nature of the procedure.
Modifier 52 – Reduced Services
Modifier 52 is used when a partial MRI or limited protocol is performed at the discretion of the physician, such as imaging only a portion of the lumbar spine.
Documentation Requirement: Physician order specifying the limitation and explanation in the clinical record supporting reduced service.
Modifier 53 – Discontinued Procedure
Modifier 53 is applied when the MRI was started but discontinued due to patient safety concerns or clinical contraindications.
Documentation Requirement: Clear clinical documentation explaining the reason for discontinuation, including safety concerns or other clinical justification.
What is the Cost of CPT 72148?
The cost of CPT 72148 varies depending on the payer, geographic location, and place of service.
RVUs & Medicare Payment
CPT 72148 has approximately 1.44 work RVUs and a total RVU contributing to payments around higher non-facility totals, per 2026 CMS data.
For CY-2026, the Medicare non-facility national payment is approximately $204.50, and the facility national payment is approximately $145.30.
Commercial Payers
Commercial payers typically reimburse higher than Medicare rates, often ranging from $250 to $400 for CPT 72148. Actual allowed amounts depend on the payer contract, network status, and local negotiations.
For example, a commercial insurer may allow $275 to $350 for code 72148, compared with Medicare’s $145 to $205 baseline.
Place-of-Service & Geographic Adjustments
Place-of-service affects the payment amount. Non-facility settings (freestanding imaging centers) generally have higher reimbursement than hospital-based outpatient facilities.
Geographic Practice Cost Indices (GPCIs) further adjust RVUs based on regional cost differences. High-cost areas may increase payment by applying GPCI multipliers to work, practice expense, and malpractice components, while lower-cost regions may see a reduced payment.
What Are Clinical Scenarios or Use Cases Examples for CPT 72148?
CPT 72148 or 72148 code is often used in scenarios where a non-contrast lumbar spine MRI is medically necessary.
Scenario 1: Chronic Lower Back Pain Evaluation
ICD-10: M54.5 (Low back pain)
The patient presents with persistent lower back pain unresponsive to conservative therapy. MRI without contrast is ordered to evaluate intervertebral discs, nerve impingement, and degenerative changes, making 72148 code appropriate.
Scenario 2: Suspected Lumbar Disc Herniation
ICD-10: M51.26 (Other intervertebral disc displacement, lumbar region)
Patient reports sciatica symptoms. MRI without contrast confirms disc protrusion and nerve root compression. 72148 CPT code accurately represents the imaging performed.
Scenario 3: Lumbar Spine Trauma Assessment
ICD-10: S33.5XXA (Sprain of lumbar spine, initial encounter)
Following a fall, the patient has lower back pain and neurological symptoms. MRI without contrast is performed to assess spinal canal integrity and vertebral alignment. CPT 72148 supports documentation of imaging service.
What Are the CPT Code 72148 Rules To Ensure Successful Reimbursement?
Follow payer guidelines for documentation, coding, and frequency. Follow these rules to reduce denials.
Bundling & NCCI Edits:
The NCCI edit for 72149 with 72148 is 0, indicating the modifier is not allowed. Do not bill CPT 72148 and CPT 72149 together on the same claim or same day unless performed at separate encounters hours apart with distinct clinical justification. Billing both codes triggers automatic denial.
Medical Necessity Threshold:
Medicare covers this code when the procedure meets established medical necessity criteria and is supported by appropriate clinical documentation. Another important condition that some payers impose for code 72148 is that, for non-emergent conditions, patients must have received at least four weeks of conservative treatment before an MRI is considered medically necessary.
Units per Date:
Report one unit per date of service. Multiple lumbar MRIs on the same date require separate billing dates or distinct clinical justification (e.g., different spinal regions; one with, one without contrast).
Prior Authorization:
Most commercial plans require pre-authorization before scheduling non-emergent lumbar MRI studies. Turnaround times range from 24 hours for urgent requests to 5–7 business days for routine cases.
What Are The Top Reasons For CPT Code 72148 Denials And Their Remedies?
The Top Reasons For CPT Code 72148 Denials issues such as insufficient medical necessity, incorrect modifier usage, or billing inconsistencies.
Denial 1: Missing Prior Authorization (Most Common)
- Reason: Claim submitted without payer pre-approval; Medicare Advantage plans require authorization despite using Medicare fee schedules.
- Remedy: Establish an authorization verification protocol. Implement an automated tracking system flagging MRI orders pending approval. Do not schedule imaging until written authorization is received.
Denial 2: Insufficient Medical Necessity Documentation
- Reason: Vague clinical indications represent a leading cause of medical necessity denials. Ordering providers who simply write “back pain” without additional clinical context give payers grounds for denial.
- Remedy: Require ordering providers to document symptom duration, radiation patterns, neurological deficits, failed treatments, and specific clinical questions the MRI will answer. Audit charts quarterly; share denial reports with referring physicians monthly.
Denial 3: Missing 4-Week Conservative Treatment Documentation
- Reason: Payer policy requires evidence of a conservative management attempt before coverage.
- Remedy: Query the ordering provider during the authorization request for the treatment history. Obtain documentation of physical therapy visits, medication trials, or other conservative interventions. Append to claim if missing at submission.
Denial 4: Bundling with CPT 72149 or Related Codes
- Reason: Improper code pairing violates CCI edits; claims are automatically adjudicated as unbundled services.
- Remedy: Providers must rigorously check the CCI matrix to ensure no bundled services are reported separately. Verify single CPT code selection accurately reflects procedure furnished (contrast vs. non-contrast; lumbar vs. cervical/thoracic).
Denial 5: Wrong Anatomical Region
- Reason: CPT 72148 is lumbar-specific (L1–L5). Billing for cervical (CPT 72141) or thoracic (CPT 72146) studies with 72148 triggers denial.
- Remedy: Confirm the anatomical region on the ordering physician’s requisition and radiology report before coding. Train billing staff on spine segment distinctions.
Conclusion
CPT 72148 requires meticulous documentation, prior authorization verification, and strict adherence to bundling rules. Implementing proactive authorization tracking, comprehensive medical necessity checklists, and quarterly denial audits maximizes first-pass claim acceptance and revenue capture.
How Do CPT Codes Impact Reimbursement and Claims Processing?
Every billed service relies on CPT codes to communicate what procedure was performed and why. Incorrect coding can lead to underpayment or claim rejection. Learning the role of CPT codes in reimbursement workflows improves billing accuracy and efficiency.







