The U.S. medical billing outsourcing market is set to more than double by 2033, growing from $6.95 billion in 2025 to $17.69 billion at a CAGR of 12.56%, according to Grand View Research. More healthcare practices are deciding that in-house billing no longer pays off.
The reason is simple. A MGMA Stat poll found that 60% of medical group leaders reported a rise in claim denials compared to the prior year. Denials drain staff and slow cash flow. Opting for outsourcing medical billing services means entrusting that work to specialists with the tools and expertise to fix it.

This guide covers everything you need to know before you outsource medical billing. We break down what it includes, why practices are switching, what it costs, and how to pick the right partner without losing control of your revenue cycle.
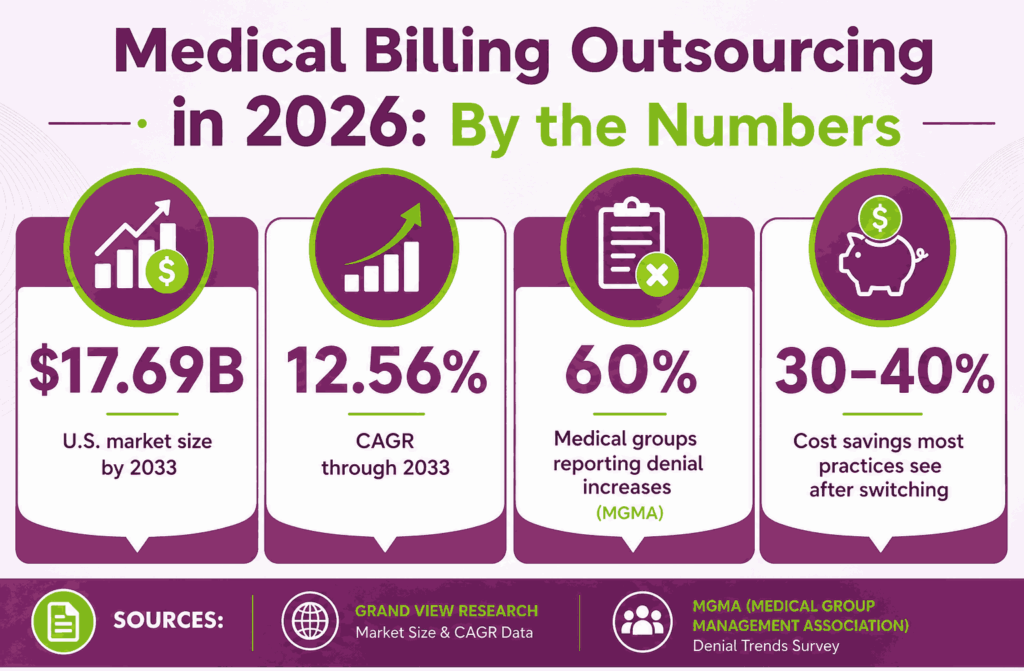
Table of Contents
ToggleWhat Is Medical Billing Outsourcing and How Does It Work?
Medical billing outsourcing means hiring a third-party expert team to handle your practice’s billing and coding instead of doing it in-house. The outsourced team manages every revenue cycle task, from coding a visit to collecting the final patient payment. Below, we break down how the workflow runs, what services are covered, and which practices benefit most.
How the Outsourced Medical Billing Workflow Operates End-to-End
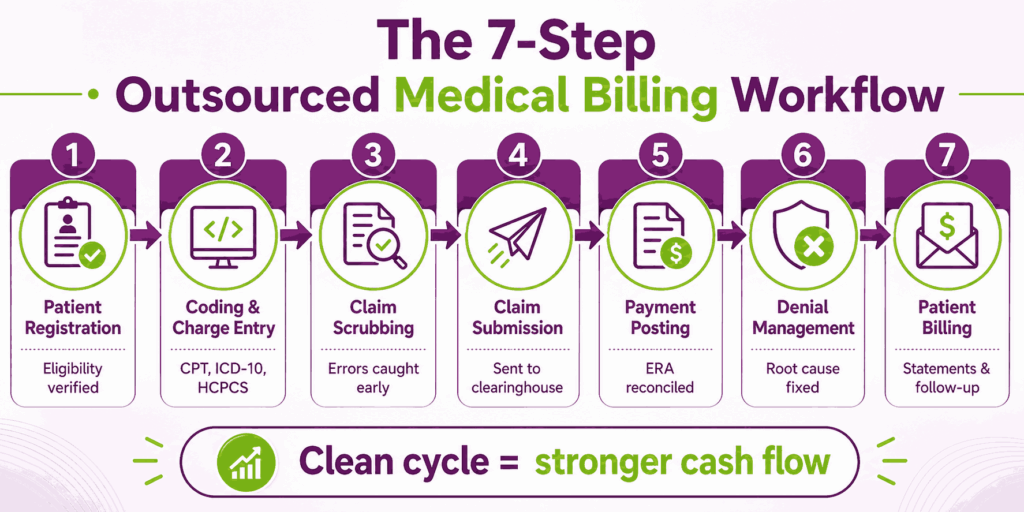
Outsourced medical billing follows a structured cycle that starts when a patient is scheduled and ends when the last dollar is collected. Each step feeds the next, and a missed step anywhere creates a denial later. The cycle flows like this:
- Patient registration and eligibility check
- Coding and charge entry (CPT, ICD-10, HCPCS)
- Claim scrubbing and submission
- Payment posting and ERA reconciliation
- Denial management and appeals
- Patient billing and collections
- Reporting and audits
When the cycle runs cleanly, cash flow improves. When it breaks, revenue leaks fast.
What Functions Are Covered Under Outsource Medical Billing Services?
Most outsource medical billing services cover the full revenue cycle, but the depth varies by company. The core functions a serious outsourced billing partner handles include charge entry and medical coding, claim scrubbing and submission, denial management and appeals, patient statements and collections, payer credentialing and enrollment, and real-time reporting on net collections, AR aging, denial rates, and payer mix.
Coding is the single biggest driver of clean claims. Scrubbing catches errors (missing modifiers, wrong NPIs, NCCI conflicts) before claims leave the system. Denial work fixes the root cause and recovers revenue. Reporting keeps you in control of what the vendor is actually doing.
Which Healthcare Practices Should Consider Outsourcing Medical Billing?
Outsourcing medical billing is not a one-size-fits-all decision. Different practice types face different pressures, and the case for outsourcing is stronger for some than others. Below are the segments where it pays off most.
Solo and Small Practices
A solo practice cannot justify a full in-house billing team. Outsourcing gives small practices certified coders and modern RCM tech without hiring a single FTE.
Multi-Specialty Group Practices
Multi-specialty groups deal with coding rules that change by specialty. An outsourced billing partner with broad coverage handles that complexity better than a small in-house team. This matters most when the group practice adds new service lines.
Ambulatory Surgery Centers (ASCs)
ASCs deal with implant billing, anesthesia splits, OR fees, and tight payer scrutiny. Generalist billers routinely miss ASC revenue.
Hospitals and Health Systems
Larger systems run on multiple EHRs and big AR balances. Outsourcing medical billing gives hospitals and health systems scalable capacity and dedicated denial teams without growing headcount.
Why Are Healthcare Practices Outsourcing Medical Billing in 2026?
Practices are outsourcing medical billing because in-house teams can no longer keep up with payer complexity, denial rates, and staffing shortages. Running billing in-house used to be the default. In 2026, it is often the more expensive choice.
What Market Trends Are Driving the Shift Toward Outsourced Medical Billing?
Three forces are pushing the shift at once: tougher payer rules, a tight labor market for billers, and AI making outsourced teams faster than most in-house operations. The U.S. medical billing outsourcing market is forecast to grow at a 12.56% CAGR through 2033, per Grand View Research, with the outsourced segment already holding 58.41% of the U.S. market in 2025. The shift is no longer a trend. It is the new default.
What Are the Top Benefits of Outsourced Medical Billing Services?
Outsourcing medical billing pays off in several ways at once. The benefits below are the ones most practices report after switching.
Significant Cost Savings vs. In-House Billing
A full in-house billing team is expensive. You pay salaries, benefits, software licenses, training, and turnover costs. Outsource medical billing services to replace that fixed cost with a percentage-of-collections fee. Most practices cut total billing costs by 30% to 40% after switching.
Higher Net Collection Rates and Faster Reimbursements
Outsourced billing teams work claims daily, not when there is time. They follow up on aging AR, fix denials fast, and submit clean claims the first time. The result is higher net collections and shorter payment cycles.
Reduced Denials and Coding Errors
Certified coders catch errors before claims leave the office. They know payer-specific rules, NCCI edits, and the latest CPT and ICD-10 updates. This is hard for a small in-house team to keep up with.
Built-In HIPAA and Regulatory Compliance
A serious outsourced billing partner runs SOC 2 Type II audits, signs BAAs, and trains staff on HIPAA every year. They also stay current with No Surprises Act rules, payer mandates, and state-level regulations. Compliance becomes a built-in feature, not a separate burden.
Scalability for Growing Healthcare Practices
When you add a provider, location, or specialty, your billing volume jumps overnight. An in-house team needs new hires, new training, and new desks. Outsourcing medical billing scales the same day, with no hiring lag.
Access to Modern RCM Technology and AI Automation
Top outsource medical billing companies invest in tools that most practices cannot afford on their own. This includes AI claim scrubbers, robotic process automation for eligibility checks, and predictive denial analytics.
What Pain Points Are Pushing Providers to Outsource Medical Billing?
Most practices do not move until the pain gets bad enough. The five issues below are the most common triggers.
Shortage of Certified Billers and Coders
There are not enough qualified billers to go around. The U.S. Bureau of Labor Statistics projects healthcare occupations to grow much faster than average through 2034, with about 1.9 million openings each year. Practices in smaller markets wait months to fill a single biller seat. Outsourcing solves the staffing gap on day one.
Rising Claim Denial Rates Across Payers
A March 2024 MGMA Stat poll found 60% of medical group leaders saw denials rise compared to the prior year. Every denial costs roughly $25 to rework, and many never get worked at all.
Increasing Coding Complexity (ICD-10, CPT, HCPCS Updates)
CPT, ICD-10, and HCPCS codes change every year. Payer rules layer more on top. A small in-house team cannot stay fluent across every specialty the way a dedicated coding team can.
No Surprises Act and Compliance Pressure
The No Surprises Act, Information Blocking Rule, and shifting state privacy laws have raised the compliance bar. Mistakes mean fines, audits, or both.
Billing Staff Burnout and Turnover
Prior authorizations are crushing in-house teams. The American Medical Association’s survey found physicians and their staff spend 13 hours per week on prior authorization, and 89% said it drives burnout. When billers burn out, they leave.
How Does In-House Billing Compare to Outsourced Medical Billing?
In-house billing gives you full control but costs more and carries hidden risks. Outsourced medical billing trades some control for lower cost, deeper expertise, and better technology. The right answer depends on your size, specialty, and how much revenue you are willing to leave on the table.
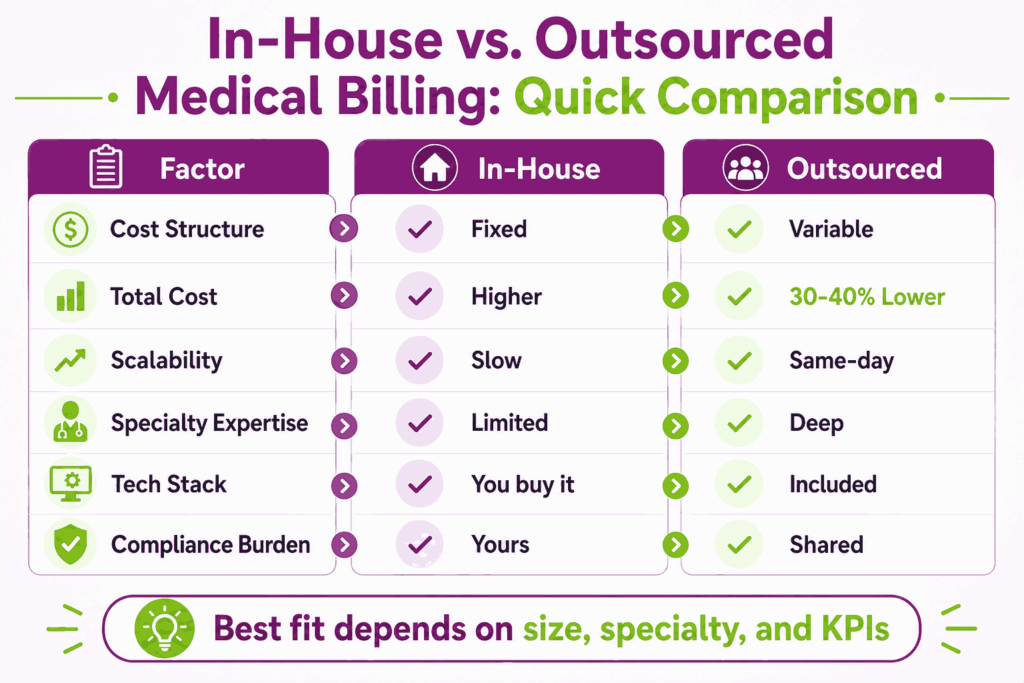
In-House vs. Outsourced Medical Billing: Side-by-Side Comparison
| Factor | In-House Billing | Outsourced Medical Billing |
|---|---|---|
| Cost structure | Fixed cost (salaries, benefits, software) | Variable cost (% of collections or per-claim fee) |
| Total cost | Higher overall, especially at scale | 30%–40% lower for most practices |
| Specialty expertise | Limited to your team’s experience | Deep coverage across multiple specialties |
| Technology stack | You buy and maintain it | Included in the service |
| Scalability | Slow, requires hiring and training | Same-day scale up or down |
| Denial management | Reactive, often understaffed | Proactive, dedicated denial teams |
| Compliance burden | Your responsibility | Shared, with vendor accountability |
| Control and visibility | Full direct control | Depends on vendor reporting |
| Staff turnover risk | High | Vendor’s problem, not yours |
| Speed to results | Months to optimize | Weeks once onboarded |
What Is the True Cost of Running Medical Billing In-House?
Most practices underestimate the true cost of in-house billing. The salary line is only the start. Once you add benefits, technology, training, and revenue leakage, the real number is often double what shows up on the payroll report. Here is what to actually count.
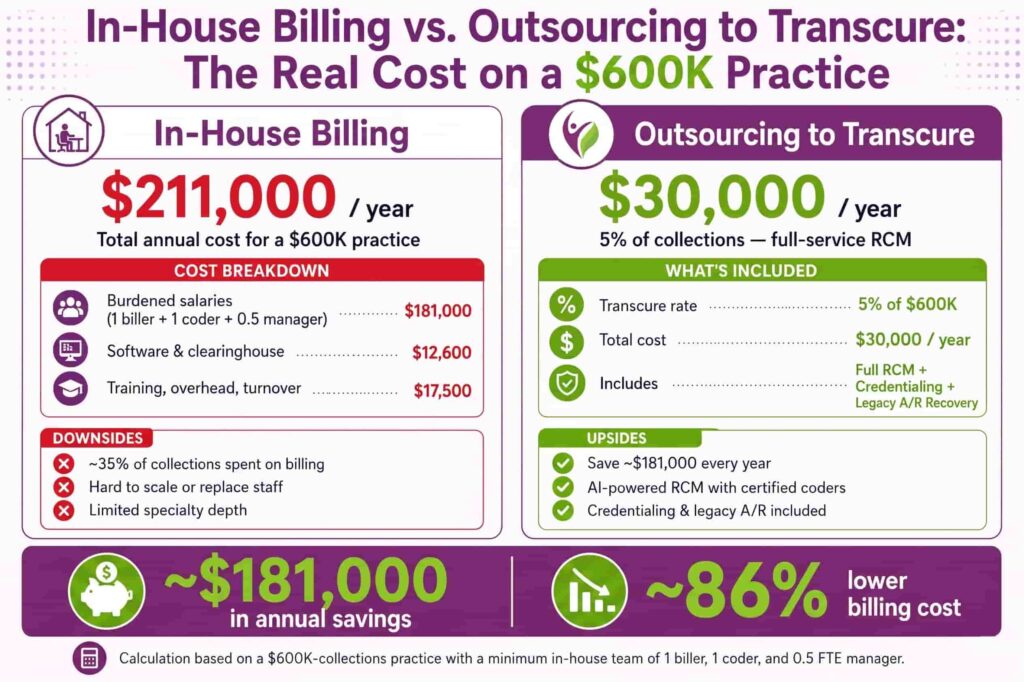
Salaries, Benefits, and Burdened Cost per FTE
A certified medical biller earns roughly $48,780 per year at the median, according to the U.S. Bureau of Labor Statistics. Add benefits, payroll taxes, and overhead, and the burdened cost per FTE runs closer to $65,000 to $75,000. Multiply that by the number of billers a practice needs, and the fixed cost gets heavy fast.
Software, Clearinghouse, and Tech Stack Fees
In-house billing needs a full tech stack. That includes a practice management system, clearinghouse fees, eligibility tools, and analytics software. Most practices spend $500 to $2,500 per provider per month on tech alone.
Training, Certification, and Turnover Costs
Coding rules change every year. CPT, ICD-10, and HCPCS updates mean ongoing training, certifications, and continuing education credits. When a biller leaves, it costs the practice 1.5x to 2x their salary to replace them, factoring in lost productivity and onboarding time.
Revenue Leakage from Denials and Aged AR
This is the cost most practices miss. Untrained or overworked billers let denials sit, miss filing deadlines, and write off recoverable revenue. A 2% drop in net collection rate on a $5M practice is $100,000 a year out the door.
When Is Outsourcing Medical Billing the Better Choice?
Outsourcing medical billing makes the most sense when in-house operations are stretched or underperforming. If two or more of these are true, outsourcing is likely the stronger move:
- Your net collection rate is below 95%
- Days in AR exceed 40
- Your denial rate is above 8%
- You are losing billers faster than you can hire them
- You are growing through new providers, locations, or specialties
- Your in-house team cannot keep up with payer rule changes
When Does Keeping Billing In-House Still Make Sense?
In-house billing still works for some practices. If your team is small, your specialty mix is narrow, and your billers are tenured and certified, you may be running just fine. The honest test is performance. If your KPIs hit benchmarks (NCR above 96%, AR days under 35, denial rate under 5%), in-house is working for you. If not, the model is the problem, not the people.
Is a Hybrid Model (In-House + Outsourced) the Right Fit for Your Practice?
A hybrid model splits the work between your in-house team and an outsourced partner. Common hybrid setups include:
- In-house front-end, outsourced back-end: Your team handles eligibility and intake, the vendor handles coding, claims, and AR follow-up.
- In-house core specialties, outsourced overflow: Your team manages your highest-volume specialties, and the vendor takes on new or low-volume ones.
- In-house day-to-day, outsourced denial and AR cleanup: The vendor handles legacy AR, denials, and appeals while your team runs current claims.

Should Your Practice Outsource Medical Billing? (A Decision Framework)
Outsourcing medical billing is not the right answer for every practice. But for most that are losing revenue to denials, struggling to hire, or growing fast, it is. The framework below helps you make the call without guessing.
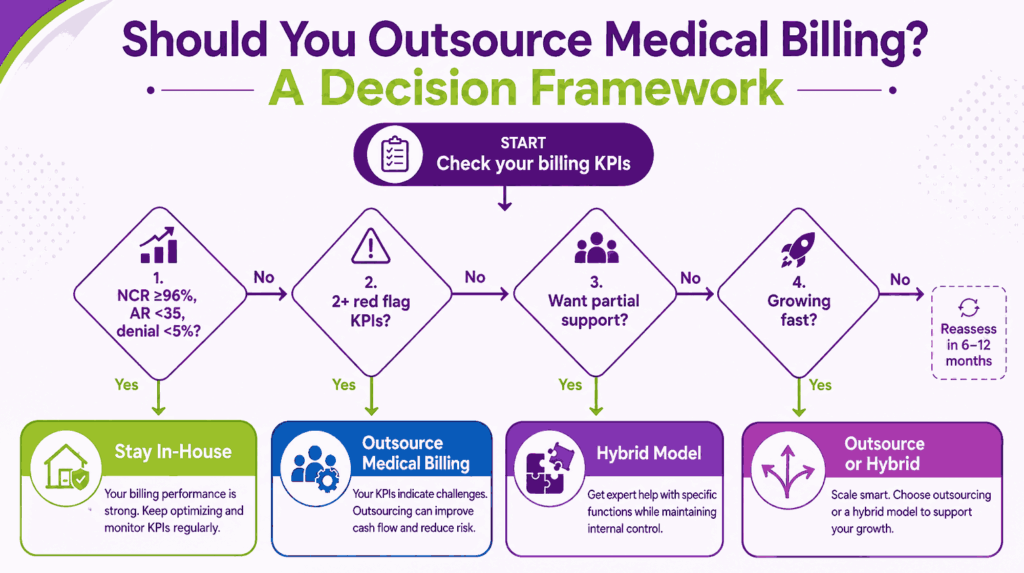
Signals It’s Time to Outsource Your Medical Billing Operations
If your numbers look like the ones below, outsourcing is no longer a “maybe.” It is a financial decision waiting to be made.
Net Collection Rate Below 90%
The MGMA benchmark for high performers is 96% or higher. Below 90%, you are leaving 6 to 10 cents of every earned dollar on the table. On a $5M practice, that is $300,000 to $500,000 a year.
Days in AR Above 40
The industry target is under 35. Once you cross 40, your billers are likely buried in old claims instead of working on new ones.
Denial Rate Above 8%
The MGMA benchmark for top performers is a denial rate under 5%. Above 8%, you are working twice as hard for the same money. And every denial costs roughly $25 to rework, with many never getting worked on at all.
Billing Staff Turnover Above 20%
Each open seat costs weeks of lost productivity, plus 1.5x to 2x salary in replacement costs. At that point, outsourcing medical billing is cheaper than hiring.
Plans to Add Locations, Providers, or Specialties
Adding a new provider or location can spike claim volume by 30% or more overnight. Outsourcing scales the same day, with no hiring lag.
Decision Framework: Outsource, In-House, or Hybrid?
| If your practice… | The right model is… |
|---|---|
| Hits NCR ≥ 96%, AR days < 35, denial rate < 5% | Stay in-house |
| Has 2+ red flag KPIs (NCR < 90%, AR > 40, denials > 8%, high turnover) | Outsource medical billing |
| Wants expert support but full visibility on a piece of the cycle | Hybrid (in-house front-end, outsourced back-end) |
| Is growing fast through acquisition or new locations | Outsource or hybrid |
| Has tenured, certified billers but weak tech | Stay in-house, upgrade tech |
| Has strong tech but constant staffing problems | Outsource medical billing |
| Runs a niche, single-specialty boutique with low volume | Stay in-house |
If two or more rows in this framework point you toward outsourcing, the cost of staying in-house is almost certainly higher than the cost of switching.
How to Choose the Right Sourcing Model for Outsourced Medical Billing
Once you decide to outsource medical billing, the next call is sourcing model. Where the work gets done matters as much as who does it. The four options trade off cost, expertise, and risk in different ways.
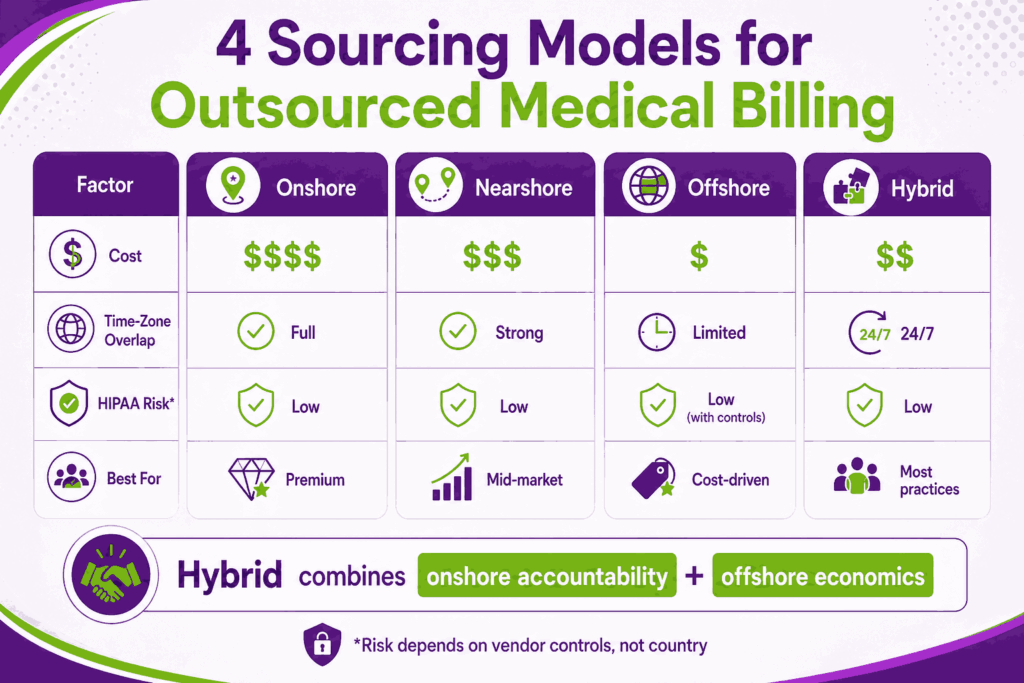
Onshore (U.S.-Based) Outsourced Medical Billing
All operations inside the U.S. Full time-zone overlap, native English, and the lowest perceived HIPAA risk. The trade-off is cost, usually 2x to 3x more expensive than offshore, with no real performance difference for most billing work.
Nearshore Medical Billing Outsourcing
Operations in Mexico, Colombia, or the Caribbean. Strong time-zone overlap, lower cost than onshore, and a smaller cultural and language gap than offshore. A middle-ground option.
Offshore Outsourced Billing Services
Offshore vendors operate in countries such as India and Pakistan, where labor costs are much lower and certified coders are abundant. Cost savings are 40% to 60% below onshore. HIPAA and time-zone concerns are valid but solved through SOC 2 Type II audits, BAAs, secure VPNs, and 24/7 coverage that actually speeds up your AR cycle.
Hybrid Onshore + Offshore Outsourcing Models
What most leading companies, including Transcure, run today. U.S.-based account managers own the relationship and stay close to your operations. Offshore teams handle high-volume coding, AR follow-up, and back-end work around the clock. Onshore accountability with offshore economics.
When evaluating sourcing models, focus on three things. HIPAA exposure is about vendor controls (SOC 2 Type II, signed BAA, encrypted access), not country. Time-zone coverage is a net positive when offshore gives you 24/7 claim work. Communication structure means U.S.-based account managers, regular standups, and shared dashboards. The model only fails when it goes dark.

What Are the Specialty-Specific Considerations for Outsourcing Medical Billing?
Every specialty has its own coding rules, payer scrutiny, and revenue traps. A generalist billing team that does fine for primary care can lose serious money on a pain practice or an ASC. The right outsourcing medical billing partner has dedicated specialty teams, not one team trying to cover everything.
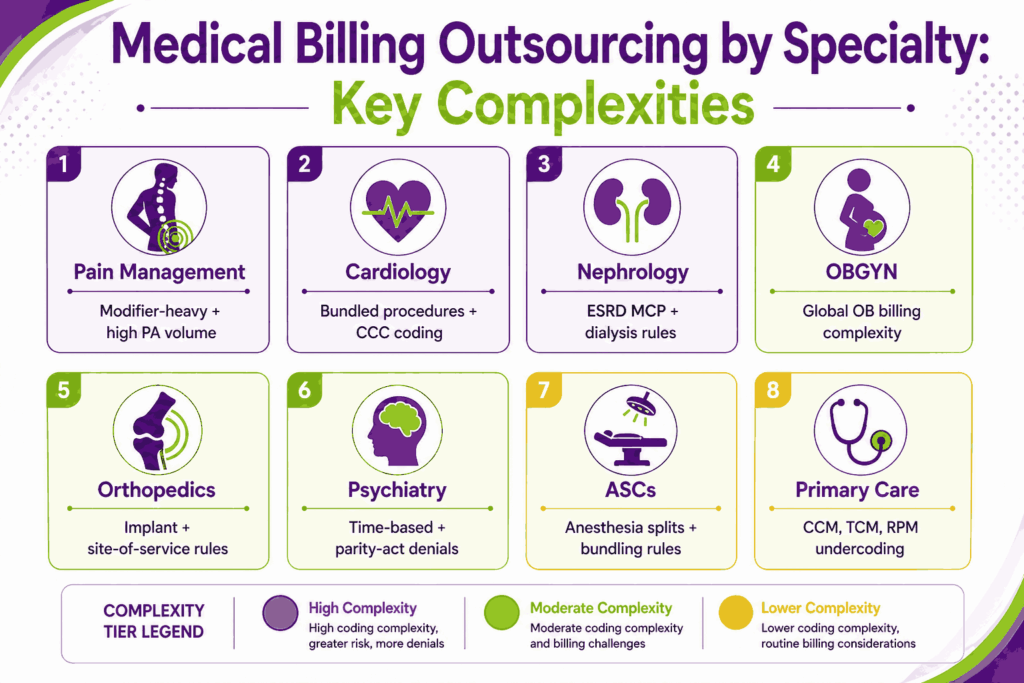
Outsourcing Medical Billing for Pain Management Practices
Pain management is one of the hardest specialties to bill. Modifier use, prior authorization volume, and payer scrutiny run heavier than average. Procedures like epidural steroid injections, facet blocks, and radiofrequency ablations require precise coding and tight medical-necessity documentation, or they get denied.
Ask any vendor how many pain practices they support and what their denial rate is for interventional pain. If you need help, our pain management billing services for specialty-specific support are something you should look into.
Outsourcing Medical Billing for Cardiology Practices
Cardiology billing involves bundled procedures, device and lead codes, and constant changes to CMS rules. A single cath lab procedure can have 5 to 10 codes that need to be sequenced correctly, with the right modifiers, or you lose revenue to bundling edits.
The vendor question that matters: do your coders hold CCC (Certified Cardiology Coder) credentials, and how do you handle global periods on cath and EP procedures? Strong cardiology billing services are built around coders who live in this code set every day.
Outsourcing Medical Billing for Nephrology Practices
Nephrology has billing rules that no other specialty shares. The Monthly Capitation Payment (MCP) model for ESRD patients, dialysis billing under Method I or Method II, and home dialysis training codes all need specialized handling. Nephrology billing services with MCP fluency will save you real money.
Outsourcing Medical Billing for OBGYN Practices
OBGYN billing splits into two worlds: routine gynecology and global obstetric care. Global OB billing means one code covers the entire pregnancy, with rules about when to bill globally and when to unbundle. Get it wrong, and you either underbill care or trigger a payer audit.
Ask the vendor how they handle antepartum care for patients who switch providers mid-pregnancy. Professional OBGYN billing services providers should be comfortable with handling all these issues.
Outsourcing Medical Billing for Orthopedic Practices
Orthopedic billing is implant-heavy and site-of-service sensitive. Whether a procedure is done in-office, in an ASC, or in a hospital changes the reimbursement, the modifiers, and the documentation requirements. Implant billing alone, with HCPCS codes and invoice-based reimbursement, trips up most generalist teams.
The right orthopedic billing partner has coders who handle implant logs and site-of-service rules every day.
Outsourcing Medical Billing for Ambulatory Surgery Centers
ASCs face a different set of challenges, including implant billing, anesthesia splits, OR fees, multiple-procedure discounts, and payer-specific bundling rules, all of which stack on top of each other. ASCs also face higher payer audit risk because of the procedure cost. That’s why outsourced ASC billing services are a specialty unto themselves, and the wrong vendor will leak revenue at every step.

How Much Does Outsourced Medical Billing Cost?
Most practices pay between 4% and 10% of monthly collections for outsourced medical billing services. The exact rate depends on specialty, claim volume, scope of work, and pricing model. Cheaper is not always better. A low rate from a vendor that misses denials will cost you more than a higher rate from one that collects every dollar.
What Are the Common Pricing Models for Medical Billing Outsourcing?
There is no single way that outsource medical billing companies charge. Most use one of the four models below, sometimes combined.
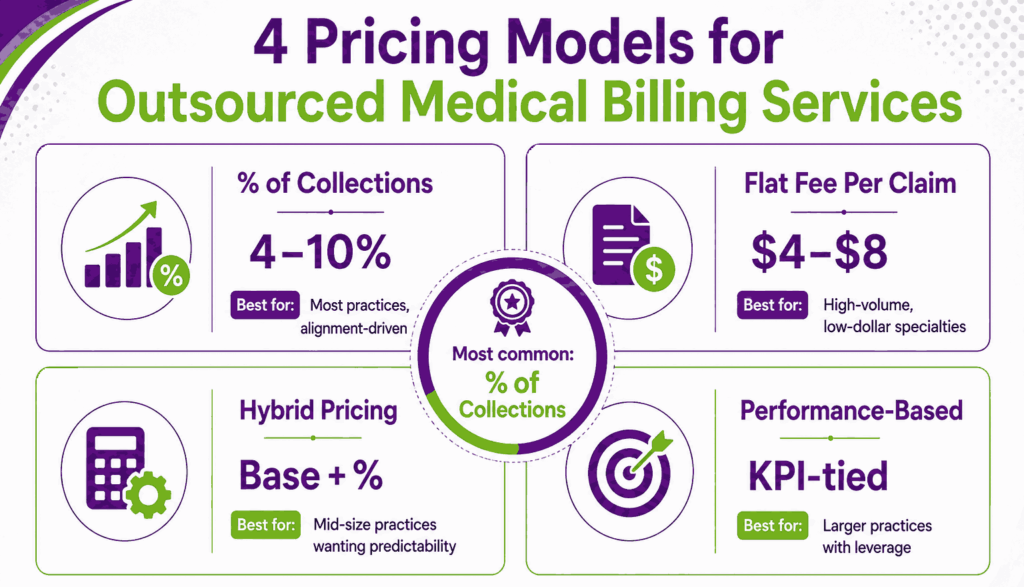
Percentage of Collections (4%–10% Industry Range)
The most common model. The vendor takes a fixed percentage of what they collect, usually 4% to 10%. Pain, ortho, and ASC practices sit at the higher end. High-volume primary care sits at the lower end. Transcure, for example, charges only 5% of the collection for the end-to-end RCM process, with no preconditions.
The advantage is alignment, as the firm only earns when you get paid. The downside is that high-revenue practices can end up paying more than on a flat fee.
Flat Fee per Claim Pricing
Some companies charge a flat fee per submitted claim, usually between $4 and $8. This works well for high-volume, low-dollar specialties where the collection rate would be expensive. The risk is misalignment. The vendor gets paid the same whether the claim collects or not.
Hybrid Pricing Models
A small base fee plus a lower percentage (e.g., $1,000/month + 3% of collections). Lowers your variable cost while keeping part of the vendor’s pay tied to performance. Good fit for mid-size practices.
Performance-Based and Value-Based Pricing
Rare but powerful when structured well. The vendor earns more when NCR, AR days, or denial rate hit agreed targets, and less when they miss. Usually only available to larger practices with the leverage to negotiate it.
Setup, Onboarding, and Termination Fees
Most agencies charge a one-time setup fee of $1,000 to $10,000 for onboarding, EHR integration, and data migration. Watch for termination fees. Some vendors lock you into 2- or 3-year contracts with steep early-exit penalties. Some, like Transcure, offer free onboarding for all practices.
How to Calculate the Total Cost of Outsourcing vs. In-House Medical Billing
Comparing in-house and outsourced costs on salary alone is the wrong math. The real comparison includes everything below.
In-house total cost includes:
- Burdened biller salaries (~$65K–$75K per FTE)
- Software, clearinghouse, and analytics tools ($500–$2,500 per provider, per month)
- Training, certification, and continuing education
- Turnover and replacement costs (1.5x–2x salary per departure)
- Revenue leakage from denials, missed filings, and aged AR
Outsourced total cost includes:
- Percentage of collections (4%–10%) or per-claim fee
- One-time setup and onboarding fee, if applicable
- Any add-on services (credentialing, patient collections, analytics)
For most practices in the $2M–$15M revenue range, outsourcing comes in 30%–40% lower once all in-house costs are counted.
How to Negotiate the Best Pricing for Outsourced Medical Billing Services
Pricing is more negotiable than most practices realize. You should always tie pricing to performance. For example, request credit back if NCR drops below 95%, AR days exceed 40, or the denial rate climbs above 8%. Similarly, push for a 12-month initial contract instead of 2–3 years, with renewal options.
You can also bundle credentialing, patient collections, or analytics to the contract, and demand real-time dashboards and monthly KPI reports should never be an add-on. The right vendor will welcome these conversations. The wrong one will resist them.
How Is AI Transforming Outsourced Medical Billing Services?
AI is changing what outsourced medical billing can deliver, but the hype is ahead of reality. The companies winning right now use AI where it actually works (eligibility, scrubbing, denial triage, AR follow-up) and keep humans in the loop where it does not (complex appeals, payer escalations, ambiguous coding).
What Medical Billing Tasks Can AI Automate Today?
AI is genuinely good at high-volume, rules-based work. The tasks below are where outsource medical billing companies are seeing real productivity gains.

Eligibility and Benefits Verification
AI bots like Transcure’s ELIXA check insurance eligibility, copays, deductibles, and prior authorization requirements in seconds across multiple payers. What used to take a front-desk team an hour per patient now happens before the patient walks in.
Prior Authorization Workflows
PA is the single biggest time drain in medical billing. AI agents, such as PRIA from Transcure, now draft PA requests, pull supporting documentation from the EHR, and automatically submit them through payer portals with over 97% accuracy.
Claim Scrubbing and Pre-Submission Edits
AI scrubbers catch missing modifiers, mismatched diagnoses, NCCI edit conflicts, and payer-specific errors before claims leave the system. Transcure maintains clean-claim rates above 98% with CLAIR, its AI scrubbing agent.
Denial Categorization and Routing
When denials come back, AI categorizes them by reason code and routes them to the right team or appeal queue. Transcure’s ARIA has an auto-resolution rate of 85% for denied claims. The denials that need human judgment get there faster.
Payment Posting and ERA Reconciliation
AI auto-posts payments from electronic remittance advice (ERA) files, matches them to the right claims, and flags variances. For example, using REMITA from Transcure offers 99.5% accuracy.
AR Follow-Up and Patient Statement Bots
AI bots work on aging AR queues, send patient statements, and trigger automated follow-up calls. They never get tired, never skip a queue, and run 24/7. This is where offshore time-zone coverage compounds with AI for real cycle-time gains.
What Tasks in Outsourcing Medical Billing Still Require Human Experts?
AI cannot do everything yet, and pretending it can is dangerous. The tasks below still need experienced humans, and any vendor claiming otherwise is overselling.
- Complex Appeals: Second- and third-level appeals need clinical reasoning, payer relationship knowledge, and persuasive writing. AI can draft, but a human has to lead.
- Payer Escalations: When payers refuse to pay despite clean claims, escalation calls, and contract enforcement, a human with leverage is needed.
- Ambiguous coding cases: When documentation is unclear, or a procedure does not fit a clean code, a certified coder has to make a judgment call.
- Compliance audits and edge cases: Anything that touches OIG audit risk or complex compliance questions needs human review.
What Are the Compliance and Audit Risks of AI in Outsourced Medical Billing?
AI introduces compliance exposure that most practices have not thought through. Three risks matter most.
- HIPAA and PHI Handling: AI tools that process patient data must be covered by your BAA, and the vendor must show how training data is segregated. Off-the-shelf LLMs are often not safe to use on PHI without specific configuration.
- OIG and Payer Audit Risk: If AI assigns a code that triggers an audit, the practice (not the vendor) is on the hook. You need clear documentation of which decisions were AI-driven, with vendor accountability built into the contract.
- Payer-Side AI Denials: Payers are using AI to deny claims at speeds humans cannot match. A 2025 ProPublica investigation reported on Cigna’s PXDX system, which allegedly let medical reviewers reject claims in batches without opening individual files. The right outsourced billing partner appeals AI-generated denials aggressively and uses their own AI to fight back.

How Do You Choose the Right Medical Billing Outsourcing Partner?
The wrong medical billing outsourcing partner can quietly cost you hundreds of thousands of dollars a year in missed collections and compliance exposure. The right one becomes an extension of your team. The difference comes down to how you evaluate, what you put in the contract, and what you negotiate before signing.
What Criteria Should You Use to Evaluate an Outsourced Medical Billing Company?
Not all outsource medical billing companies are built the same. The criteria below separate serious partners from order-takers:
- Specialty and Practice-Size Fit: Ask how many clients they have in your specialty, at your size. A vendor that mainly bills primary care will not handle ASC or pain revenue well.
- EHR/EMR Integration: Your billing partner needs to work inside your EHR, not bolt on a second system. Confirm direct experience with Epic, athena, eClinicalWorks, NextGen, Kareo, or whatever you run.
- Technology Stack and Automation: Ask what tools they use for claim scrubbing, denial analytics, and AR automation. The strongest partners run AI scrubbers, predictive denial models, and RPA bots inside a clear human-in-the-loop framework.
- Reporting Transparency: Insist on a live dashboard showing NCR, days in AR, denial rate, and payer mix. Monthly PDFs mean the vendor is filtering what you see.
- Pricing and Contract Flexibility: Short initial terms (12 months), capped rate increases, and credit-back clauses tied to KPIs all signal a vendor confident in their work.
- References, Case studies, and Client Tenure: Ask for three references in your specialty and call all three. High client tenure is the single best signal of vendor quality.
What KPIs and SLAs Should Be Written Into Your Outsourcing Medical Billing Contract?
A contract without measurable KPIs gives the vendor no accountability. Write these into the contract with target thresholds and credit-back remedies if they slip:
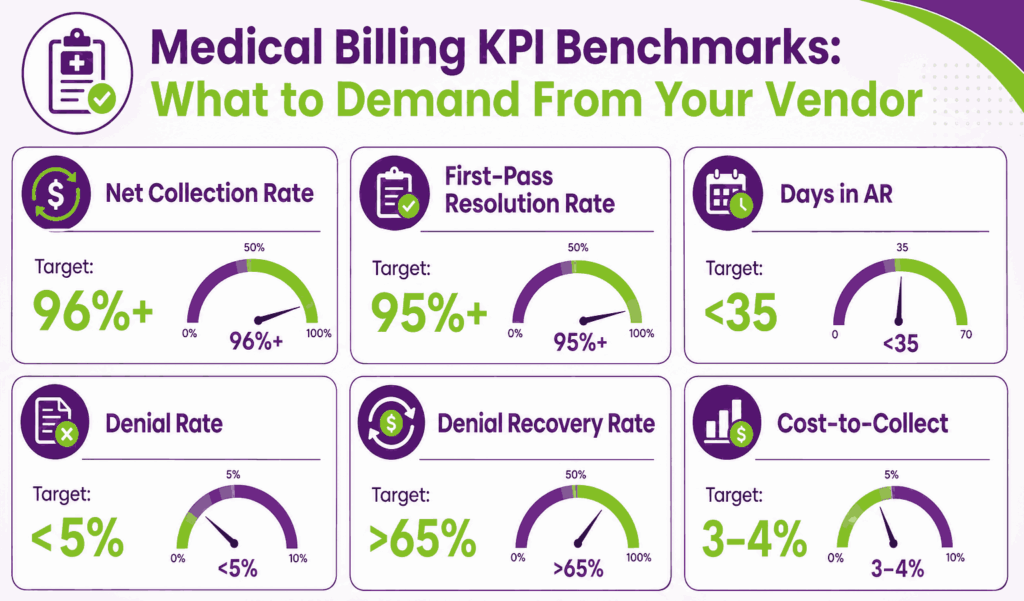
- Net Collection Rate (NCR): The MGMA benchmark for high performers is 96%+. Build credit-back if it drops below 95% for two consecutive months.
- First-Pass Resolution Rate (FPRR): Target 95%+. Below that, the vendor is leaving rework money on the table.
- Days in AR: Under 35 for a healthy practice. AR over 90 days should stay below 15% of total AR.
- Denial Rate and Recovery Rate: Denial rate target under 5%; denial recovery rate (the percentage of worked denials that get paid) above 65%.
- Cost-to-Collect: Best-in-class is 3% to 4% all-in. Ask the vendor what your cost-to-collect will look like 12 months in.
- Reporting Cadence and Escalation Paths: Weekly KPI updates and a named account manager are table stakes.
What Critical Questions Should You Ask Before Outsourcing Medical Billing?
The questions below are the ones that expose weak vendors fastest:
- How many clients do you have in our specialty and at our size?
- What is your average client tenure, and what is your annual churn rate?
- What is the average NCR, AR days, and denial rate across your client book?
- Will we have a dedicated account manager, and where are they based?
- Where do your coders, billers, and AR teams operate, and what are their certifications?
- How do you handle prior authorizations? Is it automated, manual, or hybrid?
- What is your process for working denials, and what is your denial recovery rate?
- How do you use AI, and where do humans stay in the loop?
- What is your SOC 2 status, BAA process, and HIPAA training cadence?
- What happens if performance drops below benchmarks?
- What does the offboarding process look like, and who owns the data?

What Compliance and Security Standards Must an Outsourced Medical Billing Vendor Meet?
Compliance is not negotiable. The standards below are the floor, not the ceiling.
- Signed BAA: Required before any PHI moves. The BAA should cover breach notification (24–48 hours), subprocessor disclosure, and HIPAA training. If a vendor pushes back on standard BAA language, walk away.
- SOC 2 Type II or HITRUST: SOC 2 Type II is the baseline; it proves controls work over 6 to 12 months, not just on paper. HITRUST is more rigorous and increasingly the standard for enterprise health systems.
- PHI Residency and Offshore Coverage: If any work happens offshore, the BAA must cover offshore subprocessors. Most reputable offshore vendors run secure VPN access into U.S.-based systems with no PHI stored offshore.
- Cyber Insurance and Breach SLAs: Proof of cyber liability insurance and a breach notification SLA in writing. Healthcare breach risk is real and rising.
- Subprocessor Disclosure: The vendor must disclose every subprocessor (clearinghouses, AI tools, offshore teams) that touches your data, with your right to approve new ones.
Red Flags to Watch For in Medical Billing Outsourcing Vendors
The warning signs below have shown up across years of practice, switching vendors. If you see two or more, look elsewhere:
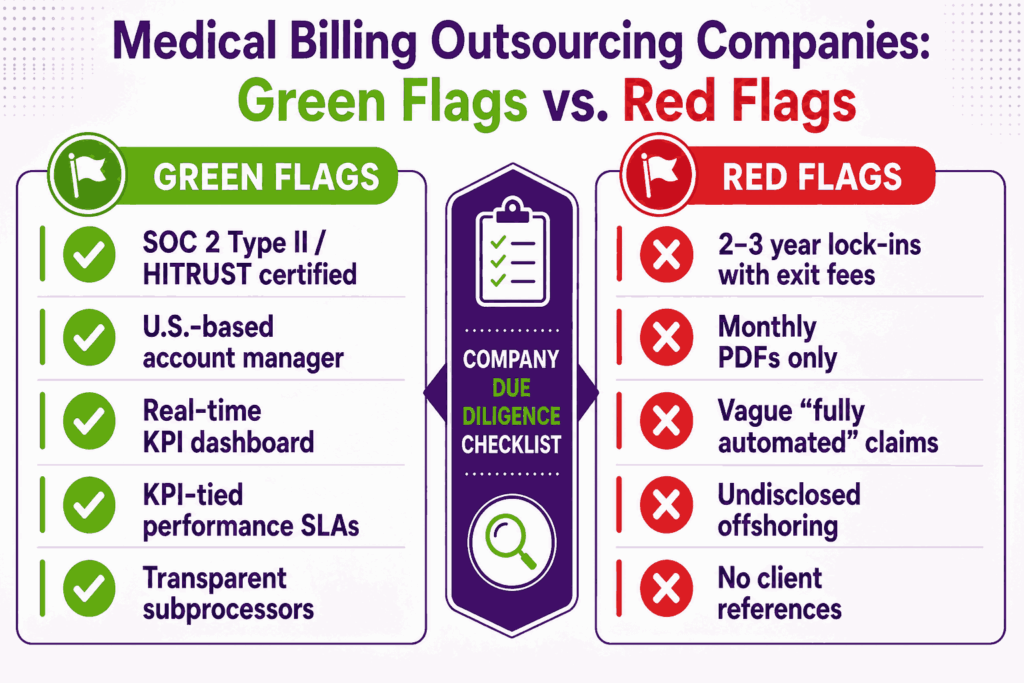
- Vague answers to specialty experience questions
- No SOC 2 Type II or HITRUST certification
- Resistance to KPI-tied performance clauses
- Long initial contract terms (2–3 years) with steep exit penalties
- No real-time reporting, only monthly summaries
- “Fully automated” claims with no human-in-the-loop detail
- Pricing that seems too good to be true (almost always is)
- Subprocessors and offshore operations are not disclosed up front
- High client churn or unwillingness to share references
If you have already shortlisted agencies and want a side-by-side comparison of the top names in the market, see our breakdown of the best medical billing outsourcing companies.
How Does the Transition to an Outsourced Medical Billing Partner Work?
A clean transition to an outsourced medical billing partner takes 60 to 90 days, with no revenue dip if it is done right. The mistakes happen when practices rush the cutover, ignore legacy AR, or fail to communicate the change. Done well, the transition is invisible to patients and barely noticed by your team.
What Is the Standard Onboarding Process for Outsourced Medical Billing?
A real onboarding has five phases, and they overlap. The company should walk you through each one before you sign, not after.
- Discovery and Audit: Review of current performance, payer mix, fee schedules, and pain points.
- System Access and Integration: Credentials set up for your EHR, clearinghouse, and payer portals with security controls verified.
- Documentation and SOPs: Vendor builds standard operating procedures specific to your practice and gets your sign-off.
- Training and Parallel Run: Outsourced team shadows your in-house team, then runs in parallel before taking over.
- Cutover and Optimization: Full handoff with weekly performance reviews for the first 90 days.
If a vendor proposes skipping any phase or compressing the timeline below 60 days, that is a warning sign.
The 30-60-90 Day Playbook for Transitioning to an Outsourced Medical Billing Company
The 90-day playbook below is what a healthy transition looks like, broken down by phase.
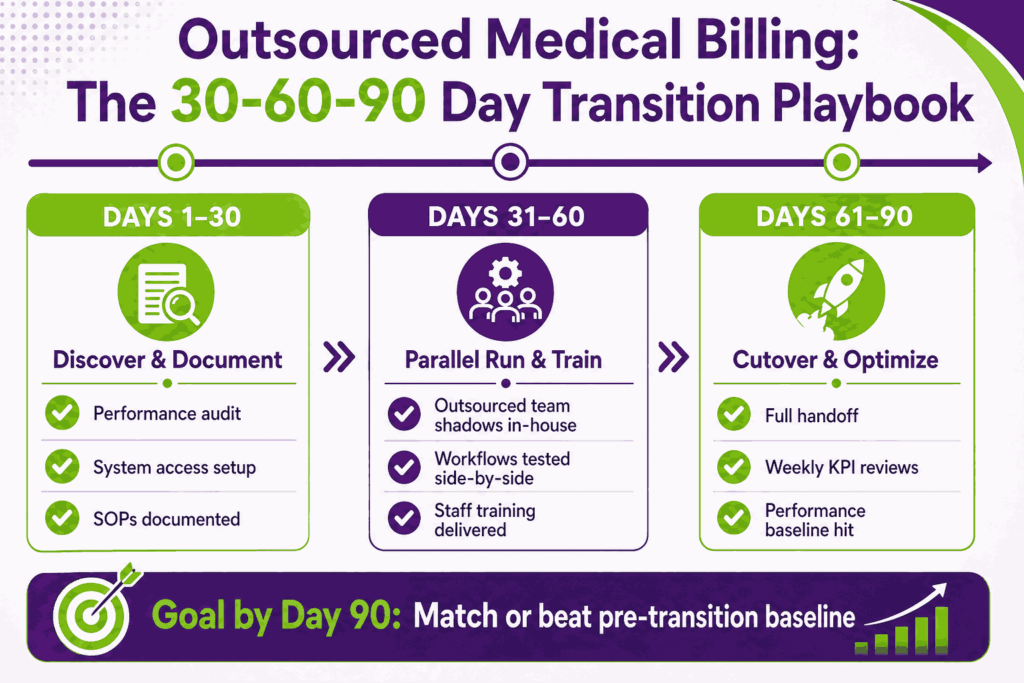
Days 1–30: Discovery, Documentation, and System Access
The first 30 days are about understanding the practice, not changing it. The firm audits current performance, builds a baseline of NCR, AR days, and denial rate, and documents every workflow. By day 30, you should have written SOPs, a documented baseline, and full system access in place.
Days 31–60: Parallel Run, SOPs, and Staff Training
The outsourced team runs alongside your in-house team. They shadow workflows, code claims in parallel, and review denials side by side. Any discrepancies get caught before they hit cash flow. Staff training happens here, too. By day 60, the outsourced team should be matching or beating in-house results in a controlled environment.
Days 61–90: Full Cutover, Performance Baselines, and Optimization
Day 61 is full cutover. The outsourced team takes over claim submission, denial work, and AR follow-up. Your in-house team either redeploys or handles legacy AR runoff. KPIs are measured weekly. By day 90, you should be hitting or exceeding the phase-one baseline.
How to Manage Legacy AR During the Outsourced Medical Billing Transition
Legacy AR is the biggest revenue risk in any billing transition. Old claims do not stop existing because you switched vendors. They keep aging, and if no one works them, they get written off. Three options:
- Outsourced Partner Takes It: The new vendor works legacy AR alongside new claims, usually at a higher percentage. Transcure offers to recover them at minimal cost or as a complementary service.
- In-house Team Finishes It: Your existing billers work down legacy AR while the new partner handles all new claims.
- Specialized AR Cleanup Vendor: A third party works only on the legacy AR. Rare but useful for very large balances.
How to Measure Success in the First 90 Days After Outsourcing Medical Billing
The first 90 days are about hitting baseline, not breaking records. Track these metrics weekly:
- Net collection rate: Should match or beat your pre-transition baseline by day 90.
- Days in AR: Expect a slight uptick in days 30–60 during parallel run, then improvement by day 90.
- Denial rate: Should drop measurably as front-end workflows tighten.
- First-pass resolution rate: Should climb as scrubbing kicks in.
- Cash collected: The most important metric. Should match prior 90-day cash within 5% by day 90, and beat it by day 180.
If any of these metrics are tracking the wrong way at day 60, that is the time to escalate, not day 120 when the damage is done. A serious outsourced medical billing partner will surface problems before you have to ask.
Frequently Asked Questions About Medical Billing Outsourcing
How Do You Track the Performance of an Outsourced Medical Billing Company?
You track the performance of an outsourced medical billing company through real-time KPI dashboards reviewed weekly, monthly trend reports against MGMA benchmarks, and a named account manager. Track NCR, days in AR, denial rate, and denial recovery rate at a minimum.
Can Outsourced Medical Billing Handle Multiple Specialties?
Yes, if the vendor has dedicated specialty teams. Ask whether you get separate teams per specialty or one general team trying to cover everything.
What Happens If You Want to Switch Medical Billing Outsourcing Companies?
You should be able to switch on 30 to 90 days’ notice with full data export in usable formats. The catch is the contract. Many companies write 2- or 3-year terms with steep early-exit fees. Always read the offboarding clause before you sign.
What Are the Common Challenges of Outsourcing Medical Billing?
Medical billing outsourcing challenges include communication gaps, slow vendor response times, performance dropping after year one, and unclear accountability when problems arise. All preventable with weekly KPI reviews, a U.S.-based account manager, and credit-back clauses tied to performance.
Who Is Responsible If an Outsourced Medical Billing Company Makes a Coding Error?
Legally, the practice is on the hook for any code submitted under its NPI, even if the vendor coded it. That is why the BAA, errors-and-omissions insurance, and contractual indemnification clauses matter. A serious vendor carries E&O coverage and contractually accepts responsibility for errors caused by their team. Always confirm this in writing before signing.
Do Medical Billing Outsourcing Companies Work With All EHR Systems?
Most reputable agencies work across the major platforms (Epic, athenahealth, eClinicalWorks, NextGen, Kareo, AdvancedMD, and others). Integration depth varies, and a vendor used to one EHR may struggle with yours.
How Do You Maintain HIPAA Compliance When Outsourcing Medical Billing?
You maintain HIPAA compliance for outsourcing medical billing through a signed BAA, SOC 2 Type II or HITRUST certification, secure VPN access, encrypted data transfer, and documented HIPAA training for all staff handling PHI. Country alone does not determine risk. Vendor maturity does.
What is the Difference Between RCM and Medical Billing Outsourcing?
Medical billing outsourcing is a subset of RCM. Billing covers coding, claim submission, denial work, payment posting, and patient collections. RCM is broader, including patient access, scheduling, eligibility, prior authorization, and analytics across the full revenue cycle.
How Do Outsourced Medical Billing Companies Handle Denials?
Strong vendors triage every denial by reason code, fix the root cause, and file appeals with payer-specific documentation. Ask for the vendor’s denial recovery rate. Best-in-class is above 65%; below 50% means denials are getting written off, not worked.
Is It Safe to Outsource Medical Billing Offshore?
Yes, offshore outsource medical billing is safe with the right controls. SOC 2 Type II audits, signed BAAs covering offshore subprocessors, secure VPN access, no offshore PHI storage, and documented HIPAA training. The risk is not the country. It is whether the vendor runs the right controls.
What Reports Should You Expect From an Outsourced Medical Billing Vendor?
Real-time dashboards covering NCR, days in AR, AR aging buckets, denial rate, denial recovery rate, payer mix, and cash collected. Plus monthly trend reports against benchmarks. Monthly PDFs only mean the vendor is filtering what you see.







