Medical billing software is a digital solution that manages the entire healthcare billing and reimbursement lifecycle. It organizes patient registration, insurance verification, clinical documentation, coding, charge entry, claim creation, submission, payment posting, and reporting within a structured workflow. By automating administrative and financial tasks, it reduces manual errors and improves operational efficiency.
The system works by capturing patient demographics and insurance details, verifying eligibility, translating documented services into standardized codes, and electronically submitting them to payers. It then tracks claim status, manages denials, posts payments, and produces financial reports for revenue monitoring.
There are several types available, including stand-alone billing software, integrated billing with EHR and practice management systems, and cloud-based solutions that allow remote access. Key benefits include faster reimbursements through clean claim submission, reduced billing errors with automated checks, and improved financial visibility using real-time dashboards and analytics.
Selecting the best medical billing software depends on practice size, specialty needs, integration requirements, and long-term scalability goals. This guide will give you detail about the medical billing software types and uses, as well as give you tips on choosing the best one for your requirements.
Table of Contents
ToggleWhat is Medical Billing Software?
Medical billing software is a digital platform to manage the complex financial workflows of healthcare practices. It automates tasks such as patient registration, insurance verification, coding, claim generation, and payment tracking.
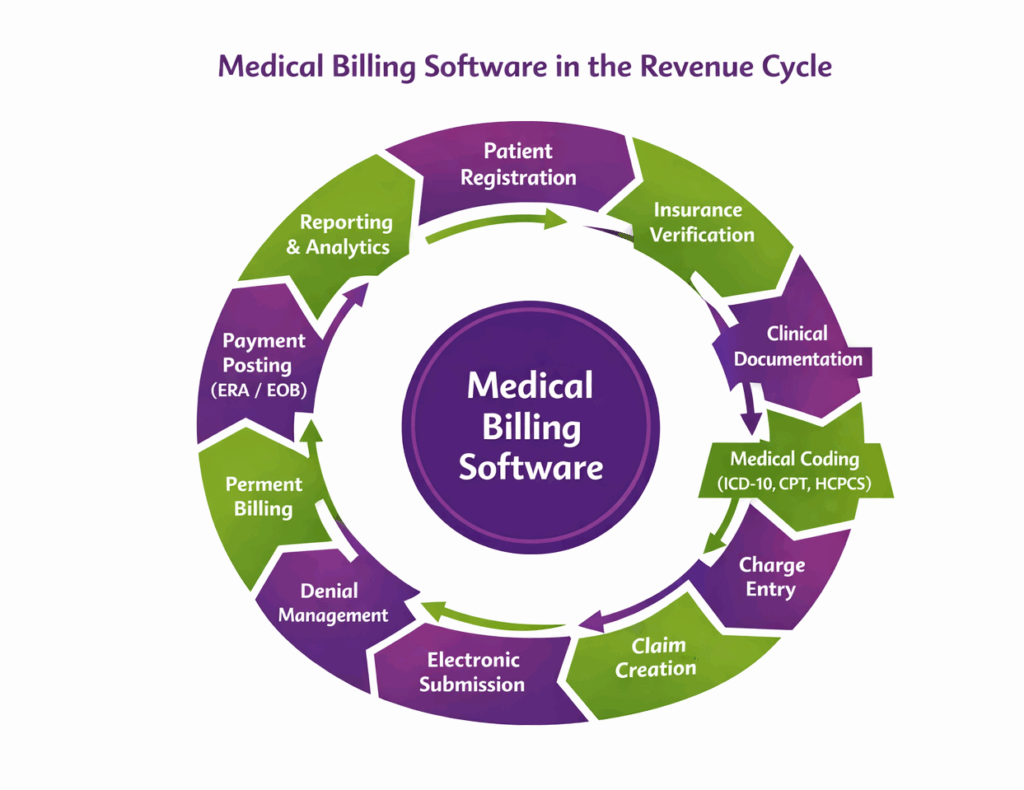
By integrating with medical coding software and medical invoice software, it ensures accurate translation of clinical services into billable codes and generates clean claims. Many vendors offer a medical billing software demo to help practices explore features and usability before implementation, so that they can select the right solution for their needs.
How Does Medical Billing Software Work?
Medical billing software works in a structured workflow that automates the entire revenue cycle of a healthcare practice. It starts from patient registration and insurance entry to claim submission and revenue tracking. Here’s a detailed overview of its workflow:
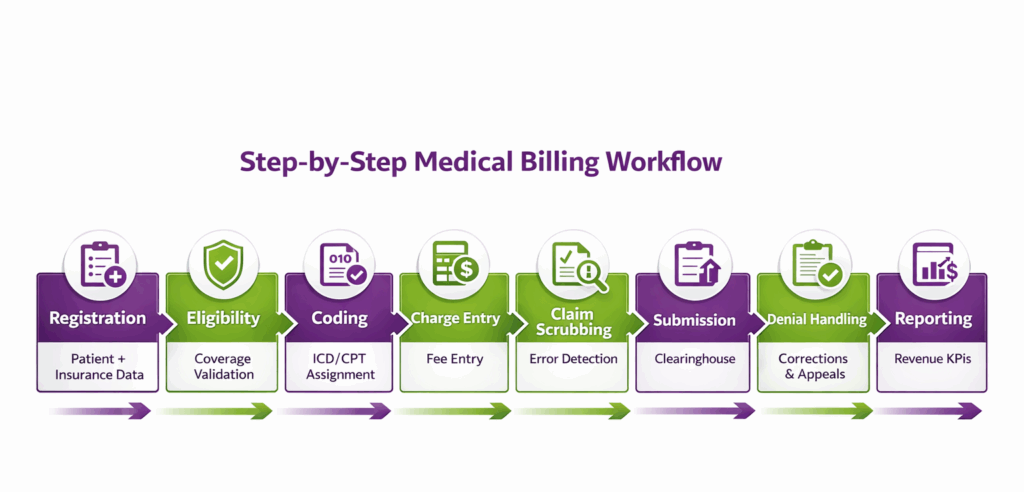
Patient Registration
Patient registration is the process of collecting a patient’s personal and insurance information when they first visit a healthcare practice. This includes demographics, contact details, and insurance policy data.
Accurate data entry is important for making clean claims and reducing billing errors. During registration, the software also performs insurance verification and coverage validation to ensure the patient’s benefits are active and applicable for the services to be provided.
Insurance Entry
After patient registration, the software performs insurance entry that is the process of recording a patient’s insurance policy details into the medical billing software. This includes the payer information, policy number, group number, and coverage specifics. The software uses this data to link claims with the correct insurance provider, verify benefits, and ensure accurate billing.
Eligibility Verification
Once the insurance details are added into the billing software, patient’s active insurance coverage and specific benefits are confirmed before services are provided. In medical billing software, this is done electronically by checking the payer’s database for coverage status, co-pays, deductibles, and service limitations.
Clinical Documentation
In the next step, patient’s diagnoses, treatments, and procedures during healthcare visits are documented. Then, medical billing software takes this information and translates it into standardized ICD-10, CPT, or HCPCS codes, while adhering to payer requirements and regulatory guidelines.
Medical Coding
At this stage, the clinical documentation is converted into standardized codes such as ICD-10, CPT, or HCPCS. In medical billing software, coding ensures accurate claim generation, facilitates proper reimbursement, and helps maintain compliance with payer and regulatory requirements.
Charge Entry
As the codes are assigned, all billable medical services provided to a patient are put into the billing system. Here, each procedure is linked to the appropriate fee schedule, and charges are captured directly from clinical data to ensure accurate billing.
Claim Creation and Claim Scrubbing
After charge entry, the next step is claim creation. At this phase, the software generates insurance-ready claims from the recorded services and codes. Claim scrubbing then reviews these claims for errors and applies payer-specific rules and edits to ensure clean claims before submission.
Electronic Claim Submission
Next, insurance claims are submitted digitally to payers through the medical billing software. The software passes the generated claims through a clearinghouse. That reviews, formats, and forwards them to the appropriate insurance company.
Denial Management
In case the claims are denied from the insurers, the medical billing software identifies the reason behind for denial and auto-corrects it. After correcting the errors, the claims are resubmitted to ensure timely reimbursements.
Payment Posting
At this stage, payments got from insurers and patients are recorded into the medical billing software. The system uses Explanation of Benefits (EOBs), which detail what the insurer paid, denied, or adjusted, and Electronic Remittance Advices (ERAs) to match payments with the corresponding claims.
Patient Billing and Statements
When the insurer’s portion of the payment is posted, any remaining balance owed by the patient is billed. The medical billing software generates clear statements and invoices that have details about the charges, payments received, and outstanding amounts. This makes it easy for patients to understand and pay their bills on time.
Reporting and Revenue Tracking
The last stage is the reporting and revenue tracking. The medical billing software generates financial reports, which track key performance indicators (KPIs) and metrics. Those include AR days, claim denial rates, and charge capture rate.
What are the Types of Medical Billing Software?
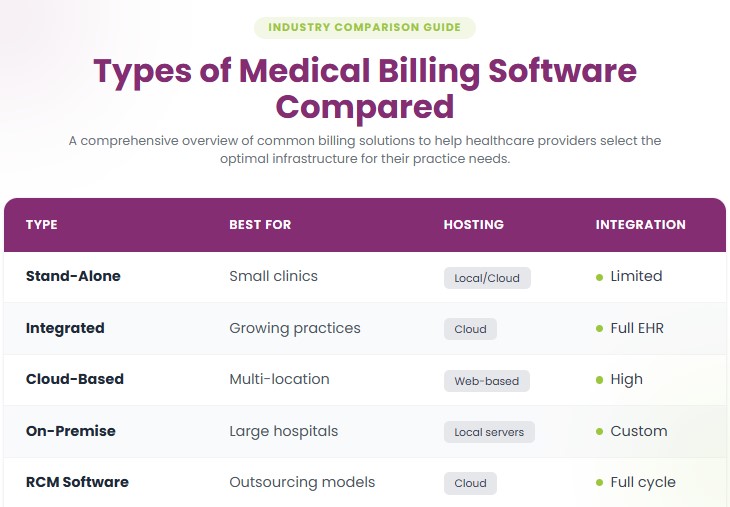
The types of medical billing software serve different purposes. They range from stand-alone billing software to EHR-integrated systems, cloud-based platforms, on-premise solutions, and specialty-specific or small-practice software. Here’s a description of each software in detail:
Stand-Alone Medical Billing Software
Stand-alone medical billing software is a billing-focused system that operates independently without deep integration with EHR systems. This software supports standalone billing workflows and includes key features such as claim management, payment posting, patient billing, reporting, and basic insurance verification.
Integrated Medical Billing Software
Integrated medical billing software integrates medical billing services with other features, such as appointment scheduling, EHRs, and patient management. This software helps manage all aspects of practice operations from a single platform.
Cloud-Based Medical Billing Software
Cloud-based medical billing software offers web-accessible solutions that automate revenue cycle management, claims processing, and patient payments. It is hosted on a secure cloud infrastructure that lets providers access billing systems anytime and from anywhere.
On-Premise Medical Billing Software
On-premise medical billing software is installed locally on servers and computers of the healthcare organization. It is hosted and managed by the clinic’s own IT staff. This software provides full ownership and control over all data and systems.
Revenue Cycle Management (RCM) Software
Revenue Cycle Management (RCM) software is a healthcare financial technology that manages and automates the entire healthcare billing process. It supports end-to-end RCM services, starting from patient registration to final payment collection.
Specialty-Specific Billing Software
Specialty-Specific Billing Software is a customized medical billing system designed to meet the unique coding, documentation, and compliance needs of specific medical specialities. It offers tailored workflows and incorporates specialty-specific CPT and ICD coding rules. Doing so ensures accurate claim submission and compliance with payer guidelines for that field.
Small Practice Billing Software
Small practice billing software is made specifically for solo providers and small clinics with limited administrative staff. It makes billing, claims management, and payment tracking easier with simple interfaces and streamlined workflows.
Medical Accounting and Billing Software
Medical accounting and billing software combines healthcare billing functions with essential accounting capabilities in a single system. It manages invoicing, insurance claim processing, and expense tracking, providing complete financial oversight for healthcare practices.
What are the Benefits of Medical Billing Software?
There are multiple benefits of medical billing software. For example, it accelerates payments by reducing claim submission delays and reducing billing errors. Let’s have a look at each benefit in detail below:
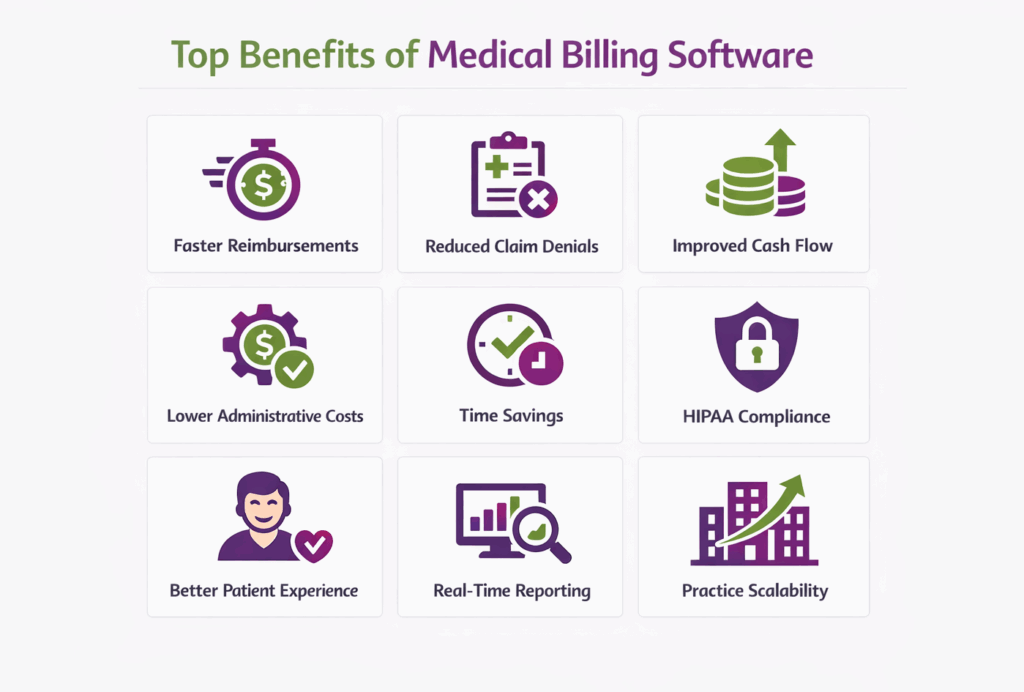
Accelerates Payments
Payment acceleration refers to speeding up the reimbursement process within the revenue cycle. Medical billing software enables faster reimbursements from payers by reducing claim submission delays, automating workflows, and ensuring clean claims are processed without unnecessary rejections.
Reduces Billing Errors
Billing errors include incorrect patient information, inaccurate coding, missing documentation, or incomplete claims that lead to denials or delays. Medical billing software helps reduce these errors by minimizing human and coding mistakes through automated claim scrubbing, real-time validation checks, and built-in compliance rules before submission.
Saves Time and Costs
Medical billing software automates repetitive billing tasks such as claim generation, eligibility checks, and payment posting. Since the tasks are automated, it reduces the administrative workload and operational expenses within a healthcare practice. This leads to both time and cost savings that support better cost control across the revenue cycle.
Improves Financial Visibility
With the help of medical billing software, you get real-time insights into revenue, collections, and outstanding balances. On top of that, interactive dashboards and performance metrics allow practices to monitor cash flow, track claim status, and analyze denial trends.
Ensures Compliance and Security
Medical billing software ensures compliance and security by helping practices follow HIPAA and other healthcare regulations. It protects sensitive patient data through encryption, and secure user authentication. This reduces the risk of data leaks and supports effective risk management across the organization.
Enhances Patient Experience
Medical billing software enhances patient experience by promoting clear billing communication and financial transparency. It generates easy-to-understand statements, provides accurate breakdowns of charges, and offers convenient payment options, helping patients feel informed and confident about their healthcare expenses.
Streamlines System Integration
By integrating with EHR, practice management, and accounting systems, medical billing software ensures that data flows seamlessly across all platforms. This connectivity automates workflows, reduces manual errors, and enhances overall operational efficiency within the practice.
Supports Practice Scalability
Medical billing software supports practice scalability by adapting to growing patient volumes and expanding operational needs. Its modular features and flexible user management allow practices to add new providers, departments, or services without disrupting existing workflows.
Leverages Data Insights
By analyzing financial and operational data, medical billing software provides actionable insights that help practices improve performance. Advanced reporting tools and predictive analytics enable optimization of revenue cycles, identification of inefficiencies, and informed decision-making for future growth.
How to Choose the Right Medical Billing Software?
To choose the right medical billing software, it’s important to evaluate your practice needs, workflow requirements, and long-term goals. Medical billing involves converting clinical services into standardized codes and submitting claims to insurance companies and other payers to secure proper reimbursement for healthcare providers. Here are the key steps to guide your selection:

- Understand Your Practice Requirements: Assess the size, specialty, and specific workflow needs of your practice.
- Identify Essential Medical Billing Features: List must-have features such as claim management, payment posting, reporting, and patient billing.
- Evaluate Billing and Claims Management Capabilities: Ensure the software efficiently handles claim creation, scrubbing, submission, and denial management.
- Assess Insurance and Eligibility Verification Tools: Verify that coverage checks and payer-specific rules are supported.
- Review Reporting and Revenue Analytics: Check for dashboards, KPIs, and financial insights to monitor revenue performance.
- Check EHR and Practice Management Integration: Ensure smooth data flow between billing, EHR, and other administrative systems.
- Ensure Security, Compliance, and HIPAA Standards: Confirm encryption, access controls, and adherence to healthcare regulations.
- Compare Cloud-Based vs On-Premise Solutions: Evaluate deployment models based on accessibility, scalability, and IT infrastructure.
- Analyze Ease of Use and Staff Adoption: Consider user-friendly interfaces and training requirements for smooth adoption.
- Review Vendor Support and Training Options: Assess customer service, technical support, and training resources.
- Evaluate Pricing Structure and Return on Investment: Compare subscription fees, licensing costs, and long-term ROI.
- Verify Data Protection and Backup Measures: Ensure secure backups, disaster recovery, and data integrity.
- Research Software Reviews and Vendor Reputation: Check user feedback, testimonials, and industry reputation.
- Request a Demo or Free Trial: Test the software firsthand to ensure it meets your practice’s needs.
Is There Free Medical Billing Software?
Yes, there are free medical billing software options available, often designed for small practices or startups with basic billing needs. While these free solutions can handle simple claim submission, patient billing, and reporting, they may have limited features compared to paid versions. Practices should carefully evaluate whether a free solution meets their long-term needs before using it.
Why Is Denial Management Important in Medical Billing Software?
Denial management is important in medical billing software because it plays an important role within RCM by identifying and resolving denied claims. The software automates denial identification, categorization, and resubmission to ensure timely reimbursements. In the United States, the average denial rates for all payers often fall around 10 – 15 %, with some practices experiencing denial rates of 20 % or higher. These high rates show the importance of an efficient denial management process.
How Does EMR Software Improve the Medical Billing Process?
EMR software improves the medical billing process by streamlining documentation, coding, and claims management. Key ways it enhances billing efficiency include:
- Accurate Charge Capture: Automatically records all billable services provided during patient visits.
- Reduced Coding Errors: Supports proper ICD, CPT, and HCPCS coding to reduce the chances of coding mistakes.
- Faster Claims Submission: Generates and submits claims electronically without delays.
- Fewer Claim Denials: Ensures clean claims by verifying data and adherence to payer rules.
- Real-Time Eligibility and Authorization Verification: Confirms patient coverage and required authorizations before services are delivered.
- Improved Documentation Compliance: Maintains thorough and accurate clinical records to meet payer and regulatory requirements.
- Integration of EMR and Billing Systems: Enables smooth data flow between clinical and billing modules, which reduces the chances of duplicate entries.
- Enhanced Revenue Cycle Visibility and Reporting: Provides dashboards and metrics for monitoring claim status, revenue, and performance.
- Improved Patient Billing Experience: Generates clear statements and facilitates easy payment options.
- Time and Cost Efficiency: Reduces administrative workload and operational costs by automating repetitive billing tasks.







