Medical coding is a fundamental function in medical billing that translates clinical documentation into standardized codes used for insurance claims and healthcare reporting. It connects patient care services with reimbursement systems by converting diagnoses, procedures, and medical services into universally recognized code formats. Accurate medical coding ensures healthcare providers receive correct payment and maintain compliance with billing regulations.
The most widely used medical coding systems are ICD, CPT, and HCPCS. Medical coding follows a defined process that begins with reviewing medical records, identifying billable services, assigning the correct codes, and verifying code accuracy before claim submission.
Medical coding also follows established rules, including adherence to official coding guidelines, accurate documentation interpretation, and avoidance of unbundling or upcoding. This article explains medical coding in medical billing, the primary coding system used in healthcare, the main steps in the coding process, and the key rules that guide compliant coding practices.
Table of Contents
ToggleWhat is Medical Coding?
Medical coding is the process of converting diagnoses, medical procedures, healthcare services, and medical supplies documented in patient records into standardized alphanumeric codes. These codes represent the clinical information recorded by healthcare providers in a uniform format. Medical coding ensures that medical documentation is translated into a structured coding system that can be consistently interpreted across healthcare organizations.
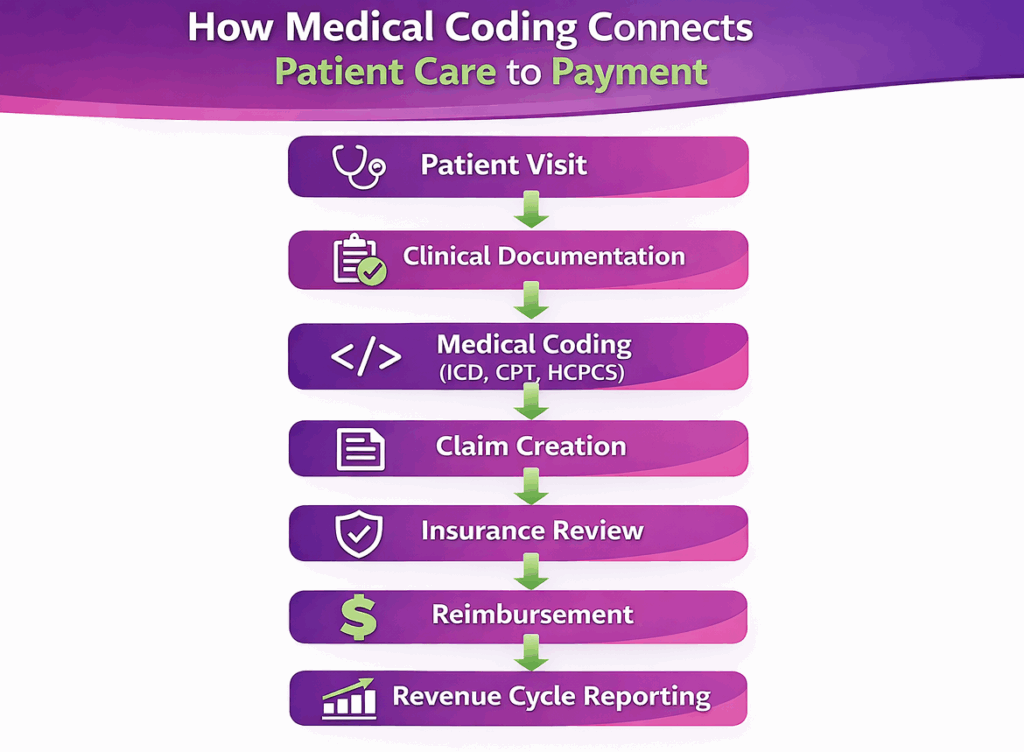
What is the Role of Medical Coding in the Medical Billing Process?
The role of medical coding in the medical billing process is to provide standardized codes that represent medical diagnoses, procedures, and healthcare services for claim submission. Medical coding converts clinical documentation into code formats required by insurance companies and government healthcare programs.
What is the Primary Purpose of Medical Coding?
The primary purpose of medical coding is to translate clinical documentation into standardized alphanumeric codes that represent diagnoses, procedures, and healthcare services. These codes create a uniform method for recording medical information across healthcare systems. Medical coding ensures that healthcare services provided to patients are accurately captured in coded form for consistent documentation and reporting.
What Does RVU Stand for in Medical Coding?
RVU stands for Relative Value Unit. In medical coding, an RVU is a standardized value assigned to medical procedures and services to represent their relative complexity, time, skill, and resources required to perform them. RVUs are used to quantify medical services in a uniform way within healthcare coding systems.
What is Risk Adjustment in Medical Coding?
Risk adjustment in medical coding is the process of capturing and coding patient diagnoses to reflect the severity of illness and the overall health status of a patient. It ensures that coded medical data accurately represents patient conditions in standardized coding systems. Risk adjustment relies on precise diagnosis coding to classify patients based on their health risks.
What is HCC in Medical Coding?
In medical coding, HCC (Hierarchical Condition Category) is a risk adjustment model that groups specific diagnosis codes into categories representing chronic or serious medical conditions. HCCs are used to classify patient health conditions based on coded diagnoses in standardized medical coding systems.
What Are the Top Medical Coding Companies in USA?
The top medical coding companies in the USA include Transcure, The Coding Network, and Omega Healthcare. These companies provide professional medical coding services to healthcare organizations to support accurate clinical documentation coding.
What is E/M in Medical Coding?
In medical coding, E/M or Evaluation and Management refers to a category of codes used to represent patient evaluation and management services provided by healthcare professionals.
What is an Add-On Code in Medical Coding?
An add-on code in medical coding is a medical code used to report a procedure that is performed in addition to a primary service. Add-on codes cannot be used alone and are always reported alongside the main procedure code.
What is a Modifier in Medical Coding?
A modifier is a two-character code added to a procedure code to provide additional information about the service performed. Modifiers indicate that a service was altered, performed under specific circumstances, or provided in a particular manner without changing the core procedure.
What Does AAPC Stand for in Medical Coding?
AAPC stands for the American Academy of Professional Coders. It is a professional organization that provides training, certification, and resources for medical coders, billers, and other healthcare revenue cycle professionals.
What Is Auditing in Medical Coding?
Auditing in medical coding is the process of reviewing coded medical records to ensure accuracy, compliance, and adherence to official coding guidelines. Medical coding audits help identify errors, improve coding quality, and ensure that claims are correctly submitted for reimbursement.
What Does a Medical Coding Auditor Do?
A medical coding auditor reviews medical records and assigned codes to ensure accuracy, compliance with coding guidelines, and proper documentation. They identify coding errors, verify that diagnoses and procedures are correctly coded, and provide feedback to improve coding quality and claim accuracy.
What Does Sequela Mean in Medical Coding?
In medical coding, sequela refers to a condition that is a direct result or complication of a previous disease or injury. Sequela codes are used to report the lasting effects or residual conditions that arise after the initial illness or injury has resolved.
Which Problems Do Bundling and Unbundling Solve in Medical Coding?
Bundling and unbundling in medical coding address problems related to correct procedure reporting and accurate reimbursement.
Bundling solves the problem of reporting multiple procedure codes separately when they are considered a single comprehensive service. It prevents duplicate billing for services already included in a primary procedure code.
Unbundling solves the problem of underreporting services by allowing separate codes for procedures that are distinct and not included in a bundled code.
Both practices ensure accurate claim submission and proper representation of performed medical services.
What Is Bundling in Medical Coding?
Bundling in medical coding is the practice of combining multiple related procedures into a single comprehensive code when those procedures are considered part of one main service. Bundling ensures that services included in a primary procedure code are not reported separately.
What Is Unbundling in Medical Coding?
Unbundling in medical coding is the practice of reporting separate procedure codes for services that are distinct and not included in a comprehensive bundled code. Unbundling makes sure that independently performed procedures are accurately represented in coding.
What Is an Encoder in Medical Coding?
An encoder in medical coding is a software tool that assists coders in selecting appropriate medical codes based on clinical documentation. Encoders help streamline the coding process by providing code search functions and coding guideline references.
What Is the Tabular List in Medical Coding?
The tabular list in medical coding is a structured section of a coding manual that organizes diagnosis or procedure codes in numerical order with detailed descriptions and coding instructions. The tabular list provides official guidelines and notes that direct correct code selection.
What Is NOS in Medical Coding?
In medical coding, NOS stands for Not Otherwise Specified. NOS is used when clinical documentation does not provide enough detail to assign a more specific code.
What Are Medical Coding Types?
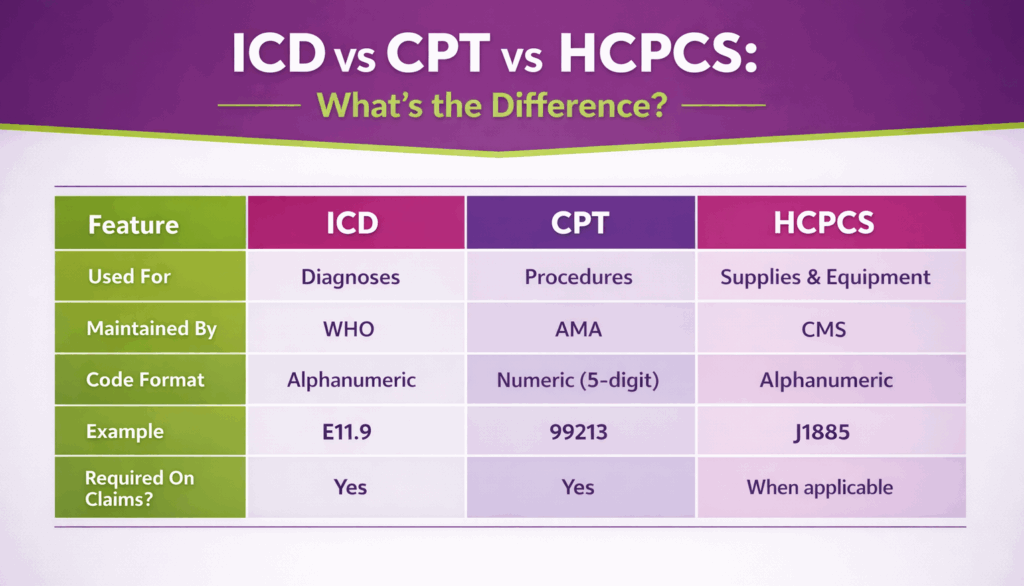
The main types of medical coding are ICD, CPT, and HCPCS. These coding types standardize clinical information across healthcare systems.
1. ICD
The International Classification of Diseases (ICD) is a standardized medical coding system used to classify and code diagnoses, diseases, and health conditions recorded in clinical documentation.
ICD has multiple versions used in healthcare systems. ICD-10 is the current version widely used for diagnosis coding, offering a detailed classification of medical conditions. ICD-11 is the latest version developed to provide updated disease classifications and improved digital compatibility for modern healthcare systems.
2. CPT
Current Procedural Terminology (CPT) is a standardized medical coding system used to report medical procedures, services, and treatments performed by healthcare providers.
CPT codes are organized into three categories. Category I codes represent commonly performed medical procedures and services. Category II codes are used for performance measurement and quality tracking. Category III codes represent temporary codes for emerging technologies, services, and procedures.
3. HCPCS
The Healthcare Common Procedure Coding System (HCPCS) is a standardized medical coding system used to report medical supplies, durable medical equipment, non-physician services, and outpatient procedures not included in CPT.
HCPCS has two main levels. Level I codes consist of CPT codes used for medical procedures and physician services. Level II codes are used to identify medical supplies, equipment, and services not covered by CPT.
Why Is Medical Coding Important?
Medical coding is important because it ensures accurate translation of clinical documentation into standardized codes, enabling correct billing, reimbursement, and healthcare data reporting. Proper coding supports compliance with regulations, reduces errors in claims, and helps healthcare organizations maintain financial and operational efficiency.
Accurate Billing and Reimbursement
Medical coding ensures that healthcare providers are reimbursed correctly for the services and procedures they perform. Accurate codes prevent claim denials and reduce delays in payment.
Regulatory Compliance
Medical coding helps healthcare organizations comply with national and international coding standards, insurance requirements, and legal regulations, minimizing the risk of audits and penalties.
Healthcare Data Reporting and Analysis
Medical coding enables consistent collection of clinical and administrative data, supporting patient care analysis, public health reporting, and research.
Revenue Cycle Efficiency
By standardizing documentation and coding, medical coding streamlines the revenue cycle, reduces errors, and improves the overall efficiency of medical billing operations.
What is the Medical Coding Process?
The medical coding process is a series of steps followed to translate clinical documentation into standardized codes accurately and consistently. It ensures correct billing, compliance with coding rules, and proper representation of healthcare services.
1. Review Medical Documentation
The first step in medical coding is reviewing clinical documentation, including physician notes, lab reports, operative reports, and discharge summaries. Coders examine all relevant records to understand the patient’s diagnosis and procedures performed.
Important Rules:
- Only code what is documented.
- Ensure documentation is complete and legible.
- Follow official coding guidelines for the chosen coding system (ICD, CPT, or HCPCS).
2. Identify Key Information
After reviewing the records, coders extract the key elements required for accurate coding, such as diagnoses, procedures, patient demographics, and service dates.
Important Rules:
- Use exact terminology from the medical record.
- Avoid assumptions; do not code undocumented services.
- Determine if codes require modifiers or special instructions.
How to Abstract Medical Records for Coding?
To abstract medical records, coders identify and highlight relevant information such as primary and secondary diagnoses, procedures performed, and relevant clinical notes. This extracted data forms the basis for accurate code assignment.
3. Assign the Appropriate Codes
Once key information is identified, coders assign the correct codes from ICD, CPT, or HCPCS based on the documentation. This step ensures services and diagnoses are accurately represented in the billing claim.
Important Rules:
- Follow official coding manuals and updates.
- Apply modifiers, add-on codes, or E/M codes correctly when required.
- Check for bundling or unbundling rules to prevent overcoding or undercoding.
- Ensure risk adjustment codes (like HCC) are included if applicable.
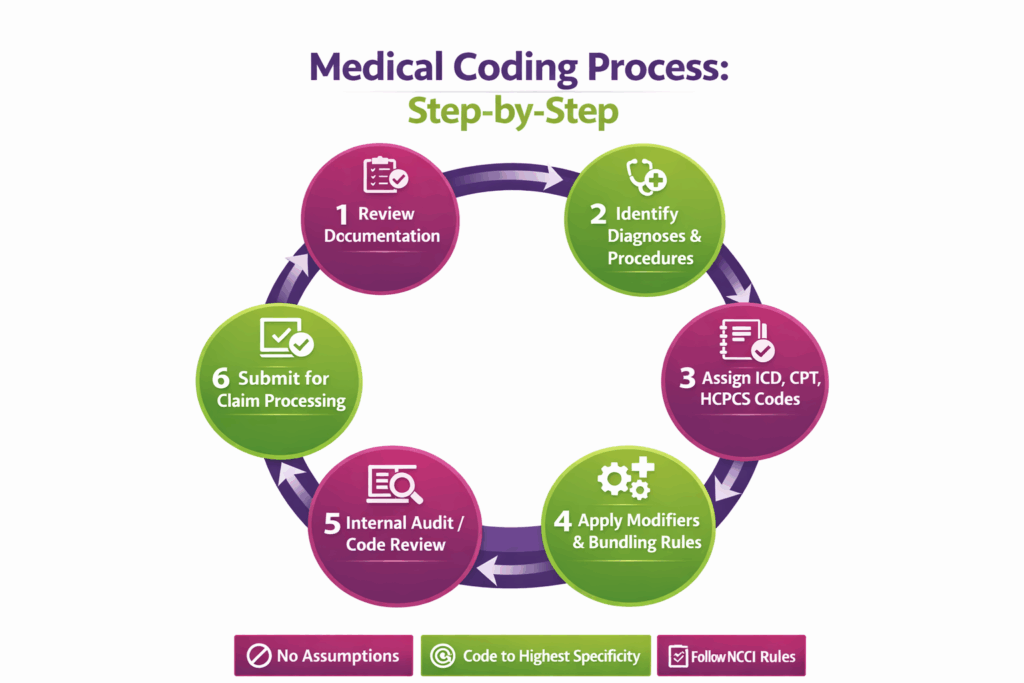
What Happens After Assigning Codes?
After assigning the appropriate codes, the coded data is reviewed and verified for accuracy before it is used in the medical billing process.
Next Steps Include:
- Code Review/Audit: Codes are checked for accuracy, completeness, and compliance with coding guidelines. Errors or inconsistencies are corrected before claim submission.
- Claim Preparation: Verified codes are used to create insurance claims, ensuring proper linkage between diagnosis, procedures, and patient information.
- Submission for Reimbursement: Claims are submitted to insurance companies or government programs for payment. Accurate coding reduces claim denials and delays.
- Record Maintenance: Coded data is stored in medical records for regulatory compliance, reporting, and future reference.
These steps ensure that medical coding supports accurate billing, proper reimbursement, and reliable healthcare data management.
What Are Medical Coding Rules?
Medical coding rules are standardized guidelines that govern how diagnoses, procedures, and healthcare services must be coded. These rules ensure that medical codes are assigned accurately, consistently, and in compliance with official coding standards.
Medical coding rules guide coders in correct code selection, documentation interpretation, and proper reporting practices.
Follow Official Coding Guidelines
Medical codes must be assigned according to the official guidelines published for ICD, CPT, and HCPCS. Coders are required to follow annual updates, notes, and instructions provided in coding manuals.
Code to the Highest Level of Specificity
Medical coding rules require coders to assign the most specific code supported by the clinical documentation. Vague or unspecified codes should be avoided when detailed information is available.
Do Not Code Unsubstantiated Information
Coders must only assign codes based on documented diagnoses and procedures. Assumptions, suspected conditions, or undocumented services must not be coded.
Apply Bundling and Modifier Rules Correctly
Medical coding rules define when procedures should be bundled and when modifiers or add-on codes are allowed. Proper application prevents overcoding and undercoding.
Ensure Documentation Supports the Codes
Every assigned code must be supported by clear and complete medical documentation. Coding without proper documentation violates coding compliance standards.
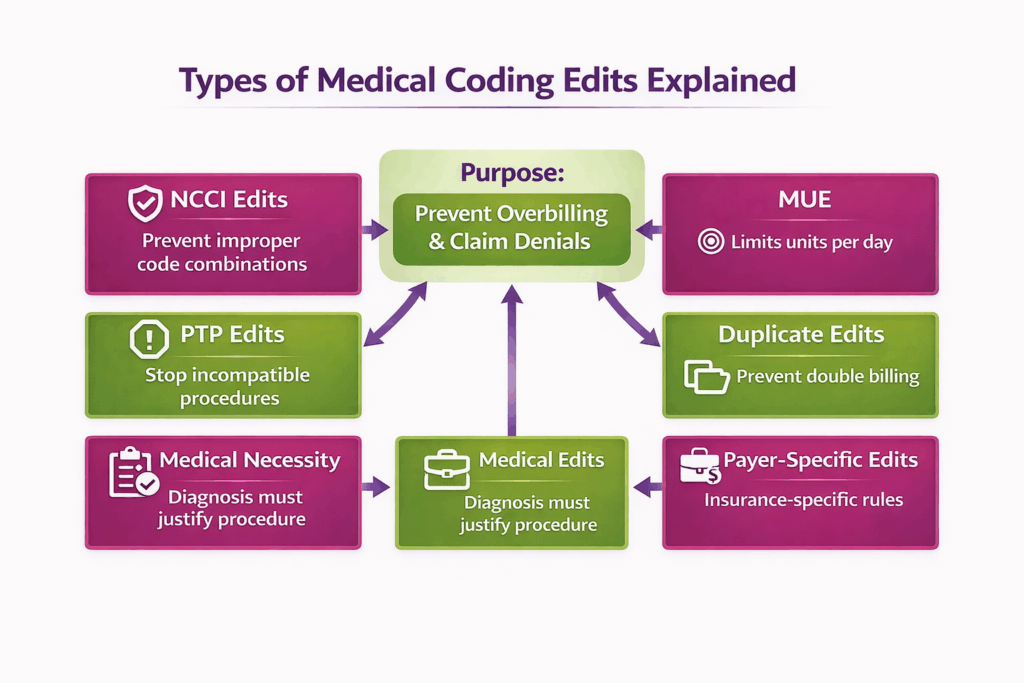
What Are Edits in Medical Coding?
Edits in medical coding are automated or manual checks applied to coded claims to ensure accuracy, compliance, and proper reimbursement. Edits detect coding errors, inconsistencies, or potential claim denials before submission.
What Are NCCI Edits in Medical Coding?
NCCI (National Correct Coding Initiative) edits are coding rules that define which procedure code combinations are allowed or disallowed when reported together. They identify mutually exclusive or bundled services to reduce the risk of overbilling.
What Are Procedure-to-Procedure (PTP) Edits in Medical Coding?
PTP edits are checks that flag when two procedure codes are reported together in a way that is not allowed. They help ensure that only legitimately distinct procedures are billed separately.
What Are Medically Unlikely Edits (MUEs) in Medical Coding?
MUEs set limits on the maximum units of a procedure code that can be reported for a single patient on one day. They prevent overreporting or duplicate services.
What Are Medical Necessity Edits in Medical Coding?
Medical necessity edits verify that the services or procedures billed are clinically justified for the patient’s diagnosis. They ensure claims meet payer and regulatory requirements.
What Are Duplicate Claim Edits in Medical Coding?
Duplicate claim edits detect when the same service or procedure has been billed more than once for a patient. They prevent multiple payments for the same service.
What Are Policy/Payer-Specific Edits in Medical Coding?
Policy or payer-specific edits are rules applied by insurance companies or healthcare programs to enforce their individual coverage policies, billing rules, and limitations on procedures or services.
What Are the Benefits of Outsourcing Medical Coding?
Outsourcing medical coding provides healthcare organizations with access to professional coding expertise while reducing administrative burden. It ensures accurate coding, timely claim submission, and compliance with coding standards.
- Improved Accuracy and Compliance: Outsourced coding teams consist of certified coders who follow official coding guidelines, reducing errors, claim denials, and regulatory risks.
- Cost and Time Efficiency: Outsourcing eliminates the need to hire and train in-house coders, saving payroll costs and allowing staff to focus on patient care.
- Faster Revenue Cycle: Professional coding services speed up claim processing and submission, leading to quicker reimbursement and improved cash flow.
- Access to Specialized Expertise: Outsourced coding teams often have experience across multiple specialties, ensuring accurate coding for complex procedures and diagnoses.
- Scalability: Outsourcing allows healthcare organizations to handle fluctuating workloads without overstaffing, providing flexibility during peak periods or growth.
How Much Does Hiring a Medical Coding Expert Cost?
The cost of hiring a medical coding expert in the USA depends on whether the coder is employed in‑house, contracted, or hired through a service. The annual cost of salaries for medical coders typically ranges broadly:
- Entry to average level coders cost roughly $45,000 to $65,000 per year.
- Some sources report average annual salary costs of around $50,000 to $60,000.
- Certified or experienced coders, especially in specialized roles, can cost $70,000 to $100,000+ per year.
In hourly terms, medical coders generally cost about $20 to $35 per hour, with higher rates for certified or specialized work. Actual cost varies based on experience, certification level, employment type, and regional market conditions.
Does Medical Coding Help in Getting Payments From Insurance?
Yes, medical coding is essential for obtaining payments from insurance providers. Accurate coding translates clinical documentation into standardized codes that insurers recognize for claim processing.
Proper medical coding ensures that claims are correctly submitted, reduces denials or delays, and helps healthcare providers receive timely and appropriate reimbursement for services rendered.
What Are Common Codes in Medical Coding?
Common codes in medical coding are frequently used diagnosis and procedure codes that represent typical medical conditions and services. Examples include:
| Code Type | Code | Description |
|---|---|---|
| ICD-10 | E11.9 | Type 2 diabetes mellitus without complications |
| I10 | Essential (primary) hypertension | |
| J06.9 | Acute upper respiratory infection, unspecified | |
| M54.5 | Low back pain | |
| F32.9 | Major depressive disorder, single episode, unspecified | |
| CPT | 99213 | Office/outpatient visit for an established patient, moderate complexity |
| 93000 | Electrocardiogram (ECG/EKG) with interpretation | |
| 90471 | Immunization administration | |
| 80053 | Basic metabolic panel | |
| 36415 | Collection of venous blood by venipuncture | |
| HCPCS | A0427 | Ambulance service, ALS, non-emergency |
| E0114 | Crutches, underarm, adjustable, pair | |
| J1885 | Injection, ketorolac tromethamine, per 15 mg | |
| L1832 | Elastic stockings, knee-high, off-the-shelf | |
| G0008 | Administration of influenza vaccine |
Understanding these codes is essential in medical billing, which is the process of submitting and following up on claims with health insurance companies to receive payment for services rendered.
Do Medical Codes Vary by Specialty?
Yes, medical codes vary by specialty because different healthcare fields perform distinct procedures and treat specific conditions.
For example:
- Cardiology uses codes for ECGs, stress tests, and heart procedures.
- Orthopedics uses codes for joint repairs, fractures, and imaging procedures.
- Dermatology uses codes for skin biopsies, lesion removals, and topical treatments.
Specialty-specific codes ensure accurate representation of services, proper billing, and compliance with coding guidelines for each area of medicine.
What Are the Most Common Denial Codes in Medical Billing?
Most common denial codes in medical billing indicate why an insurance claim was rejected or denied. Examples include:
- CO-50: Incorrect coding; the code is invalid or does not match the procedure/service
- CO-97: The service is not covered by the payer’s policy
- CO-16: Claim/service lacks information or documentation
- CO-18: Duplicate claim/service submitted
- CO-119: Benefit maximum for the service has been reached
These denial codes help healthcare providers identify issues, correct claims, and resubmit for proper reimbursement.
What Is the Difference Between Medical Coding and Medical Billing?
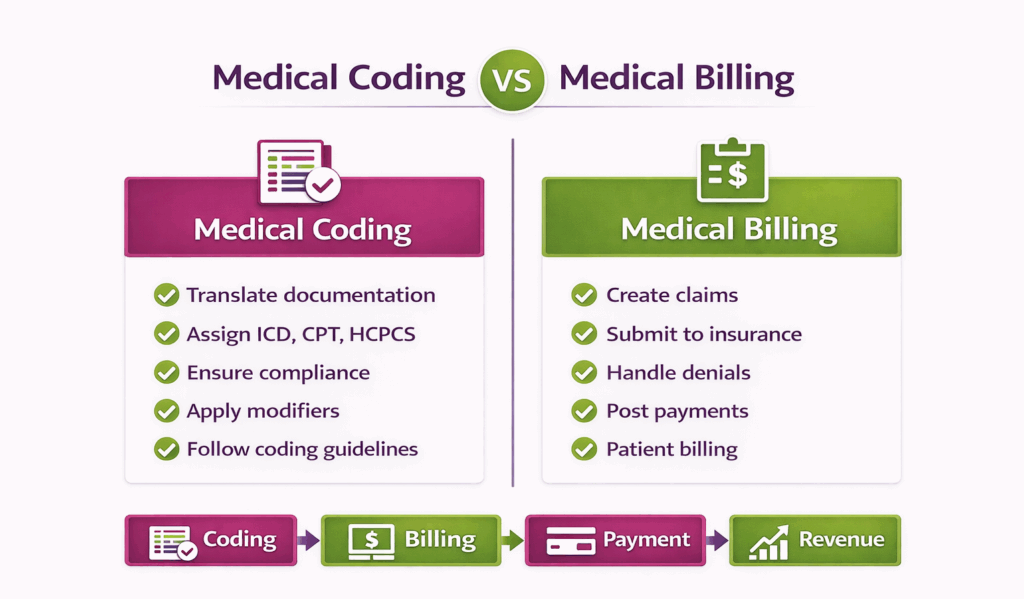
Medical coding and medical billing are related but distinct processes in healthcare revenue management.
Medical Coding involves translating clinical documentation, diagnoses, procedures, and services into standardized alphanumeric codes (ICD, CPT, HCPCS). It ensures accurate representation of patient care for claims and recordkeeping.
Medical Billing uses these codes to prepare and submit claims to insurance providers or government programs for reimbursement. Billing also involves following up on claim status, handling denials, and managing payments.
In short, coding focuses on accurate documentation and coding, while billing focuses on claim submission and payment collection.







