Running a medical practice in 2026 is not what it used to be. It is not just about seeing patients and sending out bills anymore. It is a full operation, with moving parts that touch every corner of your day. Staffing, compliance, software, billing, credentialing, and patient experience.
A lot of practice owners figure out the hard way that when the management side of the practice falls apart, the clinical side suffers too. Burned-out staff, delayed reimbursements, compliance gaps that turn into audits. Patients who stop coming back because scheduling was a nightmare.
This guide covers everything, including what medical practice management actually means, how to build a system that works, which software platforms are worth considering, and how revenue cycle management works from start to finish. We will also explain what credentialing involves, when to bring in a medical practice management consultant, and how specialty practices from nephrology to ENT face their own unique management challenges.

Table of Contents
ToggleWhat is Medical Practice Management?
Medical practice management is the business side of healthcare delivery. It is every system, process, and decision that keeps your practice running smoothly so that clinicians can focus on patient care without constantly fighting fires in the background.
It covers scheduling and front desk operations, billing, coding, and insurance, along with hiring, training, and keeping good staff. Apart from that, it includes staying compliant with a regulatory environment that seems to add new requirements every year.
The Five Pillars of Practice Management
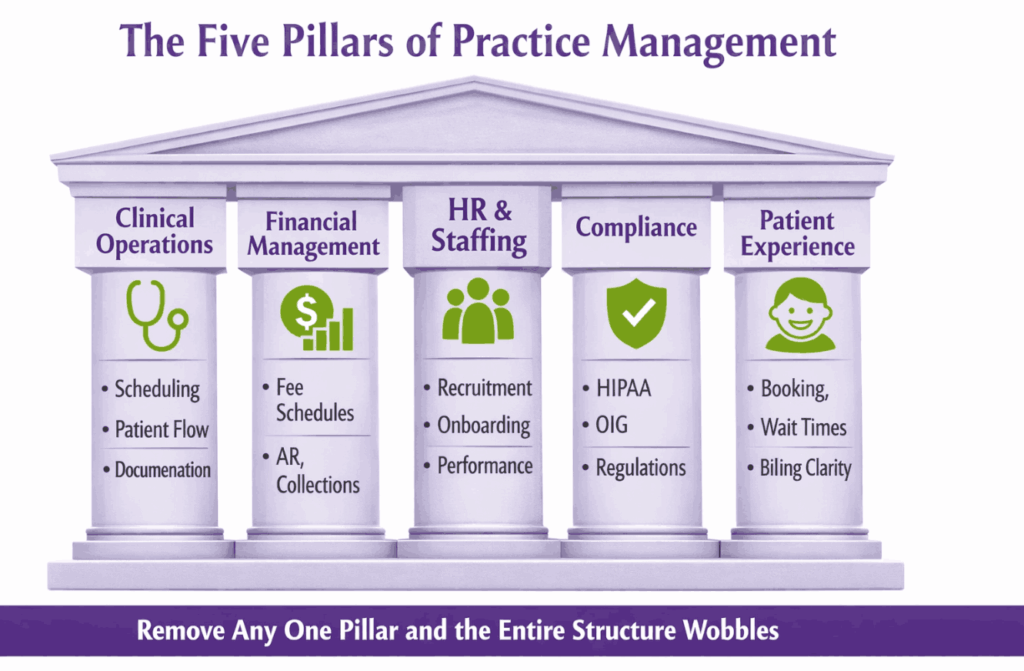
- Clinical operations include scheduling, patient flow, documentation workflows, and making sure the clinical team has what they need to work efficiently.
- Financial management covers everything from fee schedules and payer contracts to accounts receivable, collections, and financial reporting.
- HR and staffing means recruiting the right people, onboarding them well, paying them fairly, managing performance, and creating a workplace that people actually want to come back to.
- Compliance is the area most practices underinvest in until something goes wrong. HIPAA, OIG guidelines, payer rules, state regulations. It is not glamorous work, but it protects everything else.
- Patient experience is the piece that directly affects your reputation and your retention numbers. How easy is it to book an appointment? How long do patients wait? How clear is the billing process?
How Practice Management Has Changed
Post-pandemic healthcare looks different, as telehealth is no longer optional for most practices. Patient expectations around convenience have shifted significantly. Staffing shortages have pushed practices to rethink how they operate, and payer scrutiny has only increased.
Managing a medical practice today requires more sophistication than it did five years ago. The practices that are doing well are not necessarily the biggest ones. They are the ones who built solid management systems and kept improving them.
Key Roles in a Well-Run Practice
The practice manager oversees daily operations and is the connective tissue between clinical and administrative functions. The administrator handles the business and compliance infrastructure. The billing specialist owns the revenue cycle. The credentialing coordinator manages provider enrollment and re-credentialing timelines.
In smaller practices, one person often wears multiple hats. That is fine, but what matters is that someone owns each function, not that there is a separate person for every role.
Comprehensive Medical Practice Management: The 360-Degree Framework
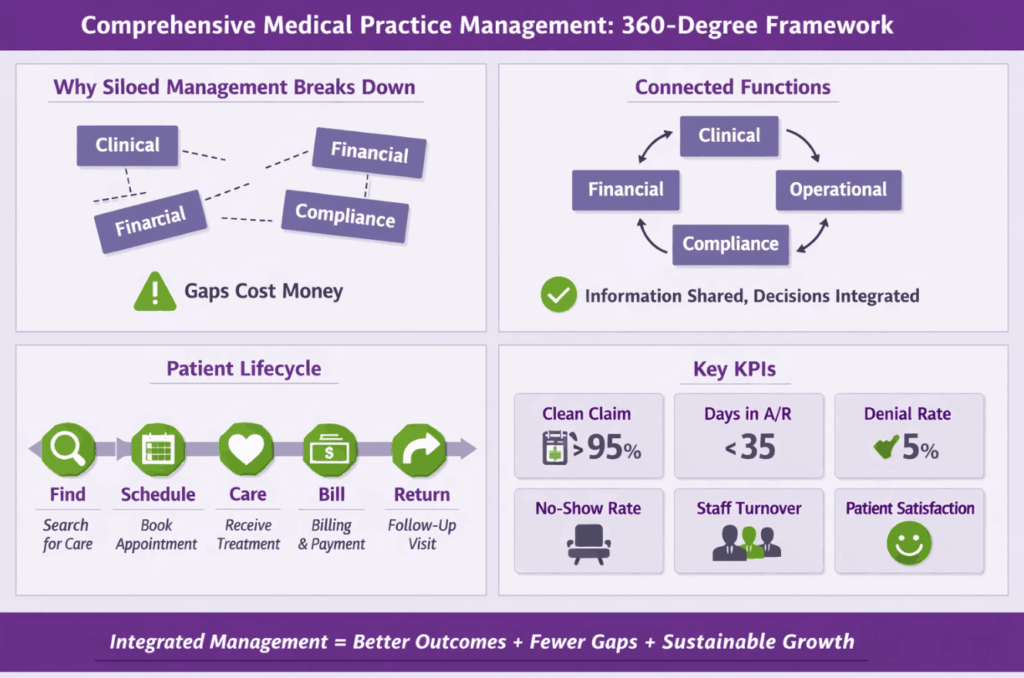
Why Siloed Management Breaks Down
Each department doing its job in isolation creates friction at every handoff, which costs money.
- The EHR is solid, but the billing staff was never trained on it properly, so claims go out with documentation gaps.
- The clinical team documents thoroughly, but the front desk is not verifying insurance eligibility before appointments, so denials pile up downstream.
- Compliance is well-managed on paper, but staff turnover is so high that nobody remembers the protocols after six months.
Connecting Clinical, Financial, Operational, and Compliance Functions
A comprehensive approach means these four areas are not operating independently. They share information, they support each other, and decisions in one area account for the impact on the others.
When a practice adds a new service line, for example, that decision touches all four areas at once. The clinical team needs protocols. The billing team needs codes and payer rules. Operations needs scheduling templates. Compliance needs documentation standards. All of that needs to happen together, not sequentially.
The Patient Lifecycle View
One of the most useful frameworks for evaluating practice management is tracing the patient lifecycle. A patient finds your practice, gets scheduled, receives care, receives a bill, and either comes back or does not. Every transition in that sequence is a management problem waiting to be solved.
A clunky scheduling process loses patients before they arrive. Poor clinical documentation creates billing errors after they leave. A confusing bill with no payment options makes them less likely to return. Managing the practice well means managing every one of those handoffs, not just the ones that seem most visible.
KPIs That Actually Tell You Something
Clean claim rate (target above 95 percent), Days in accounts receivable (target below 35 days), first-pass denial rate (target below 5 percent), patient no-show rate, staff turnover rate, and patient satisfaction scores. These metrics tell you exactly where the practice is losing revenue and where operations are breaking down.

Top Medical Practice Management Software Systems
The software conversation in healthcare can get overwhelming fast. Every vendor has a pitch, and every platform claims to do everything. Before you start comparing, get clear on what your practice actually needs.
Start with EHR integration. If your clinical and administrative systems do not talk to each other, you will spend a lot of time on manual data entry and reconciliation, which is expensive and error-prone. Also consider scheduling capabilities, billing and coding support, reporting and analytics, scalability as your practice grows, and how much training the platform requires.
Top Medical Practice Management Software Systems Worth Considering in 2026
- Athenahealth is a strong option for practices that want a cloud-based system with built-in RCM services. It works particularly well for medium to large practices that want to outsource some of the billing burden.
- Kareo (now part of Tebra) is popular with smaller independent practices. It is relatively easy to use and includes billing, scheduling, and a basic EHR.
- AdvancedMD offers robust reporting and is well-suited for specialty practices that need more customization.
- DrChrono is a good fit for mobile-first practices and works well on iPad. It has strong customization options.
- Epic is the enterprise standard. If you are affiliated with a health system or running a large multi-specialty group, Epic is likely already in the picture.
- Modernizing Medicine is specialty-specific and has particularly strong products for dermatology, orthopedics, ophthalmology, and gastroenterology.
Cloud-Based vs. On-Premise in 2026
Cloud-based systems now dominate the market and offer significant advantages in terms of accessibility, automatic updates, and lower upfront infrastructure costs. On-premise systems may be preferred by larger organizations with dedicated IT departments and specific data sovereignty requirements.
No software system solves management problems on its own. The best medical practice management software creates operational efficiency when it is implemented thoughtfully, configured correctly, and used consistently by a trained team.
Questions to Ask Any Vendor
The best medical practice management is not the most expensive solution or the most comprehensive one. It is the solution that matches the specific needs, size, and growth trajectory of the practice. When evaluating medical practice management services, the most important questions to ask are:
- How does the vendor handle transitions if a key team member leaves their organization?
- What specific outcomes has this vendor delivered for practices similar to ours?
- What does the service level agreement guarantee, and what are the remedies if those guarantees are not met?
- Who will be our day-to-day contact, and what is their experience level?
Revenue Cycle Management for Medical Practices
Revenue cycle management is the process that converts clinical services into collected revenue. When it works well, cash flow is predictable, and the practice is financially healthy. When it breaks down, even a busy practice can struggle to make payroll.
Most practices have leaks in their revenue cycle that they are not fully aware of. Common issues include eligibility not being verified before appointments, charge capture gaps, coding errors, claims going out without proper scrubbing, and denials that never get worked.
The Complete RCM Lifecycle
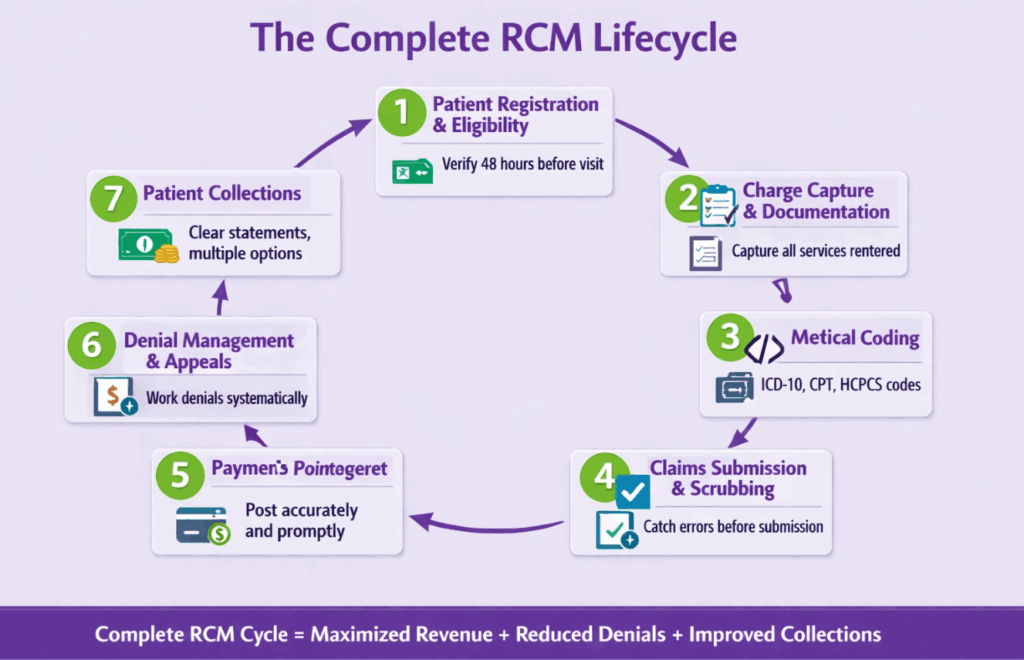
1. Patient Registration and Eligibility Verification
The cycle starts with collecting accurate patient demographics and verifying insurance eligibility before the appointment, which prevents a significant number of downstream problems. Eligibility verification should happen at least 48 hours before the scheduled visit, not at the front desk while the patient is standing there.
2. Charge Capture and Documentation
After the visit, every service rendered needs to be captured. Charge capture gaps are one of the most common sources of lost revenue, and if a provider performs a service that never makes it onto the claim, that revenue is simply gone.
3. Medical Coding
Coding converts clinical documentation into billable codes. Getting this right requires trained coders who understand ICD-10, CPT, and HCPCS, as well as the specific documentation requirements for each code. Undercoding leaves money on the table, while overcoding creates compliance risk.
4. Claims Submission and Scrubbing
Before a claim goes to the payer, it should go through a scrubbing process that catches common errors. Missing modifiers, mismatched diagnosis and procedure codes, and invalid NPI numbers. A good scrubbing process keeps your clean claim rate high and prevents denials before they happen.
5. Payment Posting
When payments come in from payers and patients, they need to be posted accurately and promptly. Errors in payment posting create problems in accounts receivable reporting and can mask collection issues.
6. Denial Management and Appeals
Denials are not the end of the road, and a well-run practice works every denial systematically, determines the root cause, files appeals where appropriate, and tracks denial trends over time to fix systemic issues.
7. Patient Collections and Statements
With patient responsibility portions growing, collecting from patients has become a more significant part of the revenue cycle. Clear statements, multiple payment options, and proactive financial counseling all improve collection rates.

In-House vs. Outsourced RCM
Keeping RCM in-house gives you direct control and visibility into every step of the process. It also requires trained and experienced staff, ongoing oversight, and the right technology infrastructure. Outsourcing to an RCM company can reduce overhead costs and bring specialized expertise, particularly in denial management and payer-specific billing rules.
The tradeoff is less direct control and the need to manage a vendor relationship with clear accountability metrics built into the contract. Some practices use a hybrid model, keeping charge capture and payment posting in-house while outsourcing credentialing or denial management to a specialized team.
Benchmark Metrics to Know
- Clean claim rate above 95 percent.
- First-pass resolution rate above 90 percent.
- Denial rate below 5 percent.
- Days in accounts receivable below 35.
If your numbers are significantly worse than these benchmarks, there is revenue leaking somewhere.
Medical Practice Management Services
Some practices want to hand off all administrative functions to a management company. Others want to keep most things in-house and outsource only specific pieces. Both approaches work. The right choice depends on your practice size, internal capacity, and comfort level with outside vendors.
Core Services Available for Outsourcing
- Billing and coding are the most commonly outsourced functions. A good billing company brings specialized expertise and takes responsibility for claim accuracy and denial resolution.
- Credentialing management involves keeping provider credentials current with payers and organizations. It is detail-intensive work that benefits from dedicated attention.
- HR and payroll outsourcing can reduce administrative burden, especially for smaller practices without a dedicated HR team.
- Compliance monitoring services keep your practice current with changing regulations and reduce audit risk.
- IT and EHR support covers system maintenance, security, and user support so your team can focus on patient care.
- Telehealth integration has become a standard service offering as virtual care has become part of routine practice operations.
Benefits and Risks of Outsourcing
The benefits of outsourcing to medical practice management services include cost savings, access to specialized expertise, and the ability to scale services as the practice grows.
The risks include vendor dependency, data security concerns, and the possibility that an outside vendor may not know your practice as well as your own team does. So, vet vendors carefully, check references, and read contracts before signing.
Credential Management for Medical Practices
This is the piece that gets underestimated most consistently. A provider who is not credentialed with a payer cannot bill that payer for services rendered. If a new hire begins seeing patients before their credentialing is complete, those visits may generate no reimbursement at all. Credentialing delays are one of the most common and entirely preventable causes of cash flow problems when practices bring on new providers.
Provider Enrollment vs. Credentialing
These terms are often used interchangeably, but they refer to different processes. Credentialing is the verification process, confirming that a provider has the education, training, licensure, board certification, and malpractice history they claim to have. Whereas, Provider enrollment is the process of registering a credentialed provider with a specific payer, so they can bill for services.
The Credentialing Lifecycle
Primary Source Verification
This involves verifying a provider’s credentials directly with the issuing institutions. Medical school, residency, board certification, licensure, and malpractice history. This takes time and requires organized documentation.
Payer Enrollment
Each payer has its own enrollment process and timeline. Medicare and Medicaid enrollment through PECOS is a separate process from commercial payer enrollment. CAQH is the central repository most payers use for provider data, and keeping CAQH profiles current is a basic requirement for smooth credentialing.
Re-credentialing
Payer contracts require periodic re-credentialing, as credentials and licenses expire. A credentialing coordinator who tracks these timelines prevents lapses that interrupt billing.
How to Avoid Common Delays
Start the process early, ideally 90 to 120 days before a new provider’s start date. Keep a complete and organized credentialing file for every provider. Make sure CAQH profiles are complete and attested regularly. Follow up with payers consistently rather than waiting for them to respond.
Medical Practice Management Consultants

Declining collections despite stable or growing patient volume. Staff turnover keeps accelerating without a clear explanation, and a compliance gap that feels too complex to address with internal resources. Moreover, the Rapid growth that the existing management infrastructure cannot support. A payer audit revealed problems the practice leadership was not aware of. Any one of these is a reasonable trigger for bringing in a consultant with relevant experience.
What a Consultant Actually Does
A good practice management consultant comes in, looks at how your practice actually operates (not how you think it operates), identifies where the problems are, and helps you fix them. That might involve an operational audit, a financial analysis, a workflow redesign, a compliance gap review, or some combination.
The value is in the outside perspective. When you are inside a practice every day, it is genuinely hard to see the patterns that are obvious to someone looking at it fresh.
Generalist vs. Specialty-Specific Consultants
A generalist consultant can address broad operational and financial issues. If your practice has specialty-specific billing complexity or regulatory challenges, a consultant with direct experience in your specialty will be more useful.
How to Vet a Consultant?
Ask for case studies from similar practices, check references, and understand exactly what deliverables are included in the engagement. A good consultant should be able to tell you, in plain language, what they will do and what outcomes you can reasonably expect.
Medical Practice Management Solutions: Building Your Stack
Technology Solutions
Cloud-based practice management platforms, AI-assisted scheduling that reduces no-shows, telehealth infrastructure, and patient portals that reduce phone volume are the technology foundations most practices need today. The key is integration. A collection of tools that do not share data creates more work, not less.
Operational Solutions
Lean workflow principles applied to patient flow can significantly reduce wait times and improve throughput without adding staff. Patient flow mapping, where you trace exactly what happens from arrival to discharge, often reveals surprising inefficiencies. Weekly staff huddles keep the team aligned and surface problems before they become larger issues.
Financial Solutions
RCM automation handles repetitive billing tasks more consistently than manual processes. Regular payer contract analysis makes sure your fee schedules are competitive. A structured denial management workflow with clear ownership and accountability prevents revenue leakage.
Human Capital Solutions
Staff retention starts with onboarding. A new employee who feels lost in their first weeks is much more likely to leave. Structured training programs, clear performance expectations, and regular feedback create the conditions for people to stay and grow.
Compliance Solutions
HIPAA risk assessment tools, OIG exclusion check services (run these monthly, not just at hire), and audit readiness software reduce your exposure. Compliance is not a one-time project, but an ongoing system.
Medical Practice Management Training
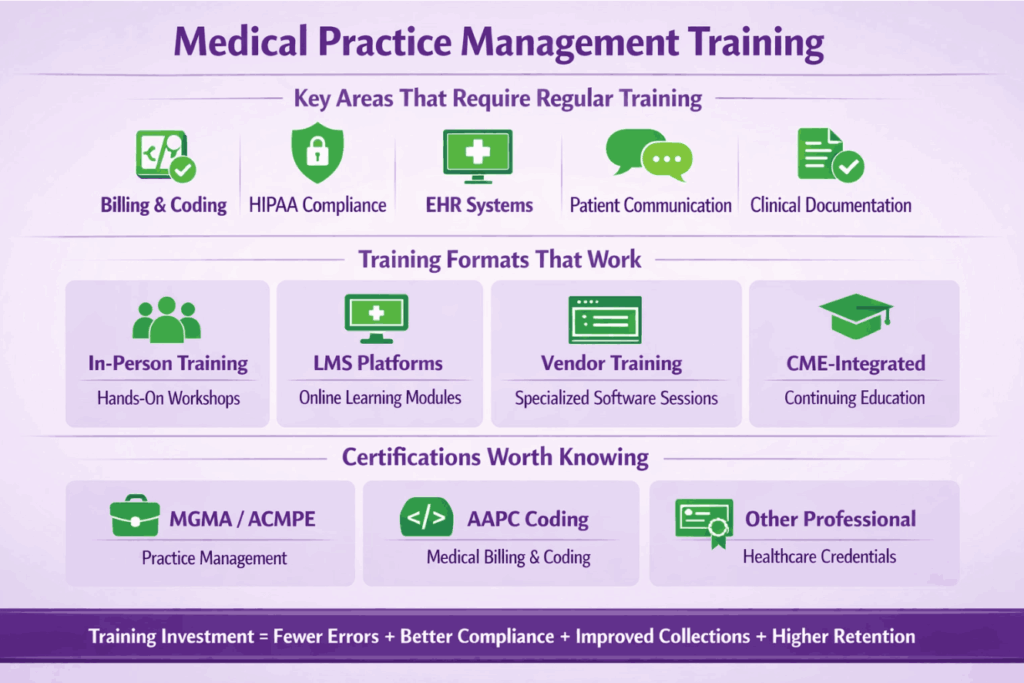
This is one of the most underinvested areas in practice management. Staff who are not properly trained make billing errors, create compliance risks, and frustrate patients. The cost of those errors is almost always higher than the cost of the training that would have prevented them.
Key Areas That Require Regular Training
Billing and coding accuracy changes every year with code updates. HIPAA compliance training needs to be refreshed annually. EHR systems need ongoing training as features change and new staff join.
Patient communication skills, particularly around financial conversations, make a significant difference in collections. Clinical documentation that supports billing requirements is something providers themselves need to understand.
Training Formats That Work
In-person training works well for hands-on skills and team building. Learning management system (LMS) platforms allow for flexible, self-paced training that fits busy schedules. Vendor-provided training for specific software is often underused but genuinely valuable. CME-integrated training helps providers meet continuing education requirements while addressing practice-specific skills.
Certifications Worth Knowing
The Medical Group Management Association (MGMA) and the American College of Medical Practice Executives (ACMPE) offer respected credentials for practice managers. The American Academy of Professional Coders (AAPC) provides coding certifications that are widely recognized by payers. Encouraging staff to pursue these credentials invests in both skill and retention.
Specialty-Specific Practice Management Strategies
Every specialty has its own billing language, regulatory environment, and operational challenges. General practice management principles apply everywhere, but the implementation details vary significantly. Here is a breakdown of what matters most in each specialty area.
Nephrology Practice Management
Nephrology billing is among the most complex in medicine. Dialysis billing follows monthly global billing cycles with specific rules about how many visits trigger a monthly capitation payment. ESRD program compliance adds another layer of regulatory oversight.
Chronic care management codes represent a significant revenue opportunity for nephrologists that many practices are not fully capturing.
Key payer rules around dialysis frequency, home dialysis oversight, and transitional care management all require specific coding knowledge. Staffing for a nephrology practice also needs to account for the demands of dialysis facility coverage, which affects scheduling in ways that other specialties do not face.
OBGYN Practice Management
Obstetrics and gynecology billing operate on two very different tracks. Obstetric care uses global billing periods, where prenatal visits, delivery, and postpartum care are typically bundled into a single payment.
Getting the global billing right, including managing when patients transfer care or deliver outside the expected window, requires careful documentation and coding.
Gynecologic billing is more straightforward but has its own coding nuances, particularly around preventive services, procedures, and the line between diagnostic and preventive colonoscopies or biopsies.
Reproductive health regulations have also created new compliance considerations that practices need to track actively.
Oncology Practice Management
Oncology practice management involves some of the highest-stakes financial management in medicine. Drug billing, particularly for infused chemotherapy agents, represents enormous revenue and significant compliance risk.
The 340B drug pricing program offers cost savings for qualifying practices, but program compliance requires meticulous record-keeping.
Prior authorization burdens in oncology are substantial. Many practices dedicate significant staff time to obtaining and managing authorizations for treatment regimens.
Patient financial counseling is an essential service, as patients facing high out-of-pocket costs need support navigating their options. Oncology Care Model and other value-based care arrangements are reshaping how oncology practices get paid.
Cardiology Practice Management
Cardiology practice management is shaped by the volume and complexity of diagnostic procedures. Echocardiograms, stress testing, cardiac catheterization, and electrophysiology procedures all have specific billing rules and documentation requirements.
Device clinic management adds an operational dimension unique to cardiology. Managing patients with implanted cardiac devices requires structured follow-up workflows and specific billing codes.
MIPS performance reporting is particularly consequential for cardiologists, and practices that ignore quality reporting are leaving significant revenue on the table.
Managing high-acuity patients across inpatient, outpatient, and telehealth settings requires coordination systems that many smaller cardiology practices have not yet formalized.
Radiology Practice Management
Radiology practice management has been transformed by teleradiology. The ability to read studies remotely has changed staffing models and created new credentialing requirements as radiologists may now need credentials at multiple facilities.
RVU-based productivity models are standard in radiology compensation, which creates specific management challenges around workload distribution and quality oversight.
Contrast agent billing and prior authorization for advanced imaging add an administrative burden that requires dedicated staff attention. Radiologist credentialing is more complex than most specialties because of the multisite nature of modern radiology practice.
Podiatry Practice Management
Podiatry billing has a unique challenge that trips up many practices: the distinction between routine foot care and non-routine foot care.
Medicare specifically limits coverage of routine foot care, with exceptions for patients who meet specific systemic condition criteria. Documentation of why a service qualifies as covered care must be airtight.
Diabetic foot care is a major component of most podiatry practices and comes with specific documentation requirements that support both clinical quality and billing accuracy.
Common podiatry claim denials cluster around this routine vs. non-routine issue and can be significantly reduced with proper staff training and documentation templates.
ASC Practice Management
Ambulatory surgery centers operate under a billing and regulatory framework that is distinct from both physician office and hospital settings. ASC facility fees, implant billing, and payer-specific fee schedules require dedicated expertise.
Accreditation through AAAHC or the Joint Commission is required for Medicare certification and is a meaningful quality marker. Facility fee negotiation with commercial payers is an area where many ASCs leave significant revenue uncollected.
Infection control and quality reporting requirements have grown more rigorous in recent years and require systematic management.
Orthopedic Practice Management
Orthopedic billing is complex because of the high proportion of surgical cases, implant billing, and the frequency of workers’ compensation and auto accident claims. Each of these payer types has its own rules and documentation requirements.
Physical therapy and other ancillary services are common in orthopedic practices and require their own billing workflows and compliance considerations.
Pre-authorization management for surgical procedures is time-intensive and directly affects scheduling and revenue. Implant billing, particularly for joint replacements, requires careful invoice reconciliation and payer-specific rules.
Gastroenterology Practice Management
Gastroenterology practice management is heavily shaped by colonoscopy volume. The distinction between a preventive colonoscopy and a diagnostic colonoscopy has significant billing implications, particularly for patient cost-sharing, and documentation must clearly support the correct classification.
Anesthesia billing for GI procedures requires coordination between the practice and anesthesia providers. High procedure volumes create scheduling management challenges and require efficient workflow systems to avoid bottlenecks. Endoscopy suite management adds an operational layer that combines elements of ASC and physician practice management.
Otolaryngology Practice Management
ENT practices often generate significant revenue from in-office procedures, including allergy testing, allergy immunotherapy, audiologic testing, and sinus procedures. Each of these has specific billing requirements and compliance considerations.
Audiology and hearing aid services represent a meaningful ancillary revenue opportunity but also bring their own regulatory complexity, particularly around hearing aid dispensing rules. Surgical scheduling for ENT procedures requires coordination with the hospital and outpatient surgical facilities.
Managing both pediatric and adult patient populations means the front desk, clinical, and billing teams need fluency in both contexts simultaneously.
Best Practices in Medical Practice Management: A 2026 Checklist
1. Patient Experience
- Online scheduling available 24 hours a day, not just during office hours
- Automated appointment reminders by text and email, sent at least 48 hours in advance
- Post-visit satisfaction surveys with a documented process for acting on the feedback received
- Clear patient financial communications before the visit for any anticipated cost-sharing
- A staff-facing protocol for handling patient complaints promptly and consistently
2. Financial Management
- Monthly RCM review covering clean claim rate, denial rate, and days in accounts receivable
- Payer contract review on at least a two-year cycle, with fee schedule benchmarking against current market rates
- Annual fee schedule analysis to confirm you are not billing below what the market supports
- A structured collections workflow with clear escalation steps and defined timelines at each stage
- Monthly financial reports are reviewed by practice leadership, not just filed by the billing team
3. Operational Management
- Weekly staff huddles, even brief ones, to surface operational problems before they compound
- Quarterly workflow reviews in key departments to identify recurring inefficiencies
- KPI dashboards accessible to department managers in real time, not just available in a monthly report
- Written standard operating procedures for all recurring administrative processes
- A clear escalation path for operational problems, so issues reach the right decision-maker quickly
4. Compliance
- Annual HIPAA risk assessment with documented remediation steps and completion tracking
- Quarterly coding audits by specialty, reviewed by someone with appropriate credentials and expertise
- Monthly OIG exclusion checks for all staff and contracted vendors
- Current HIPAA training records are maintained for every employee, updated annually
- A designated compliance contact, even in smaller practices, so compliance questions have a clear owner
5. Leadership and Culture
- Consistent investment in staff development, recognition, and career growth opportunities
- An environment where staff feel safe identifying and raising operational problems
- Clear accountability for each management function, with one named owner per area
- Regular performance conversations throughout the year, not only at annual review time
- A succession plan for key administrative and clinical leadership roles







