Charge entry is a fundamental step in medical billing where patient services, diagnoses, procedures, and related charges are entered into the billing system after a clinical encounter. It converts provider documentation into billable data that can be used to generate claims and request reimbursement from insurance payers.
The charge entry workflow involves several structured steps, including receiving patient records, downloading and organizing files, allocating cases to billing staff, and entering patient demographics and insurance information. The process also includes activities such as EOB follow-up, denial analysis, and client communication to ensure billing accuracy and resolve documentation issues.
Accurate charge entry is important because it ensures proper revenue capture, reduces claim denials, improves cash flow, and maintains compliance with payer and regulatory requirements. It also supports financial reporting, minimizes revenue leakage, and strengthens overall revenue cycle management.
This guide explains what charge entry is, outlines its step-by-step process, highlights its importance in medical billing, and discusses the tools, errors, and related functions involved in the charge entry workflow.
Table of Contents
ToggleWhat is Charge Entry in Medical Billing?
Charge entry in medical billing is the process of accurately recording patient services, procedures, diagnoses, and related charges into the billing system after a clinical encounter. It converts documented medical services into billable entries using appropriate CPT, ICD, and HCPCS codes to prepare claims for submission to insurance payers.
What is the Process of Charge Entry?
The process of charge entry is a structured workflow that converts documented patient services into claim-ready billing data. It ensures that every rendered service is reviewed, coded, validated, and entered into the billing system before claim submission. The process typically includes the following key steps:

1. Receipt of Files
The receipt of files is the initial step before charge entry begins, and it ensures that all required documentation is properly gathered and organized. Medical records are typically received through Electronic Medical Record (EMR) systems, hospital portals, secure FTP servers, encrypted emails, or scanned document uploads. Once received, the records are sorted by date of service, provider name, specialty, or facility to maintain an organized workflow.
Charge entry staff must first identify and access the correct data source to ensure accuracy. This may involve logging into EMR platforms for outpatient visits, hospital information systems for inpatient services, or reviewing scanned encounter forms and EHR exports. Access is granted through secure credentials and role-based permissions to ensure only authorized personnel can retrieve sensitive patient information.
After accessing the records, a detailed review is conducted to identify missing information, documentation gaps, or potential errors. Staff verifies that patient demographics are complete, dates of service are accurate, provider details are documented, and diagnosis and procedure information are clearly stated. They also confirm that required authorizations, referrals, and provider signatures are present. If discrepancies are identified, clarification is requested from the provider before proceeding further.
Throughout this process, strict compliance with HIPAA regulations and data protection standards is maintained. Records are accessed through encrypted systems, stored in secure folders with restricted permissions, and monitored through audit trails. Secure access controls and confidentiality protocols ensure patient information remains protected at every stage of the charge entry process.
2. File Download
The file download stage involves securely accessing client portals or EMR systems to retrieve required patient records for charge entry. Authorized staff logs into encrypted portals using secure credentials and, where applicable, multi-factor authentication. Access is granted based on role-specific permissions to ensure only relevant records are viewed and downloaded. Before downloading, the staff confirms the correct date of service, provider, and encounter type to prevent selection errors.
Once downloaded, documents such as PDFs, scanned images, or EHR exports are opened and reviewed carefully without modifying the original content. If format conversion is required for system compatibility, it is performed using secure tools that preserve document integrity and prevent data alteration. Files are handled in read-only mode whenever possible to ensure that the original medical record remains unchanged.
Standardized file naming conventions are followed to maintain consistency and improve retrieval efficiency. File names typically include elements such as client name, provider name, date of service, and encounter number. Organized folder structures are maintained by specialty, provider, or service date to streamline workflow and reduce confusion. This structured storage system ensures that records can be easily located during audits, reviews, or follow-ups.
To maintain record integrity, checks are performed to confirm that downloads are complete and not corrupted. File sizes and page counts are verified against the source to ensure no pages are missing. During transfer and storage, files are kept within secure servers or encrypted drives with restricted access permissions. Audit logs track downloads and file activity to ensure compliance with HIPAA and data security standards.
3. File Allocation
File allocation is the step where downloaded and verified records are assigned to the charge entry staff for processing. Cases are distributed based on specialty, coder expertise, and specific client requirements to ensure accuracy and efficiency. For example, complex specialties may be assigned to experienced team members who are familiar with specialty-specific coding guidelines and payer policies.
Workload distribution is managed using structured allocation methods. Some organizations follow a specialty-based model, where staff handle only specific practice areas. Others use volume-based allocation to balance daily encounter counts among team members. Team-based or shift-based distribution models are also implemented to ensure continuous workflow coverage and timely processing.
Supervisors regularly monitor productivity levels, turnaround times (TAT), and daily volume targets to prevent backlogs. Performance dashboards and workflow tracking tools help identify bottlenecks or uneven workload distribution. If delays are detected, cases may be reassigned or additional resources deployed to maintain efficiency and service-level agreements.
Urgent, high-value, or time-sensitive cases are flagged within the system for priority handling. These may include stat encounters, nearing timely filing deadlines, high-dollar procedures, or accounts requiring immediate submission. Prioritization protocols ensure that critical cases are processed first, supporting faster claim submission and improved revenue flow.
4. Entry of Patient Demographics
The entry of patient demographics is a critical step in charge entry because even minor inaccuracies can lead to claim rejections. Patient details such as full name, contact information, and insurance policy data are carefully entered into the billing system. Insurance information must be recorded exactly as documented on the insurance card or within the EMR.
After data entry, a cross-checking process is performed to prevent mismatches. The entered information is verified against the original source documents, such as the EMR record, scanned registration forms, or insurance card copies. Staff confirms spelling accuracy, correct sequencing of names, accurate policy numbers, and proper relationship codes for dependents.
Before charge submission, active coverage and payer details are verified. Eligibility checks are performed electronically or through payer portals to confirm that the insurance policy was active on the date of service. Staff verifies plan type, copayment requirements, deductible status, and referral or authorization needs.
Common data entry errors include typographical mistakes in member IDs, incorrect dates of birth, wrong insurance selection, duplicate patient profiles, and outdated policy information. Preventive checks, such as automated validation rules, mandatory field prompts, duplicate record alerts, and eligibility verification tools, are used to minimize these errors.
5. EOB Follow Up
EOB follow-up involves carefully reviewing the Explanation of Benefits (EOB) to understand how a claim was processed by the payer. The EOB outlines the billed amount, allowed amount, payment issued, adjustments applied, denial reasons if any, and the portion assigned to patient responsibility.
After reviewing the EOB, payments are matched against the originally submitted charges and the amounts posted in the billing system. Staff confirms that payment amounts, adjustment codes, and write-offs are accurately reflected in the system. Any discrepancies between the EOB and posted data are flagged for correction to maintain accurate financial records.
During this stage, payment variances and contractual underpayments are identified by comparing the allowed amount to the agreed fee schedule. Coding-related reductions, bundling adjustments, modifier impacts, or processing errors are analyzed to determine whether they were applied correctly. Trends in repeated reductions or unexpected adjustments are monitored to detect systemic issues or payer inconsistencies.
If discrepancies are identified, the billing team contacts the payer through secure portals or customer service channels to seek clarification. Supporting documentation may be submitted to justify services or request reconsideration. In cases of underpayment or improper denial, formal appeals are prepared and submitted within the payer’s defined timelines.
6. Denial Analysis
Denial analysis is the systematic review of rejected or unpaid claims to identify the exact reason for nonpayment. The process begins by examining denial codes, payer remarks, and claim details provided in the remittance advice or EOB. Staff reviews the specific adjustment reason codes, remark codes, billed services, modifiers, and documentation to determine whether the issue relates to eligibility, coding, authorization, or submission errors.
Once identified, denials are classified into defined categories such as eligibility issues, incorrect patient demographics, coding errors, missing modifiers, lack of prior authorization, timely filing violations, or documentation deficiencies. Categorizing denials helps prioritize corrective actions and track trends more effectively.
Recurring denial patterns are analyzed through denial reports and performance dashboards. Trends may reveal weaknesses in front-end verification processes, coding accuracy, documentation quality, or claim submission timing. For example, repeated eligibility denials may indicate inadequate insurance verification, while frequent coding denials may signal training gaps or inconsistent guideline interpretation.
Corrective measures are then implemented to prevent repeat denials. These may include correcting and resubmitting claims, filing formal appeals with supporting documentation, updating internal workflows, strengthening pre-submission audits, or conducting targeted staff training sessions.
7. Client Feedback
Client feedback is an essential component of the charge entry process because it ensures alignment between billing teams and healthcare providers. Regular communication is maintained with providers or clients to clarify incomplete documentation, resolve coding uncertainties, and address billing discrepancies. Queries are documented and shared through secure communication channels, and updates are provided regarding claim status, denial reasons, and corrective actions taken.
Performance metrics such as error rates, productivity levels, turnaround time (TAT), and denial trends are systematically tracked and reported. Detailed reports are generated weekly or monthly to provide transparency into operational efficiency and financial outcomes. These reports highlight processing volumes, quality scores, and areas requiring attention.
Feedback, audit findings, and performance data are analyzed to refine internal workflows and reduce recurring issues. If trends show frequent documentation gaps or coding inconsistencies, targeted improvements are implemented. This may include updating process checklists, revising allocation methods, or conducting refresher training sessions for staff.
To maintain high service standards, structured quality control measures and internal audits are performed regularly. Random file reviews, compliance checks, and coding validations help ensure adherence to payer guidelines and regulatory standards. Secure documentation practices, HIPAA compliance monitoring, and corrective action tracking further strengthen accountability.
What is the Importance of Charge Entry in Medical Billing?
The importance of charge entry in medical billing is in multiple ways, as discussed below:
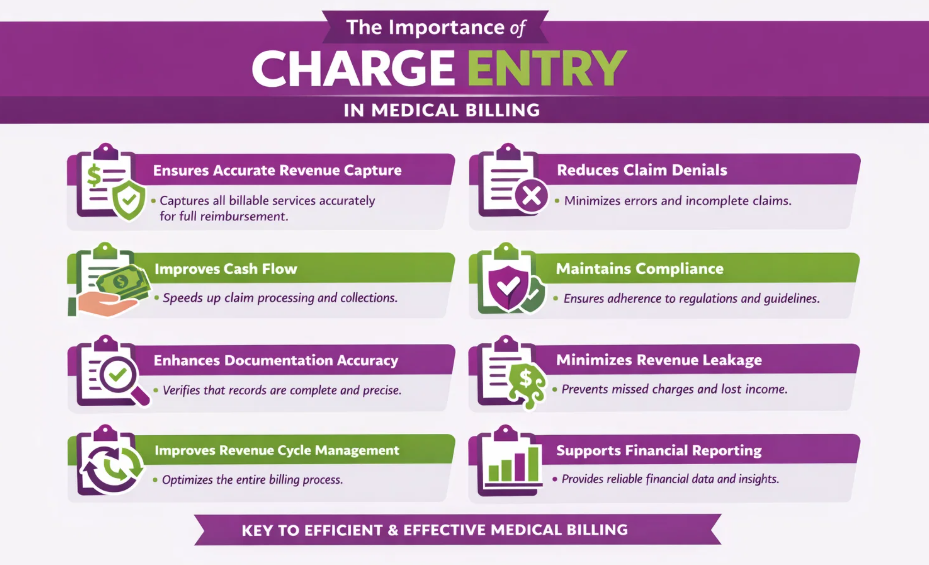
Ensures Accurate Revenue Capture
Accurate revenue capture refers to the process of recording all services provided to patients in a way that ensures the healthcare practice receives full and proper reimbursement for the care delivered. It guarantees that every billable service is accounted for, coded correctly, and submitted for payment.
To achieve this, diagnosis and procedure codes are carefully assigned based on clinical documentation, and the corresponding charges are posted into the billing system. Each encounter is reviewed to ensure all documented services are captured, and no billable activity is missed. Cross-verification between clinical notes and entered codes ensures consistency and compliance with coding guidelines and payer requirements.
Additional checks, such as auditing modifiers, units, and patient demographics, are performed to confirm that all billable services are recorded accurately. These steps help prevent revenue leakage, reduce claim denials, and maximize reimbursement for the healthcare organization.
Reduces Claim Denials
Claim denials occur when a payer refuses to reimburse a submitted medical claim, either partially or fully, due to errors, missing information, or noncompliance with payer rules. Reducing claim denials is essential to maintain cash flow and avoid delays in revenue collection.
To minimize denials, verification steps are conducted before claim submission. This includes checking for coding accuracy, confirming patient demographics, verifying insurance eligibility, and ensuring all required documentation is complete. A thorough pre-submission review ensures that all claim fields, procedure and diagnosis codes, modifiers, and authorizations are properly entered.
Quality control measures, such as automated claim scrubbing tools, internal checklists, and supervisory reviews, are implemented to increase first-pass claim acceptance. Additionally, internal audits and system checks detect inconsistencies, duplicate entries, or missing information, allowing corrections before submission.
Improves Cash Flow
Cash flow in a healthcare practice refers to the movement of money into the organization from patient services and insurance reimbursements. This is essential for sustaining operations and funding future care.
Streamlined charge entry and validation steps contribute to faster claim preparation and submission, allowing payers to process claims promptly. Accurate and timely charge entry prevents payment holds, reduces rework, and ensures that claims are adjudicated without unnecessary delays. Efficient workflows help minimize outstanding receivables, accelerate collections, and maintain a steady inflow of revenue.
By following a structured timeline from charge entry to claim transmission, practices can maintain consistent turnaround times (TAT). This leads to overall cash flow stability and supports the financial health of the organization.
Maintains Compliance
Compliance maintenance in medical billing ensures that all billing practices follow federal and state regulations, payer policies, and industry guidelines to avoid legal and financial penalties. It protects the practice against audit risks and improper reimbursement.
Charge entry practices maintain compliance by accurately coding diagnoses and procedures according to established guidelines, verifying patient eligibility, and adhering to payer-specific rules. Controls such as automated edits, internal audits, and workflow checks are implemented to prevent upcoding, duplicate billing, unbundling, and submission of false claims.
Comprehensive documentation is required to support medical necessity and all billed services. This includes provider notes, encounter forms, authorizations, and clinical evidence that justify the procedures performed. Ensuring that every charge is backed by appropriate documentation protects the practice from compliance violations and supports accurate, defendable billing.
Enhances Documentation Accuracy
Documentation accuracy refers to the completeness and correctness of clinical and billing records. Accurate documentation ensures that all services provided are properly recorded and supported for reimbursement.
Before finalizing charges, patient demographics and clinical records are cross-checked against source documents to confirm accuracy. Diagnosis and procedure codes are carefully reviewed to ensure they match the documented services and comply with coding guidelines.
Review steps include identifying discrepancies, missing information, inconsistencies in coding, or incomplete notes that could lead to claim denials. Additional measures, such as internal audits, automated edits, and validation checklists, are used to confirm that all records are complete, accurate, and compliant with billing standards. Supports Financial Reporting
Minimizes Revenue Leakage
Revenue leakage refers to the loss of potential income when billable services are not captured, coded, or submitted for reimbursement. It can occur due to missed charges, coding errors, or incomplete documentation.
To prevent revenue leakage, all billable services are carefully reviewed and captured before claim submission. Checks are performed to identify unentered procedures, missing modifiers, or ancillary services that may have been overlooked.
Reports and system alerts are used to track encounters that have not yet been billed, ensuring nothing is missed. Daily or periodic reconciliation between clinical documentation and posted charges is conducted to verify that all services provided are accounted for in the billing system.
Improves Overall Revenue Cycle Management (RCM)
The process of Revenue Cycle Management (RCM) is the end-to-end management of a healthcare organization’s financial transactions. It begins from patient registration and charge capture to claim submission, payment posting, and accounts receivable follow-up. Effective RCM ensures timely reimbursement and financial stability.
Charge entry is a critical component of RCM that connects clinical documentation with coding, claim submission, payment posting, and A/R follow-up. Accurate charge entry improves clean claim rates, reduces denials, accelerates payment, and enhances overall collections efficiency.
Coordination between clinical, billing, and finance teams ensures that workflows are streamlined, discrepancies are resolved promptly, and information flows seamlessly from service documentation to payment posting. Performance monitoring, internal audits, and feedback loops are used to identify errors, optimize processes, and continuously refine the charge entry workflow.
What Tools are Used in the Charge Entry Process in Medical Billing?
Tools that are used in the charge entry process are designed to streamline workflows, ensure accuracy, and maintain compliance across the revenue cycle. The primary tools include:
- Electronic Medical Record (EMR) Systems – Used to access and review patient clinical documentation, encounter notes, and medical histories.
- Practice Management (PM) Software – Facilitates scheduling, patient registration, billing, and tracking of claims throughout the revenue cycle.
- Medical Coding Software – Provides coding assistance for CPT, ICD, and HCPCS codes, ensuring accurate and compliant charge entry.
- Charge Capture Tools – Enables clinicians and staff to record services provided in real-time or post-encounter for accurate billing.
- Clearinghouses – Acts as intermediaries to review, validate, and transmit claims to payers, reducing errors and rejections.
- Fee Schedule and Payer Contract Management Tools – Helps verify contracted rates, allowed amounts, and billing rules for different payers.
- Audit and Compliance Tools – Supports internal audits, validation checks, and adherence to HIPAA and payer regulations.
- Revenue Cycle Management (RCM) Systems – Integrates charge entry with claim submission, payment posting, denial management, and reporting to optimize the entire revenue cycle.
What are the Possible Errors in Charge Entry?
Charge entry mistakes generally fall into several categories. Common coding and data entry errors include entering the wrong CPT or ICD-10 codes, missing required modifiers, using outdated codes, or transposing numbers. Patient/data inaccuracies are also frequent mistakes. Other categories include duplicated or missing charges and authorization/insurance errors.
These errors often arise from root causes such as rushed data entry, incomplete or unclear provider documentation, lack of standardized workflows, or insufficient staff training. The consequences of charge entry errors can be serious. Mistakes usually force claims to be corrected or rewritten, leading to administrative delays and lost revenue.
Common real-world examples include entering an office visit on the wrong date or without the appropriate modifier cause a denial or partial payment. Even a simple typo can bounce a claim. Likewise, if a clinic forgets to enter a lab test or procedure at all, that service goes unbilled. In another scenario, a physician might document a treatment, but the biller selects the wrong CPT code. In this case, the insurers will see a mismatch between the reported diagnosis and procedure, leading to a rejection.
When to Perform Charge Entry in Medical Billing?
Charge entry in medical billing should be performed after the patient visit is completed and the clinical documentation has been finalized by the provider. This step is essential in medical billing because it ensures that all services rendered during the encounter are properly documented and available for accurate claim submission.
Before charge entry begins, the clinical documentation must be complete and verified. This includes provider notes, procedure details, diagnosis information, and any supporting documentation such as referrals or authorizations. Accurate documentation is essential because it serves as the foundation for assigning the correct diagnosis and procedure codes.
Charge entry also depends on the confirmation of appropriate diagnosis (ICD) and procedure (CPT or HCPCS) codes. Coders review the clinical records and finalize the codes that represent the services provided. Once these codes are confirmed, the billing team can enter the corresponding charges into the system and prepare the claim for submission.
What is the Difference Between Charge Entry and Charge Capture?
The main difference between charge entry and charge capture is that charge capture records services performed, while charge entry enters those services into the billing system for claim preparation.
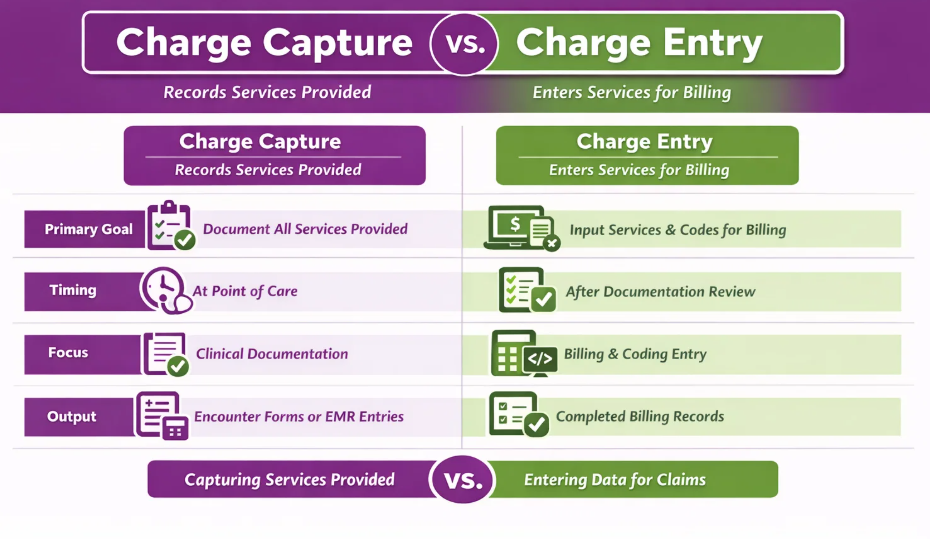
Primary Goal
The primary goal of charge capture is to ensure that every service, procedure, or supply provided during a patient encounter is recorded. The primary goal of charge entry is to accurately input those recorded services, along with the appropriate codes and charges, into the billing system for claim generation.
Timing
Charge capture occurs at the point of care or immediately after the patient encounter when providers document the services they performed. Charge entry occurs later in the billing workflow after documentation and coding are reviewed and finalized.
Focus
The focus of charge capture is clinical documentation and recording billable activities performed during patient care. In contrast, charge entry focuses on translating that documentation into structured billing data within the practice management or billing system.
Output
The output of charge capture is a record of billable services, often in the form of encounter forms, superbills, or EMR entries. The output of charge entry is a completed billing record with assigned codes and charges, which is then used to generate and submit claims to insurance payers.
What is the Difference Between Charge Entry and Payment Posting?
The main difference between charge entry and payment posting is that charge entry records services and charges before claims are submitted. On the other hand, payment posting records the payments received after the payer processes the claim.
Charge entry occurs during the billing phase of the revenue cycle. In this stage, patient services, diagnosis codes, procedure codes, and related charges are entered into the billing system to prepare the claim. In contrast, payment posting takes place during the collections phase, when payments from insurance payers and patients are received and recorded in the system.
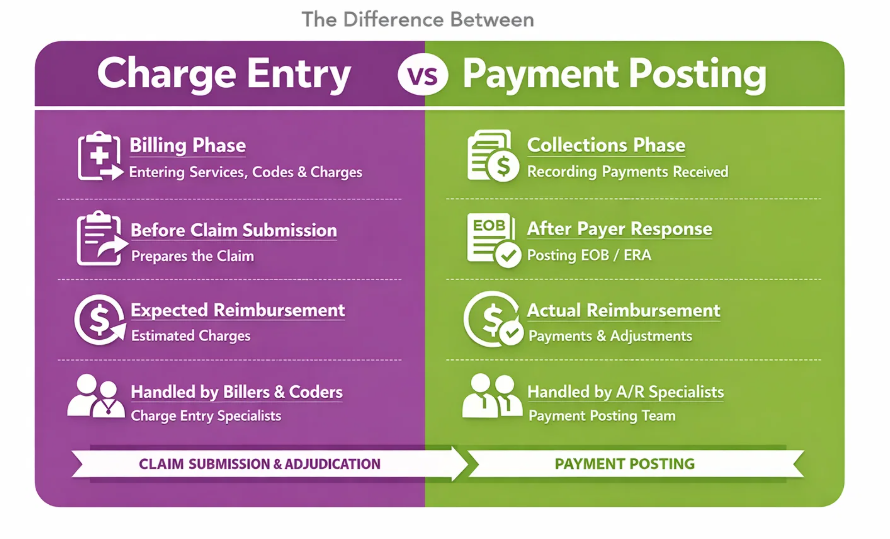
In the sequential workflow of medical billing, charge entry comes first, followed by claim submission, payer adjudication, and then payment posting. This sequence helps clarify where each function fits within the overall revenue cycle process.
Different teams typically handle these responsibilities. Charge entry specialists or medical billers manage the recording of charges and coding data. Payment posting teams or accounts receivable specialists handle the recording of payments, adjustments, and reconciliation with payer remittance advice.
Another key difference is timing. Charge entry happens before claim submission, ensuring all billable services are properly recorded. Payment posting occurs after the payer responds to the claim, based on the Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA).
Finally, charge entry reflects the expected reimbursement based on the services billed. However, payment posting records the actual amount received from the payer and identifies any adjustments, denials, or patient responsibility.







