Revenue Cycle Management (RCM) in medical billing helps healthcare providers manage the financial lifecycle of patient care. It integrates key processes such as patient registration, insurance verification, medical coding, claim submission, payment posting, and denial management to ensure accurate billing and timely revenue collection. The main steps involve pre-registration and scheduling, charge capture and coding, claim submission and payment posting, and denial management.
Effective RCM provides several benefits, including faster cash flow, reduced claim denials, enhanced revenue collection, and improved patient experience. Common mistakes in RCM include inaccurate patient information, skipping insurance verification, poor documentation practices, and inefficient payment posting. This guide will cover what RCM is, its workflow, the advantages it offers, common mistakes to avoid, and strategies for optimizing and evaluating RCM performance in medical billing.
Table of Contents
ToggleWhat is RCM in Medical Billing?
Revenue Cycle Management (RCM) in medical billing is the end-to-end process healthcare providers use to track patient revenue from the moment an appointment is scheduled until the final payment is received. It includes every administrative and financial step involved in getting accurate reimbursement, including patient registration, insurance verification, medical coding, claim submission, payment posting, and denial management.
RCM is not limited to billing alone. It also includes coding, collections, and compliance, all of which work together to keep financial operations accurate and aligned with healthcare regulations. When these functions are managed properly, providers can reduce errors, avoid claim rejections, and maintain a healthier revenue flow.
How the RCM Workflow Works?
The RCM process begins with patient registration, where accurate demographic and insurance information is collected. This step is important because even small errors in patient details can lead to claim delays or denials later in the process.
Next comes insurance verification, where the provider confirms the patient’s coverage, eligibility, benefits, and any prior authorization requirements. This step helps prevent unpaid claims and unexpected patient balances.
After the patient receives care, the clinical documentation is translated into medical codes. These codes represent diagnoses, procedures, and services provided during the visit. Accurate coding is essential because it directly affects how much the provider will be reimbursed. Incorrect coding can trigger denials, underpayments, or compliance issues.
Once coding is complete, the claim is prepared and sent through claim submission to the insurance company. Clean and complete claims improve the chances of fast reimbursement, while incomplete claims often get rejected or delayed.
When payment is received, it is recorded through payment posting. This step helps providers match payments against submitted claims and identify any balance still owed by the insurer or patient.
If a claim is rejected or denied, denial management begins. This involves reviewing the reason for denial, correcting errors, resubmitting claims, and appealing when necessary. Effective denial management helps recover revenue that might otherwise be lost.
Why RCM Matters in Medical Billing?
Effective RCM supports the financial stability of healthcare providers by minimizing claim denials, improving reimbursement accuracy, and helping maintain predictable cash flow. When the RCM workflow is efficient, providers get paid faster and with fewer interruptions, which strengthens overall business performance.
RCM also plays a major role in compliance. Since billing and coding must follow payer rules and healthcare regulations, a strong RCM process helps reduce the risk of audits, penalties, and financial losses.
RCM and EHR/EMR Integration
Modern RCM systems are usually connected with EHR and EMR software, which makes daily work much easier. When a patient’s information is entered in the EHR, it can automatically flow into the billing system, so there’s no need to enter the same data again.
This means details like patient demographics, insurance info, diagnoses, and procedures can be transferred directly from clinical records to claims. It reduces the chances of typing mistakes and missing information, which are common reasons for claim denials.
Who Is Involved in the RCM Process?
RCM involves three main parties: patients, providers, and insurers. Providers deliver the service and document it properly. Patients supply demographic and insurance information and are responsible for any remaining balance. Insurers review claims, determine coverage, and issue reimbursement according to policy terms.
What are the Steps of RCM in Medical Billing?
The steps of RCM in medical billing are the process healthcare providers follow to move from patient scheduling to final payment collection. Each step helps make sure services are documented correctly, claims are submitted properly, and payments are collected on time.
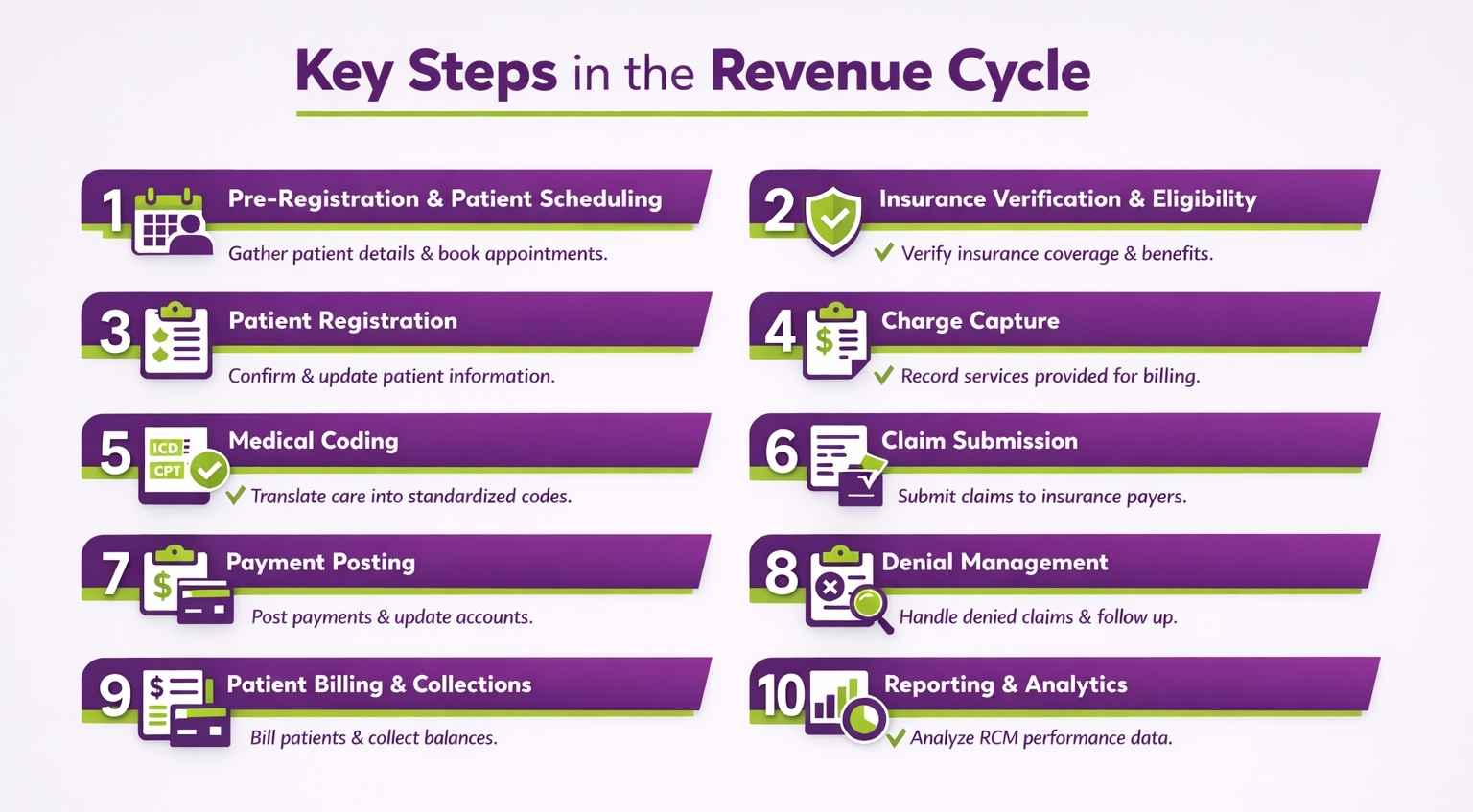
1. Pre-Registration and Patient Scheduling
Pre-registration and patient scheduling are the first steps in the revenue cycle. In this stage, the provider contacts the patient, gathers basic details, and books the appointment. This step includes collecting the patient’s name, contact information, reason for visit, and preliminary insurance details. It helps the office prepare in advance, assign the right appointment slot, and reduce waiting time at check-in.
2. Insurance Verification and Eligibility
Once the patient is scheduled, the provider must verify insurance coverage. This means checking whether the patient’s insurance is active and what services are covered before treatment is given. Verifying insurance coverage helps the billing team find out if prior authorization is needed or if certain services have coverage limits. It also allows the provider to follow payer rules correctly and avoid denied claims later.
3. Patient Registration
At registration (on the day of service), staff confirm and update the patient’s information in the system. This usually includes demographics, insurance details, address, phone number, and other billing-related information. This step also involves creating a new patient file or updating an existing one. Patients may also complete consent forms and HIPAA-related documents during registration.
4. Charge Capture
Charge capture is the step where every service, treatment, test, and procedure provided to the patient is recorded for billing purposes. This includes the doctor’s documentation, medications, diagnostic tests, procedures, and supplies used during the visit.
If anything is missed here, the provider may lose revenue. In fact, research shows hospitals can lose 3–5% of revenue to missed charges. Charge capture can be done manually or through EHR systems. When documentation is complete, it becomes much easier to move into coding and claim submission.
5. Medical Coding
Medical coding is the process of converting clinical documentation into standardized codes. These usually include ICD codes for diagnoses, CPT codes for procedures, and HCPCS codes for supplies and other services.
The coder reviews the provider’s notes and assigns the correct codes based on the care given to the patient. These codes decide how the claim will be processed and how much reimbursement the provider may receive.
6. Claim Submission
After coding, the provider creates and submits insurance claims. At this stage, all coded information is put together and sent to the insurance company electronically or via paper to get payment. Before submission, the claim is usually checked for missing details, coding errors, or format issues through a process called claim scrubbing.
7. Payment Posting
When insurers process a claim, they issue a payment (or denial) with an Explanation of Benefits (EOB). Payment posting is the process of applying those payments to the correct patient accounts. The billing team posts insurer payments daily and flags any underpayments or adjustments. This step keeps the accounts updated and helps the provider track what has been paid and what is still pending.
8. Denial Management and Follow-Up
Managing denied or underpaid claims is the next step. Denial management and follow-up involve reviewing claims that were denied or rejected by the insurer and taking action to fix them. The billing team checks the reason for denial, such as missing information, coding mistakes, eligibility issues, or lack of prior authorization. Then the claim is corrected, resubmitted, or appealed if needed.
9. Patient Billing and Collections
After insurance pays, any remaining balance is billed to the patient. This includes copayments or services not covered by insurance. Clear patient communication and billing statements at this stage improve collection rates. The RCM process at this point focuses on collecting patient payments and setting up payment plans as needed.
10. Reporting and Analytics
Reporting and analytics are the final step in the revenue cycle, where billing data is reviewed to measure performance. This includes tracking denial rates, collection rates, accounts receivable days, and other important billing numbers. These reports show how well the RCM process is working. By studying this data, healthcare providers can spot problems and make better decisions for future revenue management.
What are the Benefits of RCM in Medical Billing?
Implementing strong RCM practices brings a lot of benefits. An optimized revenue cycle improves cash flow, reduces claim denials, boosts collections, improves patient satisfaction, and increases efficiency. Specifically:

Improves Cash Flow
A well-managed RCM process helps providers submit claims quickly and correctly, which leads to faster payments from insurance companies. It also helps catch issues early, like missing details, incorrect information, or eligibility problems. Fixing these before submission prevents unnecessary delay in reimbursements.
With fewer errors and quicker processing, payments are received on time, which keeps cash flow steady. This consistency makes it easier for healthcare providers to manage daily expenses and plan financially without uncertainty.
Reduces Claim Denials
A strong RCM process helps reduce claim denials by ensuring accurate coding and properly formatted claims before submission. When claims are clean and complete, the chances of rejection from insurance companies are much lower.
It also includes verifying patient eligibility and coverage in advance, so claims are only submitted for services that are actually covered. This prevents avoidable denials and saves time for the billing team.
Enhances Revenue Collection
Thorough RCM ensures that all services provided are properly documented and coded, so nothing is missed during billing. This prevents revenue leakage and makes sure the provider is paid for every service delivered.
It also involves regular follow-up on unpaid insurance claims and patient balances. By staying on top of pending payments, providers can recover dues faster and reduce accounts receivable.
Improves Patient Experience
RCM helps create clear and easy-to-understand billing statements, so patients can see exactly what they’ve been charged, what has been paid, and what balance is left. This reduces confusion and makes the process more transparent.
It also improves communication around copayments and insurance coverage. When patients know what to expect financially, they feel more confident and less stressed about billing. Efficient front-end processes, like smooth registration and quicker billing, also reduce wait times and make interactions easier for patients.
Increases Operational Efficiency
RCM connects all key steps, like registration, coding, billing, and collections, into one smooth workflow. This coordination between departments reduces confusion and keeps the process moving without unnecessary delays. With automation and standardized procedures, there’s less manual work and fewer chances of human error.
When routine tasks are handled efficiently, staff can focus more on important work instead of fixing mistakes or chasing missing information. The use of EHR systems and billing software also helps data move easily from one step to another, speeding up the entire process and making operations more organized.
Ensures Regulatory Compliance
A strong RCM process ensures that coding is accurate and documentation is complete, so claims are submitted according to legal requirements and payer guidelines. This reduces the risk of errors that could lead to compliance issues.
By following proper regulations, healthcare providers are less likely to face audits, penalties, or legal complications. It keeps billing practices aligned with industry standards. RCM also supports adherence to HIPAA and payer-specific rules, which helps protect patient data and maintain privacy.
Improves Financial Visibility
RCM systems give a clear view of revenue, pending claims, and patient balances. This makes it easier for healthcare providers to track where money is coming from and what is still outstanding. With access to accurate reports and analytics, providers can make better decisions about budgeting, staffing, and improving operations.
It helps them understand the financial health of their practice at any time. These insights also highlight delays or problem areas in billing, claims, or collections, so issues can be fixed quickly before they impact revenue.
Accelerates Payment Cycles
An efficient RCM process helps claims get submitted quickly and without errors, which speeds up how fast insurance companies process and reimburse them. It also includes timely payment posting and regular follow-up on unpaid claims.
This ensures that any pending balances, whether from insurers or patients, are collected without unnecessary delays. With smoother workflows and fewer bottlenecks, claims don’t stay unpaid for long. This improves cash flow and keeps the overall financial performance of the practice stable.
Supports Scalability for Healthcare Practices
A well-structured RCM process allows healthcare providers to handle more patients without needing to increase administrative staff. Standardized processes also make it simpler for practices to grow across multiple locations.
Whether it’s billing, coding, or collections, having the same system in place helps maintain consistency and control. As a result, providers can expand their services while still keeping billing operations accurate, organized, and easy to manage.
Strengthens Denial Management
A strong RCM process helps quickly identify denied or rejected claims and understand the reason behind them. This allows billing teams to fix errors and resubmit claims without wasting time. With a proper system in place, denials are tracked and handled efficiently, so nothing gets missed or left unresolved.
By addressing denials promptly, healthcare providers can recover revenue that might otherwise be lost and improve overall collection rates.
What are the RCM Mistakes in Medical Billing?
RCM mistakes in medical billing can disturb cash flow, delay reimbursements, and increase claim denials. Common mistakes include inaccurate patient information, skipping insurance verification, poor documentation practices, incorrect medical coding, delayed charge entry, incomplete claim submission, ignoring claim denials, lack of follow-up, inefficient payment posting, and reporting.
Inaccurate Patient Information
Inaccurate patient details, such as misspelled names, incorrect birthdates, or wrong insurance IDs, are a common cause of billing errors and claim rejections. Even small demographic mismatches can derail claim adjudication, and reports estimate that a noticeable portion of denials stem from incorrect patient information.
Skipping Insurance Verification
Failing to verify a patient’s insurance coverage and benefits before services are provided often leads to claims for non‑covered procedures. This not only increases denial rates but also raises administrative burden due to unprocessed or returned claims. In this case, early eligibility checks help reduce these denials.
Poor Documentation Practices
Incomplete or unclear medical records make coding difficult and can make claims invalid. Missing physician signatures, missing patient consent forms, or absent clinical details are frequent documentation issues that lead to denials because the claim lacks necessary supporting evidence.
Incorrect Medical Coding
Assigning incorrect diagnostic (ICD) or procedural (CPT/HCPCS) codes remains one of the most common billing mistakes. Coding mistakes can lead to denial or underpayment. According to MGMA, coding errors account for approximately 25–30% of all claim denials in U.S. healthcare practice.
Delayed Charge Entry
Failing to promptly record services, procedures, and supplies delays the entire billing workflow. Charges that are entered late push back claim submission, which slows reimbursements and creates a backlog in accounts receivable.
Late or Incomplete Claim Submission
Claims submitted past payer deadlines or with missing required data often fail to be processed. Late filing can result in not just delay but permanent revenue loss, as many insurers enforce strict, timely filing limits. For example, if an insurer enforces a 90-day timely filing limit, submitting a claim after 100 days will result in automatic denial.
Ignoring Claim Denials
Not addressing denied claims prevents correction and resubmission, which leads to avoidable revenue loss. According to RevCycle Intelligence, practices can lose up to 3–5% of annual revenue due to unaddressed claim denials.
Lack of Follow-Up on Claims
Without prompt follow‑up with insurers or patients, claims can remain unresolved, and outstanding balances accumulate. An Experian Health survey found that about 41% of providers report denial rates above 10%, and in 65% of denied cases, practices never resubmit the claim. This shows that not following up significantly impacts revenue recovery.
Inefficient Payment Posting
Mistakes or delays in posting received payments can create discrepancies between the amounts billed and the actual collections, which makes it difficult to track revenue accurately. This shows that inefficient payment posting can lead to financial mismanagement, delayed reporting, and challenges in identifying outstanding balances.
Lack of Reporting and Analytics
Not monitoring key performance indicators (KPIs) and financial metrics prevents healthcare organizations from truly understanding how well their revenue cycle is performing. Without tracking data like denial rates, clean claim rates, and accounts receivable aging, problems can go unnoticed until they impact cash flow and operational efficiency.
How to Choose the Right RCM Company in Medical Billing?
To choose the right RCM company for medical billing, evaluate your practice’s specific needs, the company’s capabilities, and how well their services align with your financial goals. Here are the key steps to guide your selection:
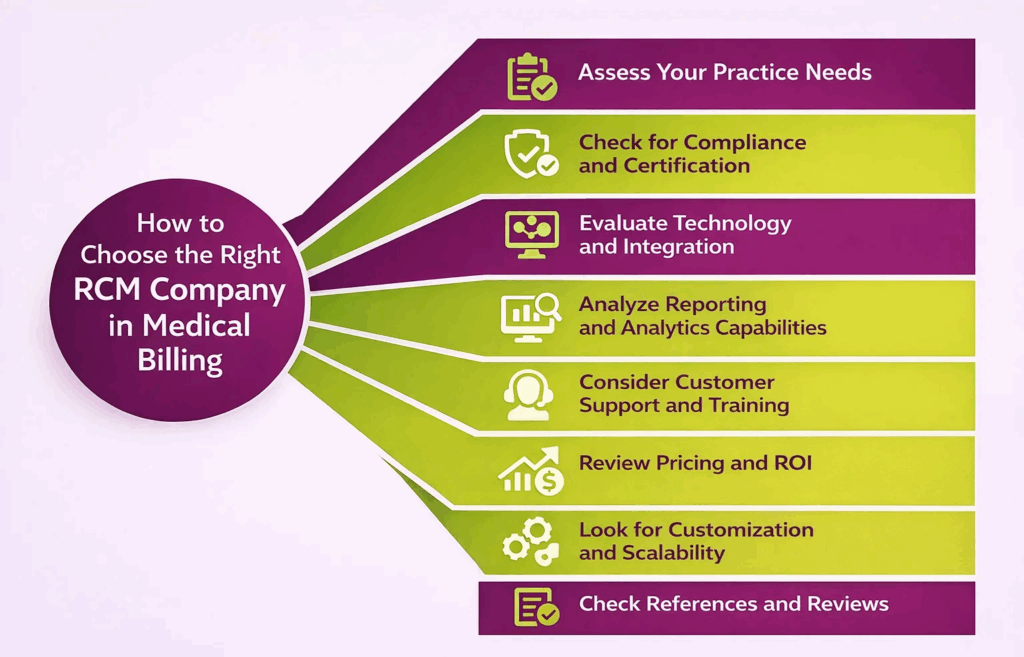
- Assess Your Practice Needs: Identify your practice size, specialties, patient volume, and specific billing challenges to determine what RCM services you require.
- Check for Compliance and Certification: Ensure the company adheres to HIPAA regulations and holds certifications like AAPC or AHIMA to guarantee proper handling of sensitive patient data.
- Evaluate Technology and Integration: Confirm that their software integrates with your existing EHR/EMR systems and supports automation to improve workflow efficiency.
- Analyze Reporting and Analytics Capabilities: Look for reporting tools that provide insights into claim performance, denial rates, and revenue trends to support data-driven decisions.
- Consider Customer Support and Training: Assess the company’s training programs, ongoing support, and responsiveness to ensure smooth onboarding and continuous assistance.
- Review Pricing and ROI: Compare pricing structures, including setup fees, monthly costs, and transaction-based charges, and evaluate the potential return on investment.
- Look for Customization and Scalability: Choose a provider that can tailor services to your practice’s workflow and scale as your patient base or locations grow.
- Check References and Reviews: Speak with current clients and read independent reviews to check reliability, performance, and client satisfaction.
How to Optimize RCM in Medical Billing?
To optimize RCM in medical billing, healthcare practices should focus on improving efficiency in how medical billing works. Here are the key steps:
- Enhance Patient Registration & Eligibility Verification: Ensure accurate collection of patient demographics, insurance information, and coverage details upfront to prevent claim denials and delays.
- Improve Charge Capture & Coding Accuracy: Record all services and procedures promptly and assign correct ICD, CPT, and HCPCS codes to maximize reimbursement and reduce errors.
- Streamline Claims Submission: Submit claims quickly with complete and accurate data, and utilize automation tools to reduce manual errors and delays.
- Implement Denial Management Strategies: Track denied or rejected claims, identify common causes, and resubmit corrected claims promptly to recover lost revenue.
- Optimize Payment Posting & Reconciliation: Accurately post payments, reconcile accounts, and identify discrepancies between billed amounts and collections to maintain financial accuracy.
- Leverage Reporting & Analytics: Use dashboards and KPIs to monitor revenue trends, claim performance, and denial rates to enable data-driven decision-making.
- Invest in Staff Training & Technology: Provide ongoing training on coding, billing regulations, and software tools while adopting advanced RCM technology for better efficiency and scalability.
Is RCM for Payers or Providers?
RCM (Revenue Cycle Management) is primarily for healthcare providers, not payers. It manages the financial processes of hospitals, clinics, and physician practices, from patient registration and insurance verification to coding, billing, claim submission, payment posting, and denial management.
How to Evaluate the Performance of Your RCM in Medical Billing?
To evaluate the performance of your RCM in medical billing, you need to measure how efficiently claims are processed, payments are collected, and resources are managed. The following steps help you pinpoint strengths and weaknesses in your revenue cycle:
- Monitor Key Performance Indicators (KPIs): Track performance metrics such as days in accounts receivable (A/R), clean claim rate, denial rate, and net collection rate. For example, many industry experts recommend a clean claim rate above 95% as a sign of strong RCM performance because higher clean claim rates correlate with faster payments.
- Track Claim Submission Timeliness: Review how quickly claims are submitted after services are provided. Claims submitted within payer filing limits have a much higher chance of being processed. For instance, claims filed before the 30‑ to 90‑day deadline set by most insurers are significantly less likely to be denied due to late filing.
- Analyze Denial and Rejection Trends: Look for patterns in why claims are denied, whether due to coding errors, missing information, or eligibility issues. Industry data shows that up to 60% of denials are avoidable if root causes are identified and corrected.
- Assess Payment Posting Accuracy: Ensure that payments received from insurers and patients are posted correctly and without delay. Inaccurate payment posting can lead to discrepancies between expected and actual revenue.
- Review Revenue Cycle Efficiency: Evaluate the time it takes for a claim to move through the entire cycle, from registration to final payment. A common benchmark is maintaining accounts receivable days under 40–45 days.
- Evaluate Reporting and Analytics Use: Confirm that your RCM platform provides meaningful reports and dashboards. Analytics that show trends in denials, outstanding claims, and payer performance help identify problem areas. Practices using advanced analytics often see improved collections because they can act on data, not guesswork.
- Solicit Feedback from Staff and Providers: Ask front‑end staff, billers, and providers where bottlenecks occur or what challenges they face. Those closest to daily operations often spot issues not visible in reports, such as recurring patient registration errors that lead to claim problems.
- Compare Against Industry Benchmarks: Compare your RCM performance to national or specialty‑specific benchmarks. For example, if your denial rate is significantly higher than the industry average (often reported between 5–12% on first submission), this indicates a need for process improvement.







