HCPCS codes are standardized codes used in healthcare billing to report medical services, procedures, equipment, and supplies. They support accurate claim submission and ensure providers receive proper reimbursement from payers.
There are two main levels of HCPCS codes. Level I includes CPT codes, which cover physician services and procedures. Level II includes alphanumeric codes used for non-physician services such as durable medical equipment, ambulance services, prosthetics, and certain drugs.
HCPCS codes offer several key benefits. They improve billing accuracy, reduce claim denials, standardize communication between providers and payers, and support compliance with healthcare regulations. These codes also help streamline reimbursement workflows and reporting.
In practice, HCPCS codes are used across hospitals, physician offices, ambulatory surgical centers, and other healthcare settings. They are essential for documenting services, submitting insurance claims, and ensuring consistent coding across the healthcare system.

Table of Contents
ToggleWhat are HCPCS Codes?
HCPCS codes are standardized billing codes used to report medical services, supplies, and procedures for reimbursement. Their correct use depends heavily on clear and complete medical documentation.
Accurate coding requires detailed records such as operative notes, patient charts, encounter notes, and imaging reports. These documents must clearly support the services performed and explain the clinical need behind them. Documentation must also directly match the assigned CPT or HCPCS codes. Every billed service should be backed by clear clinical evidence to avoid errors, delays, or claim denials.
Modifiers add another layer of specificity, and they require explicit justification in the documentation. For example, modifier 59 (distinct procedural service) must show that procedures were separate and independent. Modifier 25 (separately identifiable E/M service) requires proof that the evaluation and management service was significant and separate from other services performed the same day.
What are the Levels of HCPCS Codes?
HCPCS codes are divided into two main levels that categorize medical services, procedures, and supplies for billing and reimbursement purposes. Each level serves a distinct function in the healthcare coding system.
1. Level 1
Level I HCPCS codes are used to report physician services, medical procedures, and diagnostic services.
2. Level 2
Level II HCPCS codes are used to report non-physician services and items, such as durable medical equipment, ambulance services, medical supplies, and certain drugs.
Level 1
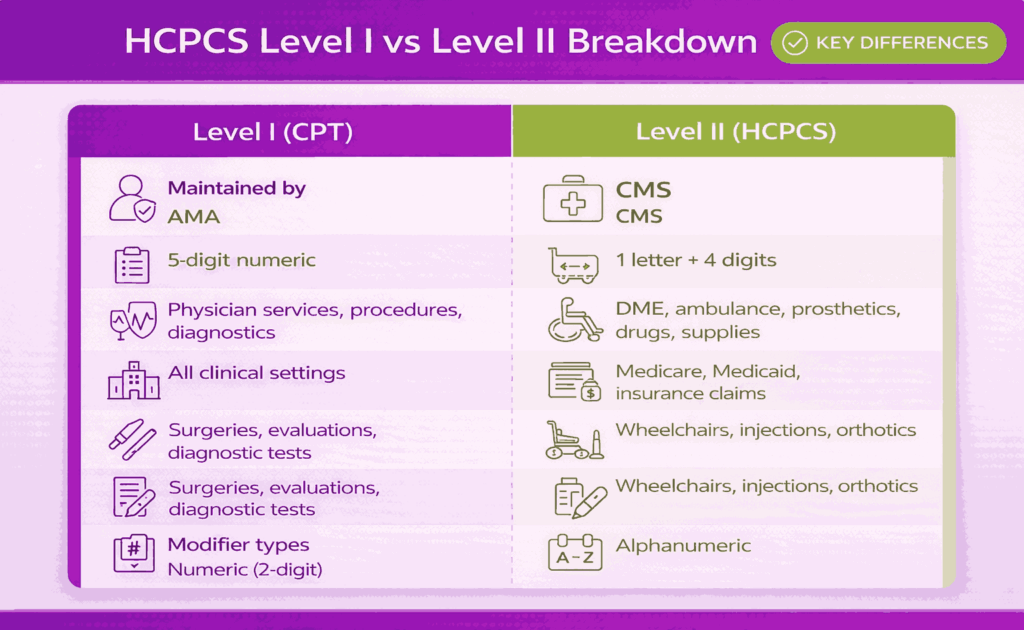
HCPCS Level I codes correspond directly to CPT (Current Procedural Terminology) codes. These codes are used to report medical procedures and services performed by healthcare providers in clinical settings.
They cover a wide range of clinical services, including patient examinations, diagnostic procedures, surgical treatments, and other medical interventions performed by physicians and qualified healthcare professionals.
Level I HCPCS codes play a key role in physician billing by standardizing how clinical services are documented and submitted to insurance payers. This ensures consistency, accuracy, and proper reimbursement across healthcare systems. These codes primarily apply to services delivered directly by healthcare professionals, such as diagnostic tests, surgeries, consultations, and other in-person or procedural care activities.
Level 2
HCPCS Level II codes are used to report non-physician services, medical supplies, medications, and equipment that are not covered under CPT codes. They fill the gap for items and services outside standard physician procedures.
These codes commonly include durable medical equipment (DME), prosthetics, orthotics, ambulance services, and certain drugs administered outside typical clinical procedures. They are essential for billing a wide range of non-clinical healthcare items.
The key difference is that Level I HCPCS codes represent physician services and medical procedures, while Level II codes focus on products, supplies, and non-physician services not included in CPT.
Level II codes follow an alphanumeric format, typically starting with a letter followed by four numbers. This structure helps organize and categorize different types of medical goods and services for consistent billing and reimbursement.
What are the Benefits of HCPCS Codes?
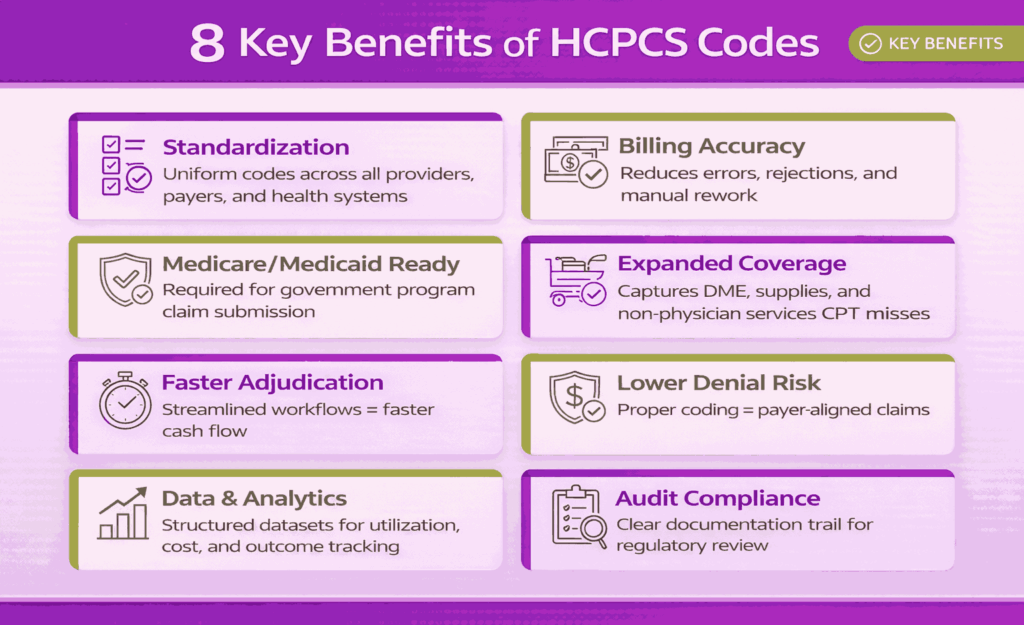
HCPCS codes provide a standardized system for reporting medical services, supplies, and equipment across the healthcare industry. This standardization ensures consistent communication between providers, payers, and regulatory bodies.
They improve billing accuracy by clearly defining each service or item, which helps reduce errors and supports proper reimbursement. HCPCS codes are also essential for Medicare and Medicaid claims processing, ensuring that services meet payer requirements.
These codes expand billing capabilities by covering non-physician services, including medical supplies, equipment, and drugs that are not included in CPT codes. This allows providers to capture the full scope of care delivered.
HCPCS codes enhance efficiency in claim processing by streamlining workflows and reducing manual corrections. They also lower the risk of claim denials by ensuring that services are properly coded and supported.
In addition, HCPCS codes strengthen data tracking and reporting by enabling consistent data collection across healthcare systems. They support compliance and auditing processes by providing clear, standardized documentation for regulatory review.
Ensuring Standardization Across Healthcare Systems
Standardized coding systems ensure that all healthcare providers and insurance companies use the same set of codes, which promotes consistency in billing and reimbursement across the industry.
This standardization also supports seamless data exchange between hospitals, clinics, insurers, and other healthcare systems. It improves coordination, reduces miscommunication, and helps ensure that services are accurately recorded and processed across different platforms.
Improving Accuracy in Billing and Reimbursement
Accurate coding and proper documentation reduce errors in claim submission, which lowers the chances of claim rejections and minimizes administrative rework.
Clear and precise coding ensures that each medical service or procedure is correctly identified. This allows payers to understand exactly what care was provided, supporting faster processing and appropriate reimbursement.
Supporting Medicare and Medicaid Claims Processing
HCPCS codes are widely used in government programs to standardize billing for medical services, supplies, and procedures. This ensures consistency across providers and aligns claims with federal requirements.
They are required for submitting Medicare and Medicaid claims, helping these programs accurately track services and determine appropriate reimbursement. This standardization supports efficient processing and reduces errors in government-funded healthcare billing.
Expanding Coverage for Non-Physician Services
HCPCS Level II codes cover services and items that are not performed by physicians, such as durable medical equipment (DME), ambulance services, prosthetics, orthotics, and medical supplies.
These codes expand the range of billable healthcare services by ensuring that non-physician services are properly documented and reimbursed. This helps providers capture the full scope of care delivered and improves overall coverage within healthcare systems.
Enhancing Efficiency in Claim Processing
Efficient coding and standardized processes allow faster claim submission and adjudication, reducing delays in reimbursement and improving overall cash flow for healthcare providers.
Modern billing systems also use automation tools and electronic workflows to streamline claim handling. These systems improve accuracy, reduce manual errors, and enhance the overall speed and efficiency of the billing process.
Reducing the Risk of Claim Denials
Accurate use of HCPCS codes ensures that claims are correctly interpreted by payers, reducing the likelihood of rejections caused by errors, missing details, or inconsistencies.
Proper coding also ensures alignment with payer-specific rules and guidelines. This helps providers meet regulatory requirements, avoid compliance issues, and reduce the risk of audits or financial penalties.
Strengthening Data Tracking and Reporting
HCPCS and related coding systems generate structured data that supports healthcare analytics. This data helps organizations evaluate trends, costs, and patient outcomes to improve decision-making.
These codes also allow tracking of how frequently specific services, procedures, or supplies are used. This provides clear insight into patient care patterns and supports better resource allocation across healthcare systems.
Facilitating Compliance and Auditing Processes
Standardized coding and documentation help healthcare providers comply with regulatory requirements and payer guidelines. This reduces the risk of violations, penalties, and reimbursement issues.
Consistent and accurate records also make audits easier. Auditors can quickly review claims and verify services, which improves transparency and speeds up the audit process.
Using uniform coding practices ensures consistency across providers and systems. This improves clarity in communication, strengthens data integrity, and supports more reliable healthcare reporting.
How are HCPCS Codes used in Medical Billing?
HCPCS codes are used throughout the medical billing process to standardize how services, supplies, and procedures are documented, submitted, and reimbursed. They ensure that each element of patient care is clearly identified and consistently communicated to payers.
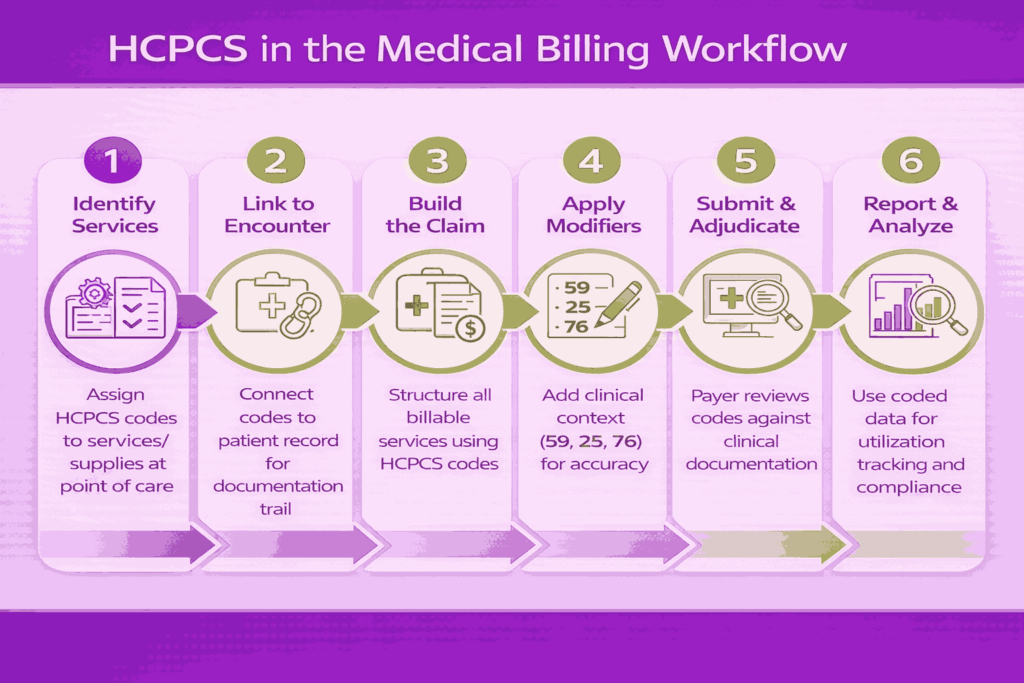
These codes are used to identify services and supplies provided during patient care, linking them directly to specific patient encounters in medical records. This ensures that every billed item is traceable to clinical documentation.
HCPCS codes are then used in claim creation and submission, where they form the core structure of billing claims sent to insurance payers. They help determine reimbursement by defining what services are covered and how payment is calculated.
Modifiers are applied alongside HCPCS codes to provide additional detail about how and why a service was performed. This improves accuracy and ensures correct payment based on the clinical scenario.
They also support compliance with coding guidelines, helping providers follow payer and regulatory requirements. During claim review and adjudication, HCPCS codes allow payers to verify services and process claims efficiently.
Finally, HCPCS codes enable reporting and data analysis by creating standardized datasets that can be used to evaluate utilization, costs, and healthcare outcomes.
Identifying Services and Supplies with HCPCS Codes
HCPCS codes assign standardized identifiers to medical procedures, supplies, and equipment. This ensures that each service or item provided in patient care is clearly documented and correctly billed.
These standardized codes help eliminate confusion by ensuring that every billed service or supply is consistently recognized by payers and healthcare systems.
Linking HCPCS Codes to Patient Encounters
HCPCS codes connect each patient encounter with the specific services, procedures, or supplies provided. This ensures accurate documentation of care and supports correct billing for every visit.
Consistent use of these codes also helps track a patient’s treatment history over time. This supports continuity of care and allows providers to review past services, treatments, and outcomes when making clinical decisions.
Using HCPCS Codes in Claim Creation and Submission
HCPCS codes structure and organize all billable services, supplies, and procedures within a claim. This ensures every component of patient care is properly represented before submission.
Using correct HCPCS codes helps ensure claims meet payer requirements and are complete. This improves the chances of timely approval and faster reimbursement.
Accurate coding also reduces common billing errors such as incorrect code selection, missing information, or mismatched services. This minimizes claim rejections, delays, and the need for resubmission.
Determining Reimbursement Through HCPCS Codes
HCPCS codes are used by payers to assign specific reimbursement values to each service, supply, or procedure. These codes form the foundation for calculating payment amounts in medical billing.
Reimbursement is typically based on payer-specific fee schedules and contractual agreements. As a result, the same HCPCS code may have different payment rates depending on the insurance provider or healthcare program.
Applying Modifiers with HCPCS Codes for Accuracy
Modifiers are used to indicate special or unique conditions under which a service was performed, such as altered procedures, multiple services, or specific clinical circumstances.
They provide additional context about how, when, or where a procedure was performed. This helps payers clearly understand the claim details and process them accurately, reducing errors in reimbursement decisions.
Ensuring Compliance with HCPCS Coding Guidelines
Compliance requires following the coding guidelines set by CMS and individual payers. This ensures that all claims meet regulatory and reimbursement requirements.
Proper compliance practices reduce billing errors and help prevent fraudulent claims. This protects healthcare providers from audits, penalties, and legal or financial consequences.
Facilitating Claim Review and Adjudication Using HCPCS Codes
HCPCS codes provide standardized identifiers for services, supplies, and procedures. This helps reviewers verify that billed services match the supporting clinical documentation.
These codes also allow insurance payers to evaluate and process claims consistently. This ensures reimbursement decisions are based on accurate, standardized, and reliable coding across all claims.
Enabling Reporting and Data Analysis with HCPCS Codes
HCPCS codes allow healthcare organizations to systematically collect and organize data from patient services. This ensures accurate and consistent reporting across providers, facilities, and healthcare systems.
The data generated through HCPCS coding can be aggregated and analyzed to support decision-making, resource allocation, and long-term strategic planning. This improves operational efficiency and helps enhance overall healthcare outcomes.
Who Maintains and Updates HCPCS Codes?
HCPCS is maintained through a structured governance system designed to ensure consistent and standardized medical coding across the U.S. healthcare system. This system defines how codes are created, updated, and reviewed.
The Centers for Medicare & Medicaid Services (CMS) is the primary authority responsible for HCPCS Level II codes. CMS oversees their development, maintenance, and updates to ensure they reflect current billing needs for non-physician services, supplies, and equipment.
HCPCS Level I codes correspond to CPT codes, which are maintained by the American Medical Association (AMA). The AMA ensures these codes remain standardized for physician services and clinical procedures.
HCPCS codes are reviewed and updated annually. This process includes adding new codes, revising existing ones, and removing outdated codes to reflect changes in medical practice, technology, and healthcare delivery.
Governance also involves collaboration between federal agencies, healthcare providers, and industry stakeholders. This ensures the coding system remains accurate, consistent, and relevant to real-world clinical and billing needs.
What is the Difference Between CPT and HCPCS?
CPT codes represent Level I of the HCPCS system, while HCPCS also includes Level II codes. Together, they form a complete coding framework used for healthcare billing and reimbursement.
CPT codes are used to report medical procedures and physician services such as evaluations, surgeries, and diagnostic tests. HCPCS Level II codes cover non-physician services, including durable medical equipment (DME), medical supplies, prosthetics, and ambulance services.
CPT codes are numeric and typically consist of five digits. In contrast, HCPCS Level II codes are alphanumeric, made up of one letter followed by four numbers, which helps distinguish them within the coding system.
CPT codes are widely used across all healthcare settings for reporting clinical services. HCPCS Level II codes are primarily required for Medicare and Medicaid billing, as well as other insurance claims involving non-physician services and items.
How Do I Look Up an HCPCS Code?
You can look up an HCPCS code using official resources, coding tools, or billing systems that help match services and supplies to the correct code.
- Use the Official CMS HCPCS Website
Visit the Centers for Medicare & Medicaid Services (CMS) website to access the most updated and official HCPCS code set and annual updates. - Use Online HCPCS Lookup Tools
Use trusted medical coding websites that allow keyword-based searches to quickly find relevant HCPCS codes. - Use a HCPCS Code Book
Refer to printed or digital HCPCS coding manuals that list codes along with detailed descriptions for services, supplies, and equipment. - Use Medical Billing Software / EHR Systems
Electronic Health Records (EHR) and billing software often include built-in code search features that suggest appropriate HCPCS codes based on documentation. - Search by Keywords
Enter relevant terms such as “wheelchair,” “ambulance,” or “injection drug” to identify the most appropriate HCPCS code based on the service or item provided.
How do HCPCS Codes Integrate with Other Medical Coding Systems?
HCPCS codes integrate with other medical coding systems by working alongside diagnosis, procedure, and billing codes to create a complete and accurate claim for reimbursement.
- Understanding the Role of Each Coding System
HCPCS, CPT, and ICD-10 all serve different purposes within Medical Coding Systems. ICD-10 codes define the diagnosis, CPT/HCPCS Level I codes describe procedures, and HCPCS Level II codes cover supplies, drugs, and equipment. - Linking Diagnosis Codes (ICD-10) with Procedure Codes (HCPCS/CPT)
ICD-10 codes are paired with HCPCS/CPT codes to establish medical necessity and justify why a service or procedure was performed. - Using HCPCS Codes for Supplies, Drugs, and Equipment
HCPCS Level II codes fill gaps in coding by covering non-physician items like durable medical equipment and injectable drugs not included in CPT. - Applying Modifiers Across Coding Systems
Modifiers are used with HCPCS and CPT codes to provide additional clinical context, improving claim clarity and accuracy. - Following Payer-Specific Guidelines (CMS Requirements)
Different payers, especially CMS programs, have specific rules within medical coding systems that determine how HCPCS codes must be applied for reimbursement. - Ensuring Coding Consistency and Accuracy
All coding elements must align properly to avoid mismatches between diagnosis, procedure, and supply codes. - Using EHR and Coding Software for Integration
Electronic Health Records and billing tools integrate medical coding systems to streamline code selection and claim creation in a single workflow. - Maintaining Compliance and Proper Documentation
Proper documentation supports all coding systems, ensuring claims meet payer and regulatory requirements. - Conducting Regular Coding Audits
Audits help identify inconsistencies or errors in how HCPCS codes interact with other medical coding systems. - Training Coding Staff on Coding System Integration
Training ensures coders understand how HCPCS fits within broader medical coding systems for accurate billing and compliance.
Are HCPCS Codes only for Medicare?
No, HCPCS codes are not only for Medicare. Although they are essential for Medicare billing, HCPCS codes, especially Level II, are also used by Medicaid and many private insurance companies. They standardize the reporting of medical services, supplies, drugs, and equipment across multiple healthcare payers, not just Medicare.
How Often are HCPCS Codes Updated?
HCPCS codes are updated on a regular schedule to keep the coding system aligned with current medical practice, technology, and billing requirements.
- Quarterly Updates (Most Frequent)
HCPCS Level II codes may receive quarterly updates to add new codes, revise existing ones, or remove outdated entries as needed for ongoing billing accuracy. - Annual Updates (Major Changes)
A major update occurs annually, typically introducing significant additions, deletions, and revisions that reflect changes in healthcare services, supplies, and regulations. - Occasional Monthly / Ad Hoc Updates
In some cases, CMS may release special or temporary updates outside the regular cycle to address urgent billing needs or policy changes.
What is the Difference Between HCPCS and ICD-10?
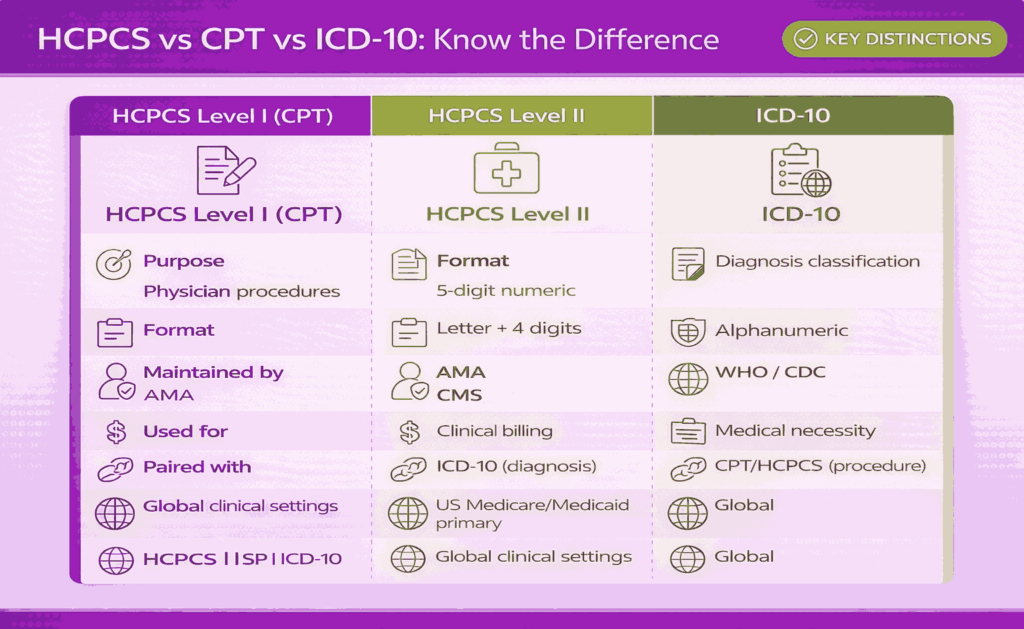
HCPCS and ICD-10 serve different purposes within healthcare billing and Medical Coding Systems. ICD-10 codes describe diagnoses, while HCPCS codes are used to report medical services, supplies, and procedures for billing.
ICD-10 codes identify the patient’s condition or reason for the visit, such as an illness, injury, or symptom. HCPCS codes, on the other hand, describe what was done or provided during care, including procedures, medical equipment, drugs, and supplies.
ICD-10 codes are alphanumeric and used globally for diagnosis classification. HCPCS Level I (CPT) codes are numeric 5-digit codes for procedures, while HCPCS Level II codes are alphanumeric (one letter followed by four digits) used mainly for non-physician services like durable medical equipment and ambulance services.
HCPCS codes are widely used across healthcare settings and are essential for Medicare and Medicaid billing, as well as many private insurance claims. Together with ICD-10, they ensure complete and accurate documentation of both diagnosis and treatment within a unified billing process.
What are HCPCS Modifiers?
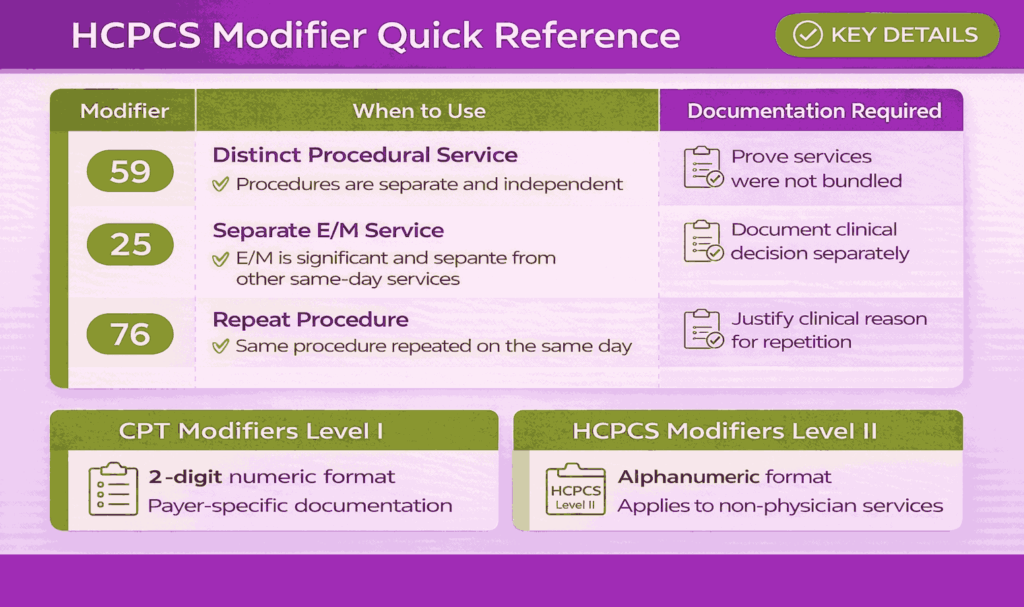
HCPCS modifiers are codes added to HCPCS or CPT codes to clarify how, why, where, or by whom a service was performed without changing the meaning of the original procedure code. They add important context to ensure the claim is accurately interpreted.
Modifiers are categorized within Medical Coding Systems as either CPT (Level I) modifiers, which are typically two-digit numeric codes, or HCPCS Level II modifiers, which are alphanumeric. Both types serve the same purpose of adding detail to a billed service.
In medical billing and claims processing, modifiers help ensure accurate reimbursement by explaining special circumstances such as multiple procedures, altered services, or repeat procedures. This reduces the risk of claim denials and misinterpretation by payers.
They also help meet payer requirements from Medicare, Medicaid, and private insurers. By providing clear supporting details, modifiers strengthen audit trails, improve compliance, and ensure proper documentation integrity.







